Chapter 4 of 4.
Patient Teaching: A Guide to Oral Health for Seniors
Oral Health and Older Adults
People are living longer and healthier lives. And, older adults also are more likely to
keep their teeth for a lifetime than they were a decade ago. Growing older often means
adapting to change. Good habits maintained for a lifetime help us cope with change and
help preserve a healthy, quality lifestyle. Your daily brushing and flossing routine and
regular visits to the dentist are strong foundations for good oral and overall health.
Why Older Citizens Don't Seek Dental Care
Unfortunately, many older adults fail to use dental services that are available. There
are several common explanations for this reluctance.
Fear of pain often associated with dental procedures may prevent some older adults
from seeking dental care. This deterrent, however, appears to be less prevalent in the
older adults than those of middle age. Most dental procedures, with the exception of
surgery, can be performed without anesthesia because of the decrease in nerve fibers.
Painless dentistry is more easily accomplished with older adults than any other age group.
Preoccupation with impending death creates a feeling of "since I am old and will
die soon, I do not need dental care." Comfort, function and appearance are important at
any age. These positive aspects of good dental care can often improve the older adult's
psychological outlook.
Cost, unfortunately, is perhaps the greatest single deterrent to those seeking dental
care. Many elderly, because of their low fixed income, feel that they cannot afford dental
care. Medicare, at this time, does not provide for dental care other than hospitalization
for surgical procedures.
How Does Growing Older Affect Oral Health?
The aging process often creates subtle or dramatic changes in the condition of
teeth, mouth and gums. Here are some hard facts to ponder:
Keeping teeth clean and white may become more
involved. The formation of plaque, a colorless layer of bacteria that builds up on teeth, accelerates as we grow older. Teeth
also may darken in color due to changes in dentin, the bone-like tissue underneath
tooth enamel.
Changes in teeth and supporting tissue. Tissues in your mouth, like other body
tissues, change as you grow older. Soft tissues (gums and cheeks) lose their ability to stretch,
and muscles become soft and weak. The amount of saliva produced by glands in your
mouth is frequently reduced. As a result, chewing becomes more difficult, and your
mouth becomes more easily irritated and heals more slowly than when you were younger.
Other changes may occur.
Gums may begin to recede from teeth. This process exposes tooth roots to plaque
and can cause tooth decay. In addition, older fillings may weaken and crack, allowing
bacteria to accumulate around the edges of fillings, causing cavities. Unfortunately, many
individuals over the age of 50 have decay on both teeth and roots which may require
clinical care.
Decay. The rate of tooth decay may be increasing as you grow older. This is
especially true when the amount of saliva is reduced. Tooth decay in older adults appears
most frequently around the teeth at the level of the gums. The root portion of a tooth,
when exposed, is especially subject to decay. Gumline or root decay is difficult to restore
with fillings, because decay often reoccurs around this type of filling soon after it is placed.
Brittleness and wear of teeth. Nerve tissue and blood vessels are found in the pulps
of teeth. When you were young, these nerves were very responsive to pain or to
anything hot or cold. As you have aged, the pulp gradually became smaller with fewer
blood vessels and less nerve tissue supplying the teeth. As a result, your teeth have less
fluid content and have become brittle. Your brittle teeth may be easily broken or
chipped. Fortunately, due to the reduced nerve tissue, little if any pain is experienced when
even severe fractures occur.
Teeth wear because of the grinding action of chewing. Tooth enamel becomes thinner.
In severe cases, the hard enamel covering is completely worn away leaving a softer part
of the tooth (dentin) exposed. Dentin can be dissolved by acidic oral fluids. Teeth with
only a fragile enamel shell may result. These teeth are easily chipped or broken.
"Dry Mouth" may develop. Caused by reduced saliva flow, dry mouth may lead to
tooth damage. Reduced saliva flow may be a medical disorder or a side effect of
medications such as antihistamines, decongestants, pain killers or diuretics. The reduced flow
affects teeth because saliva acts a cleaning agent in the mouth to wash away acids produced
by plaque. When the mouth is not adequately lubricated and moistened by saliva,
plaque forms more quickly and produces cavities.
In addition, dry mouth can cause sore throat, problems with speaking, difficulty
swallowing and hoarseness. Your dentist or periodontist can recommend various methods
to restore moisture, including sugarless gum, oral rinses or artificial saliva products.
Be sure to tell your periodontist and other dental professionals about any medications
that you are taking, including herbal remedies and over-the-counter medications.
Gum disease develops more readily. Bacteria found in sugars and starches create
toxins which irritate the gums and cause gum tissue to separate from teeth. Left untreated,
gum disease can cause unnecessary tooth loss. It also may dissolve the bone that holds
your teeth in place. Poorly fitted dentures, poor oral hygiene, illnesses and some
medications may increase the severity of gum disease and create chewing problems and pain in
the jaw. Fortunately, visiting your dentist regularly can help reduce the spread of gum
disease and its damaging effects.
Oral cancers. The incidence of oral cancer appears to increase with age. About 3
percent of all cancers detected are found in the jaws, lips, tongue and palate (roof of the
mouth). The effect of oral cancers and their treatment can be devastating. Surgical treatment
often results in loss of a portion or all of the jaws, tongue or palate. Facial disfigurement
and serious impairment of chewing ability accompanies treatment of more extensive cancers.
Radiation (x-ray) therapy used to treat some oral cancers generally results in a
reduced amount of saliva. The cleaning and lubricating effect of saliva is diminished,
leaving tissues easily irritated and teeth subject to rapid decay.
Systemic diseases. Evidence of a disease occurring elsewhere in the body is
sometimes noted in the mouth. Disorders such as those of the blood system (anemia) or diabetes
are sometimes accompanied by inflammation and reduced healing capacity of the gums.
What you may not realize is that oral health is not just important for maintaining a
nice-looking smile and being able to eat corn on the cob. Good oral health is essential
to quality of life. Consider a few of the reasons:
The Importance of Toothbrushing
Accumulation of food debris, plaque ( a white residue adhering to the teeth) or
calculus (solidified plaque) increases the rate of tooth decay and gum disease. Good oral
hygiene is perhaps the simplest and most efficient means to promote comfort and help reduce
the dental problems associated with aging.
Toothbrushing for at least 3 minutes will help to remove plaque from the surfaces of
your teeth. Plaque is the leading cause of tooth decay, so by removing it you are helping
to decrease the risk of tooth decay!
Brush daily with a soft toothbrush that is not worn out or frayed. Your toothbrush
needs to be replaced every 3 to 4 months.
Use toothpaste with fluoride in it. The use of topical fluoride, which is seen in
toothpastes, gels and rinses, have been shown to significantly reduce dental cavities. It
is important that young children are closely monitored when using
fluoride-containing products so that they do not ingest an excessive amount. Only a pea-sized amount
of toothpaste is necessary for a child to use.
Eat a balanced meal and limit food that is high in sugar.
Steps for getting the most out of your brushing:
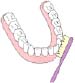
Place the brush against your gum line (where the teeth and gums meet).
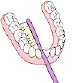
Move the brush back and forth gently with short strokes.
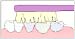
Brush the inner surfaces of your front teeth with the
front part of
your toothbrush.
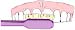
Brush the inner and outer surfaces of all teeth.
The Importance of Flossing
 You floss to remove the plaque from between your teeth and
above and below the gum line - places where your toothbrush can't reach.
You floss to remove the plaque from between your teeth and
above and below the gum line - places where your toothbrush can't reach.
By combining flossing and brushing at the same time every
day, you can thoroughly remove plaque and prevent cavities and
gum disease.
Steps for getting the most out of flossing:
Remove a length of floss about 18 inches long. Wrap most of the floss around the
middle finger of one hand and just a few inches around the middle finger of the other hand.
Hold the floss taut between thumb and forefinger (leave about one inch between
fingers) and guide it gently between the teeth. Do not snap it onto the gums.
Curve the floss into a C shape against the sides of each tooth. Use an up-and-down
scraping motion to remove plaque between teeth and just between the gum line. Do not
floss with a back and forth sawing motion.
As the floss becomes soiled, advance to a clean section of floss and
continue.
Dental Aids
Many mechanical aids have been developed to improve oral hygiene. Some have
practical application for the elderly.
Electrical tooth brushes have been shown to be effective in cleaning teeth. The
larger handle can be held more easily and the mechanical movement of the brush
compensates for those with limited movement.
Water irrigators can be useful in removing particles from between teeth. If you
have pockets between your teeth and gums, use a water irrigator with care. Rather than
being washed away, food particles can be forced into those pockets and can cause severe
irritation.
Interdental cleaners are handles with small changeable brushes. They allow for
cleaning between teeth. This is especially helpful when the gums have receded, creating
large spaces between the teeth.
Oral lubricants can ease some of the problems created by a dry mouth. Glycerine,
flavored with a few drops of lemon, can provide a lubricating effect. This will ease
the irritation caused by dentures rubbing on the underlying tissue or dry cheeks rubbing
on the denture teeth. Several prescription medications are available that can stimulate
the production of saliva or act as a saliva substitute.
Denture Care
Denture care is necessary because wearing dentures does not mean that good oral
hygiene can be neglected. If you wear dentures, they should be removed after eating and
rinsed with warm water. The mouth should also be thoroughly rinsed.
Dentures accumulate calculus like the teeth they replaced. Dentures should be
scrubbed with a stiff brush and cream to remove these deposits. Commercial denture
cleaning solutions by themselves will not adequately clean dentures.
Do-it-yourself denture liners should be avoided. They become rough and irritating
and harbor bacteria and food debris. Such liners are difficult to keep clean.
For more detailed information on any of the dental aids or cleaning procedures,
consult your dentist. Dentists can help establish a routine to provide you with the most
efficient means of cleaning your teeth and gums.
Dental Implants
More and more older people are selecting dental implants over dentures as a
replacement option for lost teeth. Whether you have lost one or all of your teeth, dental implants
allow you to have teeth that look and feel just like your own.
Older adults have similar success rate with implants compared with younger people.
As long as you're in good health and your periodontist can restore healthy gums and
adequate bone to support the implant, you're never too old to receive a dental implant.
A dental implant is an artificial tooth root placed into your jaw to hold a
replacement tooth or bridge in place. While high-tech in nature, dental implants are actually
more tooth-saving than traditional bridgework, since implants do not rely on
neighboring teeth for support.
In addition, dental implants are intimately connected with the gum tissues and
underlying bone in the mouth. Therefore, they prevent the bone loss and gum recession
that often accompanies bridgework and dentures and preserve the integrity of facial
features. When teeth are missing, the bone which previously supported these teeth
begins to deteriorate. This can result in dramatic changes in your appearance, such as
increased wrinkles around the mouth and lips that cave in and lose their natural shape.
Since periodontists are the dental experts who specialize in precisely these areas,
they are ideal members of your dental implant team. Not only do periodontists have
experience working with other dental professionals, they also have the special
knowledge, training and facilities that you need to have teeth that look and feel just like your own.
Talk with your preriodontist to find out if dental implants are an option for you.
Special Concerns for Older Women
Women who are menopausal or post-menopausal may experience changes in
their mouths. Recent studies suggest that estrogen deficiency could place
post-menopausal women at higher risk for severe periodontal disease and tooth loss. Hormonal changes
in older women may result in discomfort in the mouth, including dry mouth, pain and
burning sensations in the gum tissue and altered taste, especially salty, peppery or sour.
In addition, menopausal gingivostomatitis affects a small percentage of women.
Gums that look dry or shiny, bleed easily and range from abnormally pale to deep red mark
this condition.
Most women find that estrogen supplements help to relieve these symptoms.
Bone loss is associated with both periodontal disease and osteoporosis.
Osteoporosis could lead to tooth loss because the density of the bone that supports the teeth may
be decreased. More research is being done to determine if and how a relationship
between osteoporosis and periodontal disease exists. Women considering Hormone
Replacement Therapy (HRT) to help fight osteoporosis should note that this may help protect
their teeth as well as other parts of the body.
Congratulations!! Move on
the the quiz.
Sources:
California Dental Association
The American Academy of Periodontology
University of Missouri
Community & Public Health Administration,
Maryland Department of Health & Mental Hygiene