7.
Drowsy Driving and Automobile Crashes
- Executive Summary
 | Biology of Human Sleep and Sleepiness
 | Crash Characteristics
 | Risks for Drowsy-Driving Crashes
 | Population Groups at Highest Risk
 | Countermeasures
| | | | |
Focusing an Educational Campaign: Panel Recommendations
Introduction
 | Methods and Knowledge Base of This Report
 | Research Needs
| |
Biology of Human Sleep and Sleepiness
 | The Sleep-Wake Cycle
 | Sleepiness Impairs Performance
 | The Causes of Sleepiness/Drowsy Driving
 | Evaluating Sleepiness
| | | |
Characteristics of Drowsy-Driving Crashes
Risk for Drowsy-Driving Crashes
 | Sleep Loss
 | Driving Patterns
 | The Use of Sedating Medications
 | Untreated Sleep Disorders: Sleep Apnea Syndrome and Narcolepsy
 | Consumption of Alcohol Interacts With Sleepiness to Increase Drowsiness and Impairment
 | Interactions Among Factors Increase Overall Risk
| | | | | |
Population Groups at Highest Risk
 | Young People, Especially Young Men
 | Shift Workers
 | People With Untreated Sleep Apnea Syndrome and Narcolepsy
| | |
Countermeasures
 | Behavioral Interventions
 | Medical Interventions to Treat Narcolepsy and Sleep Apnea Syndrome
 | Alerting Devices
 | Shift Work Measures
 | Employer Management of Work Schedules
 | Employee Behavioral Steps
 | Using Bright Light Treatments
| | | | | | |
Focusing an Educational Campaign: Panel Recommendations
 | Educate Young Males About Drowsy Driving and How to Reduce Lifestyle-Related Risks
 | Promote Shoulder Rumble Strips as an Effective Countermeasure for Drowsy-Driving; in this Context, Raise Public Awareness About Drowsy-Driving Risks and How to Reduce Them
 | Educate Shift Workers About the Risks of Drowsy Driving and How to Reduce Them
 | Other Organizations Can Provide Drowsy Driving Education
| | | |
References
|

 Executive Summary
Executive Summary
Drowsy driving is a serious problem that leads to thousands of automobile crashes each year. This report, sponsored by the National Center on Sleep Disorders Research (NCSDR) of the Na-tional Heart, Lung, and Blood Institute of the National Institutes of Health, and the National Highway Traffic Safety Administration (NHTSA), is designed to provide direction to an NCSDR/NHTSA educational campaign to combat drowsy driving. The report presents the results of a literature review and opinions of the Expert Panel on Driver Fatigue and Sleepiness regarding key issues involved in the problem.

Biology of Human Sleep and Sleepiness
Sleep is a neurobiologic need with predictable patterns of sleepiness and wakefulness. Sleepiness results from the sleep component of the circadian cycle of sleep and wakefulness, restriction of sleep, and/or interruption or fragmentation of sleep. The loss of one night's sleep can lead to extreme short-term sleepiness, while habitually restricting sleep by 1 or 2 hours a night can lead to chronic sleepiness. Sleeping is the most effective way to reduce sleepiness.
Sleepiness causes auto crashes because it impairs performance and can ultimately lead to the inability to resist falling asleep at the wheel. Critical aspects of driving impairment associated with sleepiness are reaction time, vigilance, attention, and information processing.

Crash Characteristics
Subjective and objective tools are available to approximate or detect sleepiness. However, unlike the situation with alcohol-related crashes, no blood, breath, or other measurable test is currently available to quantify levels of sleepiness at the crash site. Although current understanding largely comes from inferential evidence, a typical crash related to sleepiness has the following characteristics:
 | The problem occurs during late night/ early morning or mid-afternoon.
 | The crash is likely to be serious.
 | A single vehicle leaves the roadway.
 | The crash occurs on a high-speed road.
 | The driver does not attempt to avoid a crash.
 | The driver is alone in the vehicle.
| | | | | |

Risks for Drowsy-Driving Crashes
Although evidence is limited or inferential, chronic predisposing factors and acute situational factors recognized as increasing the risk of drowsy driving and related crashes include:
 | Sleep loss.
 | Driving patterns, including driving between midnight and 6 a.m.; driving a substantial number of miles each year and/or a substantial number of hours each day; driving in the midafternoon hours (especially for older persons); and driving for longer times without taking a break.
 | Use of sedating medications, especially prescribed anxiolytic hypnotics, tricyclic antidepressants, and some antihistamines.
 | Untreated or unrecognized sleep disorders, especially sleep apnea syndrome (SAS) and narcolepsy.
 | Consumption of alcohol, which interacts with and adds to drowsiness.
| | | | |
These factors have cumulative effects; a combination of them substantially increases crash risk.

Population Groups at Highest Risk
Although no driver is immune, the following three population groups are at highest risk, based on evidence from crash reports and self-reports of sleep behavior and driving performance.
 | Young people (ages 16 to 29), especially males.
 | Shift workers whose sleep is disrupted by working at night or working long or irregular hours.
 | People with untreated sleep apnea syndrome (SAS) and narcolepsy.
| | |

Countermeasures
To prevent drowsy driving and its consequences, Americans need information on approaches that may reduce their risks. The public needs to be informed of the benefits of specific behaviors that help avoid becoming drowsy while driving. Helpful behaviors include (1) planning to get sufficient sleep, (2) not drinking even small amounts of alcohol when sleepy, and (3) limiting driving between midnight and 6 a.m. As soon as a driver becomes sleepy, the key behavioral step is to stop driving—for example, letting a passenger drive or stopping to sleep before continuing a trip. Two remedial actions can make a short-term difference in driving alertness: taking a short nap (about 15 to 20 minutes) and consuming caffeine equivalent to two cups of coffee. The effectiveness of any other steps to improve alertness when sleepy, such as opening a window or listening to the radio, has not been demonstrated.
A more informed medical community could help reduce drowsy driving by talking to patients about the need for adequate sleep, an important behavior for good health as well as drowsy-driving prevention. The detection and management of illnesses that can cause sleepiness, such as SAS and narcolepsy, are other health care-related countermeasures.
Information could be provided to the public and policymakers about the purpose and meaning of shoulder rumble strips, which alarm or awaken sleepy drivers whose vehicles are going off the road. These rumble strips placed on high-speed, controlled-access, rural roads reduce drive-off-the-road crashes by 30 to 50 percent. However, rumble strips are not a solution for sleepy drivers, who must view any wake-up alert as an indication of impairment—a signal to stop driving and get adequate sleep before driving again.
Employers, unions, and shift work employees need to be informed about effective measures they can take to reduce sleepiness resulting from shift work schedules. Countermeasures include following effective strategies for scheduling shift changes and, when shift work precludes normal nighttime sleep, planning a time and an environment to obtain sufficient restorative sleep.

 Focusing an Educational Campaign: Panel Recommendations
Focusing an Educational Campaign: Panel Recommendations
To assist the educational campaign in developing its educational initiatives, the panel recommended the following three priority areas:
- Educate young males (ages 16 to 24) about drowsy driving and how to reduce lifestyle-related risks.
- Promote shoulder rumble strips as an effective countermeasure for drowsy driving; in this context, raise public and policymaker awareness about drowsy-driving risks and how to reduce them.
- Educate shift workers about the risks of drowsy driving and how to reduce them.
The panel also identified complementary messages for the campaigns and called for the active involvement of other organizations in an effort to promote sufficient sleep—as a public health benefit as well as a means to reduce the risk of fall-asleep crashes.

 Introduction
Introduction
In the 1996 appropriations bill for the U.S. Department of Transportation, the Senate Appropriations Committee report noted that "NHTSA data indicate that in recent years there have been about 56,000 crashes annually in which driver drowsiness/fatigue was cited by police. Annual averages of roughly 40,000 nonfatal injuries and 1,550 fatalities result from these crashes. It is widely recognized that these statistics underreport the extent of these types of crashes. These statistics also do not deal with crashes caused by driver inattention, which is believed to be a larger problem."
In response, Congress allocated funds for a public education campaign on drowsy driving among noncommercial drivers, to be sponsored by the National Highway Traffic Safety Administration (NHTSA) and the National Center on Sleep Disorders Research (NCSDR) of the National Heart, Lung, and Blood Institute, the National Institutes of Health. This focus complements Federal Highway Administration efforts to address the problem among commercial vehicle drivers (Federal Register, 1996).
To provide evidence-based direction to this campaign, the Expert Panel on Driver Fatigue and Sleepiness reviewed the research conducted to date on drowsy-driving crashes. The resulting report outlines the following:
 | The biology of human sleep and sleepiness, which physiologically underlies crash risk.
 | Common characteristics of crashes related to drowsy driving and sleepiness.
 | Risks for crashes attributed to drowsy driving.
 | Population groups at highest risk.
 | Effective countermeasures used to prevent drowsy driving and related crashes.
| | | | |
In addition to summarizing what is known—and what remains unknown—from sleep and high-way safety research, the report also presents the panel's recommendations for the highest priority target audiences and educational message points for the NCSDR/NHTSA campaign.

Methods and Knowledge Base of This Report
The panel conducted a wide-ranging search for information on sleep, circadian rhythms, sleepiness, drowsiness, sleep physiology, and sleep disorders, as well as on the association of these topics with driving risk and crash prevention. The panel conducted literature searches of online databases in traffic safety, medicine, and physiology using the keywords listed above and following uggestions for linkage to related topics (e.g., technology, alerting devices, industrial accidents, and shift work). In addition, the panel requested or was forwarded formal and informal reviews and monographs by Federal, State, and nongovernmental agencies. Although there was no formal ranking of the scientific rigor of all this material, original papers, reviews, monographs, and reports selected for citation reflect the higher levels of evidence available on the topic and literature upon which the major concepts or opinions of the panel report are based. The references provided do not, however, reflect all resources available or reviewed by the panel; when possible, more recent material or reviews are preferentially cited.
The principal types of primary data the panel used fall into the following categories:
 | Studies of crash data that identify the characteristics of crashes in which the driver was reported by police to have fallen asleep and the characteristics of the sleepy driver.
 | Self-reports from drivers involved in crashes (with data collected either at the crash scene or retrospectively) that gather information on driver behavior preceding the crash or relevant work, sleep, and other lifestyle habits.
 | Population surveys that relate driver factors to fall-asleep or drowsy-driving crashes or to risky behavior associated with crashes.
 | Laboratory studies using a driver simulator or other fundamental tests that relate the effect on performance of sleepiness, sleep loss, and the combined effects of sleep loss and alcohol consumption.
 | Laboratory studies using a driver simulator or performance tests that examine the performance of persons with sleep disorders compared with a control group.
 | Retrospective studies that compare crash histories of drivers with sleep disorders with other drivers.
 | Laboratory and epidemiological studies of drowsy-driving countermeasures.
| | | | | | |
The literature reviewed had variations in design, method, rigor, populations included, ethodological detail, outcome measures, and other variables, all of which precluded a strict comparison. In addition, the number of studies is relatively small, and some of the studies do not represent large numbers of crashes or feature crash numbers or frequency as an outcome measure.

Research Needs
The panel identified three major categories in which more evidence is needed:
Quantification of the problem.
To allow accurate estimates of the true prevalence of drowsy-driving crashes, it will be important to develop a standard manner by which law enforcement officers can assess and report crashes resulting from drowsy driving. Currently, States use different definitions and have varying reporting requirements, which hinder quantification. However, this is not just a reporting problem; a method for objectively assessing sleepiness at the crash site also would enable better quantification.
Risks.
More information is needed on chronic and acute risks for drowsy-driving crashes. For example, capturing information on drivers' precrash behaviors (e.g., duration of prior wake-fulness, recent sleep-wake patterns, the quality and quantity of sleep, work hours, and work patterns [day shift, night shift, rotating shift]) could enhance understanding of the problems. It is important to learn more about at-risk drivers who do not crash and about the impact of drowsiness on driving at all points on the continuum, from low-level drowsiness to falling asleep at the wheel.
Countermeasures.
Additional information and research are needed on measures that in-crease or restore driver alertness or reduce crash risk or incidence. In addition, studies should determine whether early recognition, treatment, and management of sleepiness and sleep disorders reduce crash risk or incidence. Educational approaches that are effective for reaching high-risk audiences will need to be developed and tested; ultimately, the impact of such approaches on drowsy-driving knowledge, attitudes, and behaviors will need to be examined.

 Biology of Human Sleep and Sleepiness
Biology of Human Sleep and Sleepiness
Sleepiness, also referred to as drowsiness, is defined in this report as the need to fall asleep, a process that is the result of both the circadian rhythm and the need to sleep (see below). Sleep can be irresistible; recognition is emerging that neurobiologically based sleepiness contributes to human error in a variety of settings, and driving is no exception (Åkerstedt, 1995a, 1995b; Dinges, 1995; Horne, 1988; Sharpley, 1996; Martikainen, 1992). In the more recent surveys and reporting of noncommercial crashes, investigators have begun to collect and analyze data for instances in which the driver may have fallen asleep.
The terms "fatigue" and "inattention" are sometimes used interchangeably with sleepiness; however, these terms have individual meanings (Brown, 1994). Strictly speaking, fatigue is the consequence of physical labor or a prolonged experience and is defined as a disinclination to continue the task at hand. In regard to driving, a psychologically based conflict occurs between the disinclination to drive and the need to drive. One result can be a progressive withdrawal of attention to the tasks required for safe driving. Inattention can result from fatigue, but the crash literature also identifies preoccupation, distractions inside the vehicle, and other behaviors as inattention (Treat et al., 1979).
The driving literature before 1985 made little mention of sleepiness and instead focused on the prevention of inattention and fatigue; traffic crash forms did not have a category for reporting sleepiness as a crash cause. Certainly, sleepiness can contribute to fatigue and inattention, and given the lack of objective tests or uniform reporting requirements to distinguish these different crash causes, misclassification and inconsistencies in the primary data and the literature can be expected. Some, but not all, recent studies and reviews make an explicit assumption that given the uncertainty in crash reports, all crashes in the fatigue and inattention categories should be attributed to sleepiness. The panel suspects that sleepiness-related crashes are still very often reported in the categories of fatigue and inattention, and it reached consensus that sleepiness is an underrecognized feature of noncommercial automobile crashes.
The panel concluded that the data on fatigue and inattention provide less support for defining risk factors and high-risk groups than the data on sleepiness or drowsiness. In addition, sleepiness is identifiable, predictable, and preventable.

The Sleep-Wake Cycle
A body of literature exists on the mechanisms of human sleep and sleepiness that affect driving risks. The sleep-wake cycle is governed by both homeostatic and circadian factors. Homeostasis relates to the neurobiological need to sleep; the longer the period of wakefulness, the more pressure builds for sleep and the more difficult it is to resist (Dinges, 1995). The circadian pace-maker is an internal body clock that completes a cycle approximately every 24 hours. Homeostatic factors govern circadian factors to regulate the timing of sleepiness and wakefulness. These processes create a predictable pattern of two sleepiness peaks, which commonly occur about 12 hours after the midsleep period (during the afternoon for most people who sleep at night) and before the next consolidated sleep period (most commonly at night, before bedtime) (Richardson et al., 1982; see Figure 1). Sleep and wakefulness also are influenced by the light/dark cycle, which in humans most often means wake-fulness during daylight and sleep during darkness.
People whose sleep is out of phase with this cycle, such as night workers, air crews, and travelers who cross several time zones, can experience sleep loss and sleep disruption that reduce alertness (Åkerstedt, 1995b; Samel et al., 1995).
The panel noted that the sleep-wake cycle is intrinsic and inevitable, not a pattern to which people voluntarily adhere or can decide to ignore. Despite the tendency of society today to give sleep less priority than other activities, sleepiness and performance impairment are neurobiological responses of the human brain to sleep deprivation. Training, occupation, education, motivation, skill level, and intelligence exert no influence on reducing the need for sleep. Micro-sleeps, or involuntary intrusions of sleep or near sleep, can overcome the best intentions to remain awake.
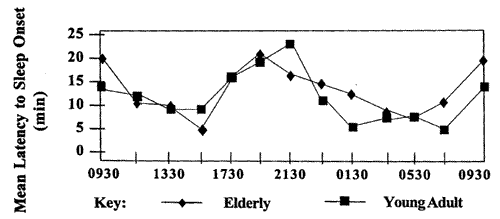
Figure 1. Latency to sleep at 2-hour intervals across the 24-hour day. Testing during the daytime followed standard Multiple Sleep Latency Test procedures. During the night, from 2330 to 0800 hours (based on a 24-hour clock), subjects were awakened every 2 hours for 15 minutes, and latency of return to sleep was measured. Elderly subjects (n = 10) were 60 to 83 years of age; young subjects (n = 8) were 19 to 23 years of age (Carskadon and Dement, 1987).

Sleepiness Impairs Performance
Sleepiness leads to crashes because it impairs elements of human performance that are critical to safe driving (Dinges, Kribbs, 1991). Relevant impairments identified in laboratory and in-vehicle studies include:
 | Slower reaction time. Sleepiness reduces optimum reaction times, and moderately sleepy people can have a performance-impairing increase in reaction time that will hinder stopping in time to avoid a collision (Dinges, 1995). Even small decrements in reaction time can have a profound effect on crash risk, particularly at high speeds.
 | Reduced vigilance. Performance on attention-based tasks declines with sleepiness, including increased periods of nonresponding or delayed responding (Haraldsson et al., 1990; Kribbs, Dinges, 1994) (see Figure 2).
 | Deficits in information processing. Processing and integrating information takes longer, the accuracy of short-term memory decreases, and performance declines (Dinges, 1995).
| | |
Often, people use physical activity and dietary stimulants to cope with sleep loss, masking their level of sleepiness. However, when they sit still, perform repetitive tasks (such as driving long distances), get bored, or let down their coping defenses, sleep comes quickly (Mitler et al., 1988; National Transportation Safety Board, 1995).
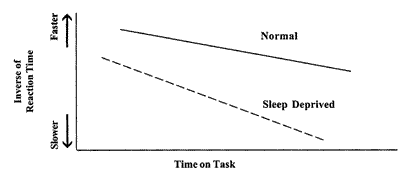
Figure 2. Performance slows with sleep deprivation. A summary of data (Kribbs, Dinges, 1994) on reaction to anevent marker presented to a subject every 4 seconds or so over a 10-minute period. As reaction time is longer, the inverse value is reduced, indicating a slowing of the perception/reaction response. The response to an event marker slows more across time in the leep-deprived (very sleepy) subject than in a subject who has had normal amounts of sleep.

The Causes of Sleepiness/Drowsy Driving
Although alcohol and some medications can independently induce sleepiness, the primary causes of sleepiness and drowsy driving in people without sleep disorders are sleep restriction and sleep fragmentation.
Sleep restriction or loss. Short duration of sleep appears to have the greatest negative effects on alertness (Rosenthal et al., 1993a; Gillberg, 1995). Although the need for sleep varies among individuals, sleeping 8 hours per 24-hour period is common, and 7 to 9 hours is needed to optimize performance (Carskadon, Roth, 1991).
Experimental evidence shows that sleeping less than 4 consolidated hours per night impairs performance on vigilance tasks (Naitoh, 1992). Acute sleep loss, even the loss of one night of sleep, results in extreme sleepiness (Carskadon, 1993b). The effects of sleep loss are cumulative (Carskadon, Dement, 1981). Regularly losing 1 to 2 hours of sleep a night can create a "sleep debt" and lead to chronic sleepiness over time. Only sleep can reduce sleep debt. In a recent study, people whose sleep was restricted to 4 to 5 hours per night for 1 week needed two full nights of sleep to recover vigilance, performance, and normal mood (Dinges et al., 1997).
Both external and internal factors can lead to a restriction in the time available for sleep. External factors, some beyond the individual's control, include work hours, job and family responsibilities, and school bus or school opening times. Internal or personal factors sometimes are involuntary, such as a medication effect that interrupts sleep. Often, however, reasons for sleep restriction represent a lifestyle choice—sleeping less to have more time to work, study, socialize, or engage in other activities.
Job-related sleep restriction.
Contemporary society functions 24 hours a day. Economic pressures and the global economy place increased demands on many people to work instead of sleep, and work hours and demands are a major cause of sleep loss. For example, respondents to the New York State survey who reported drowsy-driving incidents cited a variety of reasons related to work patterns. These included working more than one job, working extended shifts (day plus evening plus night), and working many hours a week (McCartt et al., 1996).
Personal demands and lifestyle choices.
Many Americans do not get the sleep they need because their schedules do not allow adequate time for it. Juggling work and family responsibilities, combining work and education, and making time for enjoyable pastimes often leave little time left over for sleeping. Many Americans are unaware of the negative effects this choice can have on health and functioning (Mitler et al., 1988).
From high-profile politicians and celebrities to the general population, people often see sleep as a luxury. One in four respondents who reported sleeping difficulties in a recent Gallup Survey said you cannot be successful in a career and get enough sleep (National Sleep Foundation, 1995).
Sleep fragmentation.
Sleep is an active process, and adequate time in bed does not mean that adequate sleep has been obtained. Sleep disruption and fragmentation cause inadequate sleep and can negatively affect functioning (Dinges, 1995). Similar to sleep restriction, sleep fragmentation can have internal and external causes. The primary internal cause is illness, including untreated sleep disorders. Externally, disturbances such as noise, children, activity and lights, a restless spouse, or job-related duties (e.g., workers who are on call) can interrupt and reduce the quality and quantity of sleep.
Studies of commercial vehicle drivers present similar findings. For example, the National Transportation Safety Board (1995) concluded that the critical factors in predicting crashes related to sleepiness (which this report called "fatigue") were duration of the most recent sleep period, the amount of sleep in the previous 24 hours, and fragmented sleep patterns.
Circadian factors.
As noted earlier, the circadian pacemaker regularly produces feelings of sleepiness during the afternoon and evening, even among people who are not sleep deprived (Dinges, 1995). Shift work also can disturb sleep by interfering with circadian sleep patterns.

Evaluating Sleepiness
An ideal measure of sleepiness would be a physiologically based screening tool that is rapid and suitable for repeated administration (Mitler, Miller, 1996). No measures currently exist for measuring sleepiness in the immediacy of crash situations. Furthermore, a crash is likely to be an altering circumstance. A measuring system would be performance based and in vehicle, linked to alerting devices designed to prevent the driver from falling asleep.
The current tools for the assessment of sleepiness are based on questionnaires and electrophysiological measures of sleep, and there is interest in vehicle-based monitors. A comprehensive review of these efforts is beyond the scope of the present report. In the following brief discussion, some tools for the assessment of sleepiness are described to illustrate the different subjective and objective measures of chronic and situational (acute) sleepiness and the vehicle-based technology to sense sleepiness.
Assessment for chronic sleepiness.
The Epworth Sleepiness Scale (ESS) (Johns, 1991) is an eight-item, self-report measure that quantifies individuals' sleepiness by their tendency to fall asleep "in your usual way of life in recent times" in situations like sitting and reading, watching TV, and sitting in a car that is stopped for traffic. People scoring 10 to 14 are rated as moderately sleepy, whereas a rating of 15 or greater indicates severe sleepiness. The ESS is not designed to be used to assess situational sleepiness or to measure sleepiness in response to an acute sleep loss. The ESS has been used in research on driver sleepiness and in correlations of sleepiness to driving performance in people with medical disorders.
Other rating tools that measure an individual's experience with sleepiness over an extended period of time and contain a component or scale that is congruent with measuring sleepiness include the Pittsburgh Sleep Quality Index (Buysse et al., 1989) and the Sleep-Wake Activity Inventory (Rosenthal et al., 1993b). Other self-report instruments obtain historical information pertinent to sleepiness using patient logs and sleep-wake diaries (Douglas et al., 1990) and the Sleep Disorders Questionnaire (Douglas et al., 1994). The information gathered with these instruments has not been as widely applied to assessments of noncommercial crashes.
Laboratory tools for measuring sleepiness include the Multiple Sleep Latency Test (MSLT) (Carskadon et al., 1986; Carskadon, Dement, 1987) and the Maintenance of Wakefulness Test (MWT) (Mitler et al., 1982). The MSLT measures the tendency to fall asleep in a standardized sleep-promoting situation during four or five 20-minute nap opportunities that are spaced 2 hours apart throughout the day and in which the individual is instructed to try to fall asleep. Sleep is determined by predefined brain wave sleep-staging criteria. The presumption underlying this test is that people who fall asleep faster are sleepier. Individuals who fall asleep in 5 minutes or less are considered pathologically sleepy; taking 10 minutes or more to fall asleep is considered normal. In the MWT, individuals are instructed to remain awake, and the time it takes (if ever) in 20 minutes to fall asleep by brain wave criteria is the measure of sleepiness..
Although the relative risk for fall-asleep crashes has not been established, individuals who exhibit a sleep latency of less than 15 minutes on the MWT are categorically too sleepy to drive a motor vehicle (Mitler, Miller, 1996).
The MSLT and MWT were developed for neuro-physiologic assessment and are sensitive to acute as well as chronic sleep loss. Both assume standardization of procedures involving specially trained personnel and are not valid if the individual being tested is ill or in pain (Carskadon, 1993b). The panel thought that the use of these medical tests may not be practical for crash assessment; however, the use of a modified "nap test" has been used along with questionnaires for field assessment of driver sleepiness (Philip et al., 1997).
Assessment for acute sleepiness.
Acute sleepiness is defined as a need for sleep that is present at a particular point in time. The Stanford Sleepiness Scale (SSS) (Hoddes et al., 1973) is an instrument that contains seven statements through which people rate their current level of alertness (e.g., 1= "feeling...wide awake" to 7= "...sleep onset soon..."). The scale correlates with standard performance measures, is sensitive to sleep loss, and can be administered repeatedly throughout a 24-hour period. In some situations, the scale does not appear to correlate well with behavioral indicators of sleepiness; in other words, people with obvious signs of sleepiness have chosen ratings 1 or 2.
The Karolinska Sleep Diary (Åkerstedt et al., 1994) contains questions relating to self-reports of the quality of sleep. Laboratory and some field studies suggest that most subjective sleep measures in this scale show strong covariation and relation to sleep continuity across a wide spectrum of prior sleep length and fragmentation. As in the SSS, several questions are asked to determine values for subjective sleepiness.
A Visual Analogue Scale (VAS) for sleepiness permits the subjects to rate their "sleepiness" in a continuum along a 100-mm line (Wewers, Low, 1990). Anchors for sleepiness range from "just about asleep" (left end) to "as wide awake as I can be" (right end). Persons rate their current feelings by placing a mark on the line that indicates how sleepy they are feeling. The VAS is scored by measuring the distance in millimeters from one end of the scale to the mark placed on the line. The VAS is convenient and rapidly administered over repeated measurements.
In all these attempts to measure subjective sleepiness, a person's response is dependent on both the presentation of the instructions and the subject's interpretation of those instructions. Problems related to these factors may confound interpretation between studies and between groups of different ages or cultures.
Vehicle-based tools.
There are some in-vehicle systems that are intended to measure sleepiness or some behavior associated with sleepiness in commercial and noncommercial driving. Examples include brain wave monitors, eye-closure monitors, devices that detect steering variance, and tracking devices that detect lane drift (Dinges, 1995). This technology is currently being examined in physiologic, psychophysiologic, and crash-prevention domains. There is insufficient evidence at present to judge its application and efficacy in regard to noncommercial driving.

 Characteristics of Drowsy-Driving Crashes
Characteristics of Drowsy-Driving Crashes
As noted above, unlike the situation with alcohol-related crashes, no blood, breath, or other objective test for sleepiness currently exists that is administered to a driver at the scene of a crash. No definitive criteria are available for establishing how sleepy a driver is or a threshold at which driver sleepiness affects safety. If drivers are unharmed in a crash, hyperarousal following the crash usually eliminates any residual impairment that could assist investigating officers in attributing a crash to sleepiness.
As a result, our understanding of drowsy-driving crashes is based on subjective evidence, such as police crash reports and driver self-reports following the event, and may rely on surrogate measures of sleepiness, such as duration of sleep in a recent timeframe or sleep/work patterns. Some researchers have addressed the problem by analyzing only those crashes known not to be caused by alcohol (because alcohol can cause sleepiness and affect other performance variables), mechanical problems, or other factors and by looking for evidence of a sleepiness effect in categories of inattention or fatigue. Thus, reports on drowsy driving are often inferential. The strength of the inferences is increased when different types of studies reach similar conclusions.
The characteristics of drowsy-driving crashes reported below resemble the inclusion criteria that some researchers have used to define a crash as having been caused by drowsiness. This similarity suggests the possibility that the researchers' initial assumptions influenced the determination of crash characteristics. Despite these caveats, a fairly clear picture emerges from studies conducted to date of the typical crash related to sleepiness.
The problem occurs during late-night hours.
Drowsy-driving crashes occur predominantly after midnight, with a smaller secondary peak in the midafternoon (Studies of police crash reports: Pack et al., 1995; Knipling, Wang, 1994; New York State GTSC Sleep Task Force, 1994; New York State Task Force on Drowsy Driving, 1996; Langlois et al., 1985; Lavie et al., 1986; Mitler et al., 1988; Horne, Reyner 1995b; Studies based on driver self-reports: Maycock, 1996; McCartt et al., 1996). Studies of commercial drivers show a similar pattern (see Figure 3). According to a 1996 report, time of day was the most consistent factor influencing driver fatigue and alertness. Driver drowsiness was markedly greater during night driving than during daytime driving, with drowsiness peaking from late evening until dawn (Wylie et al., 1996). Nighttime and midafternoon peaks are consistent with human circadian sleepiness patterns.
The risk of a crash related to sleepiness increases during nighttime hours among both younger drivers (25 years of age and younger) and drivers between the ages of 26 and 45. However, younger drivers have no increased risk during the afternoon, when the
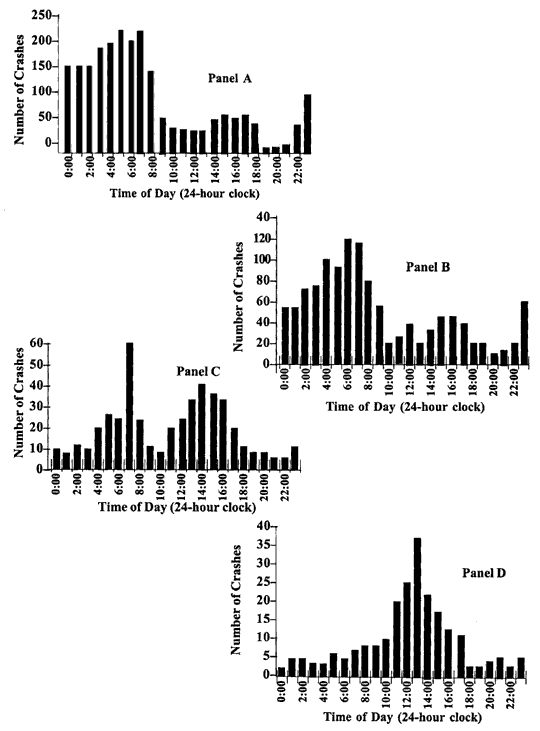
predictable circadian sleepiness peak is expected. Drivers ages 45 through 65 have fewer nighttime crashes, with a peak at 7 a.m. Drivers ages older than 65 are more likely to have fall-asleep crashes during the midafternoon (Pack et al., 1995; Wang, Knipling, Goodman, 1996).
Fall-asleep crashes are likely to be serious.
The morbidity and mortality associated with drowsy-driving crashes are high, perhaps because of the higher speeds involved (Horne, Reyner, 1995b) combined with delayed reaction time. In North Carolina, more of these crashes resulted in injury compared with other, nonalcohol-related crashes—fatalities occurred in 1.4 percent and 0.5 percent, respectively (Pack et al., 1995). Pack (1995) and Maycock (1996) both conclude that a higher proportion of the most serious crashes are sleepiness related.
A single vehicle leaves the roadway.
An analysis of police crash reports in North Carolina showed the majority of the nonalcohol, drowsy-driving crashes were single-vehicle roadway departures (Pack et al., 1995). Among New York State drivers surveyed about their lifetime experience with drowsy driving, almost one-half of those who had a fall-asleep or drowsy-driving crash reported a single-vehicle roadway departure; about one-fourth of those who had fallen asleep without crashing also reported going off the road (McCartt et al., 1996). NHTSA General Estimates System data reflect the same trend but also suggest that sleepiness may play a role in rear-end crashes and head-on crashes (Knipling, Wang, 1994).
The crash occurs on a high-speed road.
In comparison with other types of crashes, drowsy-driving crashes more often take place on highways and major roadways with speed limits of 55 to 65 mph (Knipling, Wang, 1994; Wang, Knipling, Goodman, 1996). Pack and colleagues (1995) found that most sleepiness-related crashes occur at higher speeds, attributing this finding to the effect of sleep loss on reaction time. NHTSA figures show that most drowsiness- or fatigue-related crashes occur on higher speed roads in nonurban areas. However, Maycock (1996) found that a greater absolute number occur in built-up areas. Panel members noted the possibility that more crashes occur on high-speed roads because more long-distance nighttime driving occurs on highways.
The driver does not attempt to avoid crashing.
NHTSA data show that sleepy drivers are less likely than alert drivers to take corrective action before a crash (Wang, Knipling, Goodman, 1996). Anecdotal reports also suggest that evidence of a corrective maneuver, such as skid marks or brake lights, is usually absent in fall-asleep crashes.
The driver is alone in the vehicle.
In the New York State survey of lifetime incidents, 82 percent of drowsy-driving crashes involved a single occupant (McCartt et al., 1996). Conversely, respondents who reported having fallen asleep without crashing were less likely to have been alone in the automobile.
Wilkins and colleagues (1997) confirmed that crashes attributed to driver fatigue have characteristics similar to those cited above regarding driver age, time of day, crash type, and severity. But, in addition, when alcohol involvement was combined with fatigue or sleepiness, the patterns became more pronounced. For example, "asleep with alcohol" crashes involved a higher percentage of young males than did crashes in which the driver was asleep with no evidence of alcohol.

 Risk for Drowsy-Driving Crashes
Risk for Drowsy-Driving Crashes
Although its conclusions were based on a limited body of knowledge, the panel identified a number of chronic predisposing factors and acute situational factors that increase the risk of drowsy driving and drowsy-driving crashes. These include sleep loss, driving patterns that disregard the normal sleep-wake cycle or represent driving increased time or miles (exposure), the use of sedating medication, sleep disorders such as sleep apnea syndrome (SAS) and narcolepsy, and the increased drowsiness and performance impairment that result from consuming alcohol when drowsy. All factors may interact, and with the exception of medical disorders, all factors may have either chronic or acute effects.

Sleep Loss
As noted before, external and internal factors and current lack of knowledge and attitudes about sleep cause many Americans to get inadequate sleep either occasionally (acute sleepiness) or routinely (chronic sleepiness). Those who suffer chronic sleep restriction and sleepiness may also combine this lifestyle pattern with situational acute sleep loss, aggravating their risk of drowsy driving.
Chronic sleepiness.
In a recent Gallup survey, approximately one-half of U.S. adults reported experiencing sleeping difficulties sometimes, with about 1 in 10 saying the difficulties are frequent (National Sleep Foundation, 1995). In a 1997 followup survey, three of four Americans who reported getting as much or more sleep than they "need" said they were sleepy during the day. One in three of the adult public was deemed "significantly" sleepy on the Epworth Sleepiness Scale (ESS), and 1 in 20 scored at the "severe" sleepiness level (National Sleep Foundation Survey, 1997).
In the New York State survey, the reported frequency of drowsy driving in the past year was associated with the quantity and quality of sleep obtained. For example, those who reported having fair or poor sleep quality were more likely to have driven drowsy sometimes or very often than were those who said their sleep was good or excellent (McCartt et al., 1996).
In addition, Maycock (1996) found that higher scores on the ESS were positively associated with crashes. Drivers who reported having trouble staying awake during the day were more likely to report having sometimes or very often driven drowsy (McCartt et al., 1996).
Acute sleep loss.
As discussed in an earlier chapter, the loss of even one night of sleep may cause extreme sleepiness. Short-term work demands, child care, socializing, preparing for a trip or vacation, and "pulling all nighters" are common causes of acute sleep loss.
Sleep-restrictive work patterns.
Working the night shift, overtime, or rotating shifts is a risk for drowsy driving that may be both chronic and acute. In the New York State survey, nearly one-half the drowsy drivers who crashed (and more than one-third of those who drove drowsy without crashing) reported having worked the night shift or overtime prior to the incident. In addition, a higher reported frequency of driving drowsy was associated with working a rotating shift, working a greater number of hours per week, and more frequently driving for one's job (McCartt et al., 1996). In the British study (Maycock, 1996), respondents said that working the night shift led to sleepiness while driving, and in many studies a majority of shift workers admit having slept involuntarily on the night shift. The return to day work and morning shifts starting between 4 a.m. and 7 a.m. also may lead to sleepiness. EEG studies of sleep in rotating shift workers in both the natural environment and the laboratory have shown that day sleep after night work and early night sleep before morning work (e.g., going to sleep at 7 or 8 p.m. before a 4 a.m. shift) is 2 to 4 hours shorter than night sleep (Åkerstedt, 1995a).
In addition, a study of hospital house staff working around the clock (Marcus, Loughlin, 1996) found higher levels of sleepiness and crashes following on-call periods. In a survey of hospital nurses, night nurses and rotators were more likely than nurses on other shifts to report nodding off at work and at the wheel and having had a driving mishap on the way home from work (Gold et al., 1992).

Driving Patterns
Driving patterns, including both time of day and amount of time driven, can increase crash risk. As detailed earlier, the greatest proportion of drowsy-driving crashes occurs during the late-night hours. The biology of the sleep-wake cycle predicts sleepiness during this time period, which is a circadian sleepiness peak and a usual time of darkness. Other driving time patterns that increase risk include driving a larger number of miles each year and a greater number of hours each day (McCartt et al., 1996) and driving a longer time without taking a break or, more often, driving for 3 hours or longer (Maycock, 1996).

The Use of Sedating Medications
A number of studies indicate that using certain medications increases the risk of sleepiness-related crashes, particularly using prescribed benzodiazepine anxiolytics, long-acting hypnotics, sedating antihistamines (H1 class), and tricyclic antidepressants (Kozena et al., 1995; Van Laar et al., 1995; Ray et al., 1992; Leveille et al., 1994; Ceutel, 1995; Gengo, Manning, 1990). The risks are higher with higher drug doses and for people taking more than one sedating drug simultaneously (Ray et al., 1992). Younger males have higher risks than do females or other age groups across all drug classes. It appears that risk is highest soon after the drug regimen is initiated and falls to near normal after several months (Ceutel, 1995). Recreational drug use also may exacerbate sleepiness effects (Kerr et al., 1991).

Untreated Sleep Disorders: Sleep Apnea Syndrome and Narcolepsy
Untreated sleep apnea syndrome and narcolepsy increase the risk of automobile crashes (Findley et al., 1995; George et al., 1987; Aldrich, 1989; Alpert et al., 1992; Broughton et al., 1981; Broughton et al., 1984). No current data link other sleep disorders with drowsy-driving crashes. However, other medical disorders causing disturbed sleep and excessive daytime sleepiness could pose risks.
In sleep apnea syndrome, brief interruptions of air flow and loss of oxygen during sleep disrupt and fragment sleep. The condition also is associated with loud, chronic snoring. Although people with untreated sleep apnea syndrome may not be aware of the brief disturbances, poor sleep quality often leads to daytime sleepiness. Narcolepsy is a disorder of the sleep-wake mechanism that also causes excessive daytime sleepiness. In untreated patients, involuntary 10- to 20-minute naps are common at 2- to 3-hour intervals throughout the day. Cataplexy, a sudden loss of muscle tone ranging from slight weakness to complete collapse, is another major symptom of narcolepsy that increases the risk of crash. These conditions are unrecognized and untreated in a substantial number of people (National Sleep Foundation Survey, 1997; American Thoracic Society, 1994).

Consumption of Alcohol Interacts With Sleepiness to Increase Drowsiness and Impairment
Although sleepiness and alcohol are distinct crash causes, the data also show some evidence of overlap. NHTSA found that drivers had consumed some alcohol in nearly 20 percent of all sleepiness-related, single-vehicle crashes (Wang, Knipling, Goodman, 1996). More than one in three New York State drivers surveyed in drowsy-driving crashes said they had drunk some alcohol (McCartt et al., 1996), and police- reported, fall-asleep crashes had a higher proportion of alcohol involvement than other types of crashes in that State. (New York GTSC Task Force, 1994; New York State Task Force, 1996).
Laboratory studies explain and predict these patterns. Many researchers have shown that sleepiness and alcohol interact, with sleep restriction exacerbating the sedating effects of alcohol, and the combination adversely affecting psychomotor skills to an extent greater than that of sleepiness or alcohol alone (Roehrs et al. 1994; Wilkinson, 1968; Huntley, Centybear, 1974; Peeke et al., 1980). Driving simulation tests specifically show this effect, even with modest reductions in sleep, low alcohol doses, and low blood ethanol concentrations. In a driving simulation study, alcohol levels below the legal driving limit produced a greater number of deviations from the road after 4 hours of sleep than after 8 hours of sleep (Roehrs et al., 1994) (see figure 4).
It is possible that the effects of low levels of blood alcohol may have an interaction with circadian rhythms that produces sleepiness in the afternoon and evening (Roehrs et al., 1994; Horne, Baumber, 1991; Horne, Gibbons, 1991). The panel speculated that drinking alcohol before driving in the afternoon or at night might pose special risks given the circadian effects.

Interactions Among Factors Increase Overall Risk
Some of the crash-related factors have been studied more than others. The panel could not find evidence to determine whether chronic or acute situations pose the greater risk for crashes. However, it is clear that these factors are cumulative, and any combination of chronic and acute factors substantially increases crash risk. For example, people with chronic sleep loss who drive in the early morning hours are likely to be at greater risk than are early morning drivers who slept well the night before and usually get enough sleep.
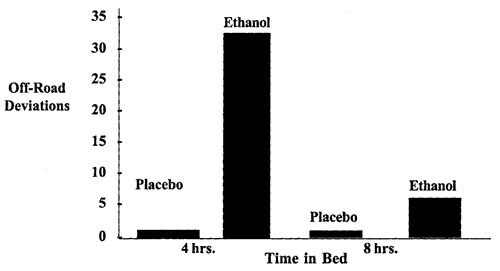
Figure 4. Interaction between alcohol and sleepiness. These data from Roehrs et al. (1994) were collected in a laboratory using a driving simulator. Studies were performed in the morning after either 8 hours or 4 hours of time in bed the previous night and with either a low dose of ethanol or placebo. The number of off-road deviations by the driver was 4 times higher after 8 hours of sleep time but 15 times higher with only 4 hours of sleep time.

 Population Groups at Highest Risk
Population Groups at Highest Risk
All drivers who experience the chronic or acute situations described earlier are at risk for drowsy driving and drowsy-driving crashes. Although no one is immune from risk, research to date clearly identifies three broad population groups at high risk for drowsy-driving crashes. Their higher risk is based on (1) evidence from crash data of a greater absolute or relative number of fall-asleep crashes and/or (2) increased intermediate risk, based on subjective reports of their having higher levels of sleepiness and more of the chronic or acute factors that underlie risk for everyone. The three groups at high risk are young people, shift workers, and people with untreated sleep conditions.

Young People, Especially Young Men
Virtually all studies that analyzed data by gender and age group found that young people, and males in particular, were the most likely to be involved in fall-asleep crashes (Pack et al., 1995; Horne, Reyner, 1995b; Maycock, 1996; Knipling, Wang, 1994). Definitions of "young" differed among authors; the ages included in this category fell between 16 and 29.
Young people.
Knipling and Wang (1995) found that drivers younger than 30 accounted for almost two-thirds of drowsy-driving crashes, despite representing only about one-fourth of licensed drivers. These drivers were four times more likely to have such a crash than were drivers ages 30 years or older. In Pack and colleagues' study (1995), 20 was the peak age of occurrence of drowsy-driving crashes, whereas in New York State the greatest number of drowsy drivers (on self-report) were within the 25-to-34 age group (McCartt et al., 1996), and both the 18-to-24 and 25-to-39 age groups were overrepresented in fall-asleep crashes (New York State Task Force, 1996).
Horne and Reyner (1995a) suggest that a combination of having more of the chronic and acute risk factors and frequently being on the roads during nighttime hours (greater exposure) may explain the greater incidence of drowsiness-related crashes in youth. Carskadon (1990) offers a variety of age-specific reasons for the involvement of younger people, particularly adolescents. During this period, young people are learning to drive, experimenting and taking risks, and testing limits. At the same time, this age group is at risk for excessive sleepiness because of the following:
 | Maturational changes that increase the need for sleep.
 | Changes in sleep patterns that reduce nighttime sleep or lead to circadian disruptions.
 | Cultural and lifestyle factors leading to insufficient sleep, especially a combination of schoolwork demands and part-time jobs, extracurricular activities, and late-night socializing. In one study (Carskadon, 1990), boys with the greatest extracurricular time commitments were most likely to report falling asleep at the wheel. The subgroup at greatest risk comprised the brightest, most energetic, hardest working teens.
| | |
The panel felt that vulnerability may be further increased when young people use alcohol or other drugs because sleepy youth are likely to be unaware of the interaction of sleepiness and alcohol and may not recognize related impairments they experience.
Males.
In North Carolina, males were found to be at the wheel in about three of four fall-asleep crashes (Pack et al., 1995). NHTSA data show.that males are 5 times more likely than females to be involved in drowsy-driving crashes (Wang, Knipling, Goodman, 1996). The reasons young males have more crashes than do young females are not clear because both young men and young women are likely to be chronically sleep-deprived.

Shift Workers
Most shift workers have at least occasional sleep disturbances, and approximately one-third complain of fatigue (Åkerstedt, 1995a, 1995b, 1995c). Older shift workers appear to have more sleep-related difficulties than do younger workers, but no gender differences have been found (Harma, 1993). Night shift workers typically get 1.5 fewer hours of sleep per 24 hours as compared with day workers. The midnight to 8 a.m. shift carries the greatest risk of sleep disruption because it requires workers to contradict circadian patterns in order to sleep during the day (Kessler, 1992).
Investigations have demonstrated that circadian phase disruptions caused by rotating shift work are associated with lapses of attention, increased reaction time, and decreased performance (Dinges et al., 1987; Hamilton et al., 1972; Williams et al., 1959). A study of hospital nurses reached similar conclusions based on "real world" experiences. Rotating shifts (working four or more day or evening shifts and four night shifts or more within a month) caused the most severe sleep disruptions of any work schedule. Nurses on rotating schedules reported more "accidents" (including auto crashes, on-the-job errors, and on-the-job personal injuries due to sleepiness) and more near-miss crashes than did nurses on other schedules (Gold et al., 1992). About 95 percent of night nurses working 12-hour shifts reported having had an automobile accident or near-miss accident while driving home from night work (Novak, Auvil-Novak, 1996).
Hospital interns and residents routinely lose sleep during on-call periods, which may last 24 hours or more. A survey of house staff at a large urban medical school found that respondents averaged 3 hours of sleep during 33-hour on-call shifts, much of which was fragmented by frequent interruptions (Marcus, Loughlin, 1996). About 25 percent reported that they had been involved in a motor vehicle crash, 40 percent of which occurred while driving home from work after an on-call night. Others reported frequently falling asleep at the wheel without crashing, for example, while stopped at a traffic light.
Although this evidence does not demonstrate a conclusive association between shift work and crashes, the panel believes that shift workers' increased risks for sleepiness are likely to translate into an increased risk for automobile crashes. Competing demands from family, second jobs, and ecreation often further restrict the hours available for sleep and further disrupt the sleep schedule. The panel also designated shift workers as a high-risk group because the number of people who perform shift work—and are thus exposed to crash risk—is increasing. This sector is growing at a rate of 3 percent per year, as businesses such as overnight deliveries, round-the-clock computer operations, overnight cleaning crews, 24-hour markets, and continuous-operation factories prosper and expand. Currently about one in five men (20.2 percent) and almost one in six women (15 percent) work other than a daytime shift, including evening, night, rotating, split, and irregular shifts (Kessler, 1992).

People With Untreated Sleep Apnea Syndrome and Narcolepsy
Although the absolute number of crashes is low, crash risk is increased among people with untreated sleep apnea syndrome (SAS) and narcolepsy. The proportion of crashes is higher for people with untreated narcolepsy than it is for people with untreated SAS. However, because SAS is more common than narcolepsy, the absolute number of crashes is higher for those with untreated SAS (Aldrich, 1989). In addition, patients with untreated SAS or narcolepsy perform less well on driving simulation and vigilance or attention tests than do people without these disorders (Findley, 1995; American Thoracic Society, 1994; Haraldsson et al., 1990). Undiagnosed sleep-disordered breathing, ranging from habitual snoring to repeated breathing interruptions, also increases the likelihood of crashes in a dose-response manner (Stradling et al., 1991; Philip et al., 1996; Hanning, Welch, 1996; Ohayon, Priest, Caulet, et al., 1997).
Although these conditions place people at higher risk for drowsy-driving crashes, they are not invariably linked with impaired driving. For example, many people with these disorders report no auto crashes (Findley et al., 1988; Aldrich, 1989). Findley and colleagues (1989) found that patients with severe untreated sleep apnea had more frequent crashes than did those with untreated mild apnea. A patient who can recognize impending uncontrollable sleepiness and take precautions is less likely to be at risk than one who is unaware of or denies his or her sleepiness (Aldrich, 1989).
Sleep apnea syndrome is somewhat more common among males than among females, and typical patients tend to be overweight and middle aged or older, with a large collar size and history of loud snoring; however, women and men without this profile also have the disorder (American Thoracic Society, 1994). People with narcolepsy are as likely to be female as male, and the disorder usually begins in adolescence. The time from onset of symptoms to diagnosis of narcolepsy averages 10 years (American Thoracic Society, 1994; National Commission on Sleep Disorders Research, 1993). Currently, many people with these conditions are undiagnosed and untreated, unaware of the potentially serious consequences of driving while drowsy, or unaware of the seriousness of the difficulty they may experience in maintaining alertness (Arbus et al., 1991; Hansotia, 1997). Falling asleep at the wheel may be a major factor that motivates undiagnosed patients to seek medical care. The matter is rarely raised in driver or law enforcement education, and even health care professionals may not recognize a history of sleepiness as a risk factor for fall-asleep crashes. Medical systems have been successful in identifying only a fraction of the population with symptomatic sleep apnea (Strohl, Redline, 1996).

 Countermeasures
Countermeasures
The panel reviewed the knowledge base in four categories of countermeasures: behavioral, medical, alerting devices, and shift work. They found only a few scientific evaluations of potential countermeasures, most of which were laboratory studies. Reports that exist tend to address the biological feasibility of reducing drowsiness or improving alertness, rather than demonstrate an intervention that reduces drowsy-driving crashes. As noted earlier, more research is needed on this topic.
Countermeasures for drowsy driving aim either to prevent it or to ameliorate it after it occurs. The panel concluded that preventing drowsiness with adequate sleep before driving is both easier and much more successful than any remedial measure reviewed. Methods of obtaining adequate sustained sleep include creating a positive sleep environment (a room that is cool, quiet, and dark) and sleeping at regularly scheduled times. Such measures are often promoted as "sleep hygiene" and make intuitive sense; however, few rigorous studies support all sleep hygiene claims.
The panel noted that the wake-up effects from remedial approaches to existing sleepiness do not last long. At best they can help sleepy drivers stay awake and alert long enough to find a motel, call for a ride, or stop driving and sleep. They are not a substitute for good sleep habits and should not be viewed as a "driving strategy" that can get drowsy drivers safely to their destination.

Behavioral Interventions
In addition to getting adequate sleep before driving, drivers can plan ahead to reduce the risk of drowsy driving in other ways. Some evidence exists that napping before a long drive may help make up for sleep loss in the short term and enhance wakefulness during the drive. Napping has the greatest effect on performance several hours after the nap (Dinges et al., 1987; Dinges,1992, 1995). Two other proven interventions avoid known problem situations: not drinking alcohol when sleepy (Roehrs et al., 1994) and not driving between midnight and 6 a.m. (Mitler et al., 1988; Åkerstedt, 1995c), especially well into the period when sleep is usual (Brown, 1994). Graduated driver-licensing programs that disallow late-night driving among younger drivers can mandate this risk-avoiding behavior (Waller, 1989; Frith, Perkins, 1992).
When a driver becomes drowsy, the most obvious behavioral step for avoiding a crash is to stop driving and sleep for an extended period. When this approach is not practical and another driver is not available to take over, studies have found two remedial actions that can make a short-term difference:
Napping.
Taking a break for a short nap (about 15 to 20 minutes) has been shown to improve subsequent performance, even among sleep-deprived people (Horne, Reyner, 1995a; Dinges et al., 1987; Philip et al., 1997). Naitoh (1992) found that short naps every 6 hours during a 35-hour (otherwise sleepless) period was effective in maintaining performance in the laboratory. However, nappers are often groggy for about 15 minutes upon awakening from naps longer than 20 minutes (Dinges, 1992). Practical issues with this strategy include the inability of some people to take short naps and the need for secure rest areas. The New York State survey found that about one-third of drivers had needed or wanted to stop in the past year, but a rest area was not available. Many also were unlikely to use a rest area when they were driving alone at night.
Consuming caffeine.
Caffeine, even in low doses, significantly improves alertness in sleepy people (but only marginally in those already alert) (Regina et al., 1974; Lumley et al., 1987; Griffiths et al., 1990; Lorist et al., 1994). The minimum dose needed can be obtained in about two cups of percolated coffee, although caffeine content of coffee varies widely (Fox, 1993). Caffeine also is available in other forms such as caffeine-fortified soft drinks and tablets. In driving simulators, sleep-deprived drivers who consumed caffeine reduced lane deviations, potential crashes, and sleepiness for about an hour after consumption (Horne, Reyner, 1995a).
In addition, limited evidence suggests that physical discomfort (such as sitting in an uncomfortable seat or position and shivering or sweating) may also keep sleepy drivers awake (Åkerstedt, Ficca, 1997). Nicotine can improve short-term performance significantly in people with cognitive or attention performance impairments such as those from sleepiness (Kerr et al., 1991). Obviously, however, smoking tobacco should not be generally recommended in an educational campaign as a drowsy-driving countermeasure because the well-established risks substantially outweigh the possible benefits. The panel found no evidence of effectiveness for commonly accepted remedial approaches such as brief exercise (e.g., getting out of the car and walking around for a few minutes) (Horne, 1988), listening to the car radio, or opening the car windows (Horne, Reyner, 1995a). The panel found no studies evaluating other driver-reported steps such as talking to another passenger, talking on a cellular phone or CB radio, chewing gum or ice, or snacking. One study suggests that talking on a cellular phone while driving is associated with increased crash risk (Redelmeier, Tibshirani, 1997).

Medical Interventions to Treat Narcolepsy and Sleep Apnea Syndrome
Although effective treatments are available for both narcolepsy and obstructive sleep apnea, relief of sleepiness and related symptoms is not always easily achievable for all patients (Broughton et al., 1981; Haraldsson et al., 1995). Although treatment can improve driving simulator performance (Findley et al., 1989), individual performance varies. A few studies to date have evaluated crash experiences of patients successfully treated for these disorders and found a positive effect (Cassel et al., 1996; Haraldsson et al., 1995). An impediment to diagnosis is a lack of physician education on the recognition of sleepiness and sleep disorders (National Commission on Sleep Disorders Research, 1993).

Alerting Devices
To date, research has validated only one type of device that alarms or awakens drivers who are drowsy or asleep—shoulder rumble strips placed on high-speed, controlled-access, rural roads. A recent synthesis of reports on the effectiveness of rumble strips shows that they reduce drive-off-the-road crashes by 30 to 50 percent—the only countermeasure the panel found in any category that has a demonstrated effect on crashes. Rumble strips also appear to be a relatively low-cost solution with a positive benefit-to-cost ratio (Garder, Alexander, 1995; National Sleep Foun-dation, June 1997). However, the effectiveness of rumble strips has been demonstrated only in drive-off-the-highway crashes; their value with other types of sleepiness or inattention crashes or other types of roads has not been studied.
Earlier section listed some of the technological in-vehicle monitors designed to detect and evaluate driver sleepiness. Some of these devices contain alarms or other alerting devices that go off when indications of sleepiness occur. Controlled trials are needed to evaluate the usefulness of these tools.
An inherent deficiency in all types of alerting devices is that many people continue to drive even when they know they are drowsy and fighting to stay awake. Although an effective alerting device may prevent one crash, a driver who falls asleep once is likely to fall asleep again unless he or she stops driving. Some safety experts have expressed concern that alerting devices may in fact give drivers a false sense of security, encourage them to drive long after impairment, and inhibit their taking effective behavioral measures to prevent or relieve sleepiness (Lisper et al., 1986; Dinges, 1995; Horne, Reyner, 1995a).

Shift Work Measures
Research has shown that effective steps are available for both employers and employees to reduce the likelihood of excessive sleepiness and drowsy driving. Because of the complexity of the issues involved (Rosekind et al., 1995), a combination of alertness management approaches is likely to be most effective. Researchers also have found differences in individual tolerance to shift work (Harma, 1993); knowing more about the biological and behavioral factors that determine these differences could provide direction for future educational efforts.

Employer Management of Work Schedules
Several approaches have been effective in reducing sleepiness caused by working irregular hours and nighttime hours. To minimize disruption and help employees adjust to circadian rhythm changes, employers should educate employees about the problem (Harma, 1993). In addition, periods of work longer than 8 hours have been shown to impair task performance and increase crashes. For example, performance appears worse with a 12-hour, 4-day week schedule than with an 8-hour, 6-day week (Brown, 1994). In jobs with extended hours, the scheduling of work and rest periods to conform to circadian rhythms promotes better sleep and performance (Stampi, 1994). Another effective approach is to allow and facilitate napping for night shift workers (Dinges, 1992; Naitoh, 1992).

Employee Behavioral Steps
Shift workers themselves can take steps to reduce their risks of drowsy driving by planning time and creating an environment for uninterrupted, restorative sleep (good sleep hygiene) (Minors, Waterhouse, 1981; Rosa, 1990). Shift workers who completed a 4-month physical training program reported sleeping longer and feeling less fatigue than did matched controls who did not participate in the program. However, individual response to the stresses of shift work varies (Harma, 1993), and the background factors or coping strategies that enable some workers to adapt successfully to this situation are not well defined. The behavioral steps discussed earlier for younger males also seem reasonable for reducing risk in this population.
Nurses working the night shift reported using white noise, telephone answering machines, and light-darkening shades to improve the quality and quantity of daytime sleep (Novak, Auvil-Novak, 1996).

Using Bright Light Treatments
Several studies show that timed exposure to bright light has been successful in helping shift workers and those suffering from jet lag adapt to and overcome circadian phase disruption (Czeisler et al., 1990; Stampi, 1994). This approach promotes longer, uninterrupted sleep, which may help reduce sleepiness on the job and behind the wheel. The panel did not find data linking such treatment to changes in rates of crashes or industrial accidents.

 Focusing an Educational Campaign: Panel Recommendations
Focusing an Educational Campaign: Panel Recommendations
To assist the NCSDR/NHTSA in developing its educational initiatives, the panel recommended three priorities for the campaign:
- Educate young males (ages 16 to 24) about drowsy driving and how to reduce lifestyle-related risks.
- Promote shoulder rumble strips as an effective countermeasure for drowsy driving; in this context, raise public awareness about drowsy-driving risks and how to reduce them.
- Educate shift workers about the risks of drowsy-driving and how to reduce them.

Educate Young Males About Drowsy Driving and How to Reduce Lifestyle-Related Risks
Young males, ages 16 to 24, received highest priority because of their clear over-representation in crash statistics and because many of their lifestyle risks are amenable to change. Although males up to age 45 have increased crash risks, the panel targeted only the younger group to enable specific tailoring of educational messages to this population's needs and preferences. In fact, campaign designers may want to segment further, creating different messages for the 16-to-18 and 19-to-24 age groups. The younger group is high school age and more likely to live at home with parents; members of the older group are more likely to be working or in college, living on their own and less subject to parental authority. The panel also believes it may be worthwhile to educate preteen boys, their parents, and their schools to influence attitudes before problems begin. The messages might be the following: sleepiness is not inevitable for teens, and it is not okay to drive when you are sleepy.
The panel recognized that the risk-taking behaviors of younger men will be a challenge in developing successful educational approaches. Focus group research is needed to develop a better understanding of young men's perceptions of fall-asleep crash risk and the kinds of interventions that would be effective with this group. Based on the literature, however, the panel suggests that campaign designers consider the following message points, many of which are appropriate for all public audiences:
Sleepiness is a serious risk for young male drivers.
Although little is known about the knowledge and attitudes of this group regarding sleepiness and driving risk, surveys of the general population suggest that knowledge of the risk is likely to be low and awareness will need to be raised. It also will be important for messages to affect attitudes, so that young men and their parents believe the risk is serious and young men are vulnerable. Misconceptions that sleepiness is inevitable at this age and that chronic sleepiness is a safe lifestyle choice need to be overcome. Understanding the concept of sleep debt could be useful, as could recognizing the uncontrollable nature of falling asleep at high levels of drowsiness.
Driving between midnight and 6 a.m. is a high-risk situation.
Scheduling a trip at another time is a simple way to reduce risk, especially if the drive is long.
An active lifestyle that restricts sleep is a special risk.
Many young men will recognize themselves in the picture of a chronically sleepy student who also works part-time, participates in extracurricular activities, and has an active social life. The "all nighter" represents an acute risk because extreme tiredness follows one sleepless night. The recommended action is not to start a long drive after one or more sleepless nights (e.g., do not drive home from college the day your exams are over; get a good night's sleep first).
Drinking alcohol increases sleepiness, and the combination of alcohol and sleepiness decreases performance and increases risk, even at low levels of alcohol use.
A message that would convince young men not to drink when they are already sleepy could be useful. However, focus groups of youth in New York State revealed that drowsy-driving messages could be lost or ignored if paired with "don't drink and drive" messages, which some believe are already overemphasized (New York GTSC Sleep Task Force, 1994).
You can take effective steps if you become sleepy while driving.
These steps include stopping driving altogether, if possible; consuming the caffeine equivalent of two cups of coffee; taking a 20-minute nap, and after the nap, driving to the closest safe resting spot, such as a motel, friend's house, or home; and sleeping.
Successful strategies from drinking and driving campaigns might also be adapted to drowsy driving if focus groups confirm their appeal. For example, an educational campaign could suggest that teens call a friend or a parent for a ride or let a friend drive home instead of driving while sleepy. Complementary educational messages to parents might suggest that they tell teenagers to call for a ride at any hour without recriminations if they feel too sleepy to drive. In another alcohol strategy variation, parents might allow sleepy friends of teens to sleep over rather than drive home.
The campaign also could counter common misconceptions of useful "stay awake" behaviors, such as exercising, turning on the radio, or opening the windows, which have not been shown to prevent sleep attacks.
Messages to policymakers could promote the value of graduated driver licensing that does not permit younger drivers to drive during late night hours (e.g., after midnight). These leaders may need information on the drowsy-driving problem and the special risks of driving during this period for all drivers and especially for younger ones.

Promote Shoulder Rumble Strips as an Effective Countermeasure for Drowsy Driving; in this Context, Raise Public Awareness About Drowsy-Driving Risks and How to Reduce Them
The panel believes that focusing a campaign on shoulder rumble strips offers multiple educational opportunities to convey key drowsy-driving messages.
Messages to the general public can explain the following:
What rumble strips are and why they are increasingly being used.
A message that rumble strips are designed to arouse sleepy drivers before they drive off the road could be an attention-getting way to highlight the prevalence of chronic sleepiness and point out the risks and possible consequences of drowsy driving. People who have driven over a rumble strip in the past could personalize the risk, and even seeing the strips on the highway in the future could repeatedly remind people of the message.
What to do when awakened by driving over a rumble strip.
Rumble strips act as an alarm clock, alerting drivers to the fact that they are too impaired to drive safely. The key to safety is what the driver does after hearing the alarm. In the short term, risk-reducing actions include stopping immediately if possible (e.g., a more alert driver can take over); consuming the caffeine equivalent of two cups of coffee; and taking a 20-minute nap. Then the driver should get off the road (e.g., at a motel or rest stop) as soon as possible and sleep.
In the longer term, planning ahead can help people avoid driving while drowsy. Key steps include planning sleep and naps before long trips, scheduling trips to avoid midnight through 6 a.m. driving, and avoiding alcohol and sedating medicines while sleepy or sleep deprived.
The limitations of rumble strips.
Rumble strips should not give drivers a false sense of security about driving while sleepy. The strips are useful as alerting devices, but they will not protect drivers who continue to drive while drowsy. Being awakened by driving over a rumble strip is a warning to change sleep and driving behaviors for safety. The strips are not a technological quick fix for sleepy drivers.
Messages to policymakers, especially from States in which rumble strips are not currently used, can emphasize what rumble strips are, their relative cost-effectiveness, and why they are a valuable addition to highways in rural areas. Policymakers also may need information on the risks of drowsy driving and crashes to put the need for rumble strips in perspective.

Educate Shift Workers About the Risks of Drowsy Driving and How to Reduce Them
Employers, unions, and shift workers are potential target audiences for education on shift work and drowsy driving issues. The panel believes that an initial focus on employees would complement and reinforce other drowsy-driving messages directed to the public. Although many shift workers are not in a position to change or affect their fundamental work situation, they and their families may benefit from information on their risks for drowsy driving and effective countermeasures. Key message points include the following:
Shift work may increase the risk of drowsy-driving crashes.
Night-, early morning-, and rotating-shift workers are often sleepy because their work times are inconsistent with the natural sleep-wake cycle. Workers on these shifts routinely get less sleep and lower quality sleep than do day workers. Driving while sleepy is a risky behavior that leads to many serious crashes each year.
Driving between midnight and 6 a.m. and driving home immediately after an extended or night shift are special risks for a drowsy-driving crash.
Driving during late night/early morning hours increases risk for all drivers because those hours are a natural period of sleepiness. Many drowsy-driving crashes occur at this time. Driving while acutely tired, such as after a night shift, also increases the risk of crashing. Shift workers, many of whom are already chronically sleep deprived, are at extra risk.
You can take effective steps to reduce your risks.
First, it is important to give regular priority to getting good sleep by creating a quiet, cool, dark environment, allowing sufficient time for sleep, and trying to sleep during the same hours each day. Another strategy is to avoid driving home from work while sleepy (e.g., getting a ride from a family member, taking a cab, napping before heading home). Consuming caffeine equivalent to two cups of coffee may help improve alertness for a short period.

Other Organizations Can Provide Drowsy Driving Education
The panel recognizes that limitations in resources will not allow NCSDR/NHTSA to conduct all needed educational interventions. However, other sponsors can make an important contribution by disseminating messages to high-risk audiences, intermediaries, and gatekeepers, such as industries where shift work is prevalent. Potential sponsors may include consumer, voluntary, health care professional, and industry groups and other government agencies. The panel encourages such groups to use this report and resulting campaign materials to inform and assist their own audience-specific efforts. NCSDR/NHTSA efforts to educate the public, especially youth, about the importance of sleep and sleep hygiene should complement other initiatives and, in combination, reinforce messages on the prevention of fall-asleep crashes.
NCSDR/NHTSA EXPERT PANEL ON DRIVER FATIGUE AND SLEEPINESS
Kingman P. Strohl, M.D.
Panel Chairman
Director, Center for Sleep Disorders Research
Division of Pulmonary and Critical Care Medicine
Cleveland Veterans Administration Hospital
Jesse Blatt, Ph.D.
Senior Research Psychologist
Office of Research and Traffic Records
National Highway Traffic Safety Administration
Forrest Council, Ph.D.
Director
University of North Carolina
Highway Safety Research Center
Kate Georges
Special Assistant to Executive Deputy Commissioner
Department of Motor Vehicles
State of New York
James Kiley, Ph.D.
Director
National Center on Sleep Disorders Research
National Heart, Lung, and Blood Institute
National Institutes of Health
Roger Kurrus
Division Chief, Consumer Automotive Safety
Information Division
National Highway Traffic Safety Administration
Anne T. McCartt, Ph.D.
Deputy Director
Institute for Traffic Safety Management and Research
State of New York
|
Sharon L. Merritt, Ed.D., R.N.
Director
Department of Medical-Surgical Nursing
Center for Narcolepsy Research
University of Illinois
Allan I. Pack, Ph.D., M.D.
Director
Center for Sleep and Respiratory Neurobiology
University of Pennsylvania Medical Center
Susan Rogus, R.N., M.S.
Coordinator, Sleep Education Activities
Office of Prevention, Education, and Control
National Heart, Lung, and Blood Institute
Thomas Roth, Ph.D.
Division Head
Sleep Disorders and Research Center
Henry Ford Hospital
Jane Stutts, Ph.D.
Manager, Epidemiological Studies
University of North Carolina Highway Safety
Research Center
Pat Waller, Ph.D.
Director
University of Michigan Transportation Research
Institute
David Willis
President
AAA Foundation for Traffic Safety
|
References
- Åkerstedt T: Work hours, sleepiness and accidents: introduction and summary. J Sleep Res 1995(a);4(2):1-3.
- Åkerstedt T: Work hours, sleepiness and the underlying mechanisms. J Sleep Res 1995(b);4(2):15-22.
- Åkerstedt T: Work hours and sleepiness. Neurophysiol Clin 1995(c);25(6):367-75.
- Åkerstedt T, Ficca G: Alertness-enhancing drugs as a countermeasure to fatigue in irregular work hours. Chronobiol Int 1997;14:145-58.
- Åkerstedt T, Gillberg M: Subjective and objective sleepiness in the active individual. Int J Neurosci 1990;52:29-37.
- Åkerstedt T et al.: The subjective meaning of good sleep, an intraindividual approach using the Karolinska Sleep Diary. Percept Mot Skills 1994;79:287-96.
- Alaia S: Life effects of narcolepsy: measures of negative impact, social support, and physiological well-being. Loss Grief and Care 1992;5:1-22.
- Aldrich M: Automobile accidents in patients with sleep disorders. Sleep1989;12(6):487-94.
- Alpert M et al.: Sleep-disordered breathing and car accidents in the elderly. J Sleep Res 1992;21:167.
- American Association of State Highway and Transportation Officials: A policy on geometric design of highways and streets. Washington, DC:1995.
- American Thoracic Society: Sleep apnea, sleepiness, and driving risk. Am J Respir Crit Care Med 1994;50:1463-73.
- Arbus L et al.: Drowsiness and traffic accidents. Importance of diagnosis. Neurophysiol Clin 1991;21(1):39-43..27
- Broughton R et al.: Life effects of narcolepsy in 180 patients from North America, Asia and Europe compared to matched controls. Canadian Journal of Neurological Science 1981;8:299-304.
- Broughton R et al.: Comparison of the psychosocial effects of epilepsy and narcolepsy/cataplexy: a controlled study. Epilepsia 1984;25:423-33.
- Brown I: Driver Fatigue. Hum Factors 1994;36(2):298-314.
- Buysse D et al.: The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res 1989;28:193-213.
- Carskadon M: Adolescent sleepiness: increased risk in a high-risk population. Alcohol, Drugs and Driving 1990;5(4)/6(1):317-28.
- Carskadon M: Sleepiness in adolescents and young adults. Proceedings of the Highway Safety Forum on Fatigue, Sleep Disorders and Traffic Safety. State University of New York, Institute for Traffic Safety Management and Research; 1993(a) Dec 1. pp. 28-36.
- Carskadon M: Evaluation of excessive daytime sleepiness. Neurophysiol Clin 1993(b);23:91-100.
- Carskadon M, Dement WC: Cumulative effects of sleep restriction on daytime sleepiness. Psychophysiology 1981;18:107-13.
- Carskadon M, Dement WC: Daytime sleepiness: quantification of a behavioral state. Neurosci Biobehav Rev 1987;11:307-17.
- Carskadon M, Roth T: Sleep restriction. In: Monk T, editor. Sleep, sleepiness and performance. Chichester: John Wiley & Sons; 1991. pp. 155-67.
- Carskadon M et al.: Guidelines for the Multiple Sleep Latency Test: a standard measure of sleepiness. Sleep 1986;9:519-24.
- Cassel W et al.: Risk of traffic accidents in patients with sleep-disordered breathing: reduction with nasal CPAP. Eur Respir J 1996;9(12):2606-11.
- Ceutel C: Risk of traffic accident injury after a prescription for a benzodiazepine. Ann Epidemiol 1995;5(3):239-44.
- Czeisler C et al.: Exposure to bright light and darkness to treat physiologic maladaption to night work. N Engl J Med 1990;322(18):1253-9.
- Dinges D: Adult napping and its effects on ability to function. In: Stampi C, editor. Why we nap:evolution, chronobiology, and functions of polyphasic and ultrashort sleep. Boston: Birkhauser; 1992. pp. 118-34.
- Dinges D: An overview of sleepiness and accidents. J Sleep Res 1995;4(2):4-14.
- Dinges D et al.: Temporal placement of a nap for alertness: contributions of circadian phase and prior wakefulness. Sleep 1987;10:313-29.
- Dinges D et al.: Cumulative sleepiness, mood disturbance, and psychomotor vigilance performance decrements during a week of sleep restricted to 4-5 hours per night. Sleep 1997;20(4):267-77.
- Dinges D, Kribbs N: Performing while sleepy: effects of experimentally-induced sleepiness. In: Monk T, editor. Sleep, sleepiness, and performance. New York: John Wiley & Sons; 1991. pp. 98-128.
- Douglass A et al.: The Sleep Disorders Questionnaire I: creation and multivariate structure of SDQ.Sleep 1994;17:160-7.
- Douglass A et al.: Historical database, questionnaires, sleep and life cycle diaries. In Laughton E, Broughton R, editors. Medical monitor in home and work environment. New York: Raven Press; 1990.
- Federal Register: Motor vehicle safety standards: hours of service of drivers; proposed rule. Part VI Department of Transportation, 49CFR Part 395, November 5, 1996.
- Findley L: Vigilance and automobile accidents in patients with sleep apnea or narcolepsy. Chest 1995;108(3):619-24.
- Findley L et al.: Automobile accidents involving patients with obstructive sleep apnea. Am Rev Respir Dis 1988;138(2):337-40.
- Findley L et al.: Driving simulator performance in patients with sleep apnea. Am Rev Respir Dis 1989;140:529-30.
- Fox S: Coffee, caffeine and health. In: Members reference book, Royal College of General Practitioners. London; 1993. pp. 419-22.
- Frith W, Perkins W: The New Zealand graduated driver licensing system. New Zealand: Wellington; 1992.pp. 1-23.
- Garder P, Alexander J: Fatigue related accidents and continuous shoulder rumble strips. Presented at the Transportation Research Board's 74th Annual Meeting; 1995 January 22-28. Preprint Paper No. 95 01 32;1995.
- Gengo F, Manning C: A review of the effects of antihistamines on mental processes related to automobile driving. J Allergy Clin Immunol 1990;86:1034-9.
- George et al.: Sleep apnea patients have more automobile accidents. Lancet 1987 Aug 22:447.
- Gillberg M: Jet lag and sleepiness in aircrew. J Sleep Res 1995;4(2):37-40.
- Gold D et al.: Rotating shift work, sleep, and accidents related to sleepiness in hospital nurses. Am J Public Health 1992;82(7):1011-4.
- Griffiths R et al.: Low-dose caffeine discrimination in humans. J Pharmacol Exp Ther 1990;262:970-6.
- Hamilton P et al.: A study of four days partial sleep deprivation. In: Colquhoun W, editor. Aspects of human efficiency. London: English Universities Press, Ltd.; 1972. pp. 101-13..28
- Hanning C, Welch M: Sleepiness, snoring and driving habits. J Sleep Res 1996;5(1):51-4.
- Hansotia P: Sleep, sleep disorders and motor vehicle crashes. Wis Med J 1997;96(5):42-7.
- Haraldsson P et al.: Driving vigilance simulator test. Acta Otolaryngol (Stockh) 1990;110:136-40.
- Haraldsson P et al.: Long-term effect of uvulopalatopharyngoplasty on driving performance. Arch Otolaryngol Head Neck Surg 1995;121(1):90-4.
- Harma M: Individual differences in tolerance to shift work: a review. Ergonomics 1993;36(1-3):101-9.
- Hoddes E et al.: Quantification of sleepiness: a new approach. Psychophysiology 1973;10:431-6.
- Horne J: Why we sleep. Oxford: Oxford University Press; 1988. pp. 1-12.
- Horne J, Baumber C: Time-of-day effects of alcohol intake on simulated driving performance in women. Ergonomics 1991;34(11):1377-83.
- Horne J, Gibbons H: Effects on vigilance performance and sleepiness of alcohol given in the early afternoon (`post lunch') vs. early evening. Ergonomics 1991;34(1):67-77.
- Horne J, Reyner L: Driver sleepiness. J Sleep Res 1995(a);4(2):23-9.
- Horne J, Reyner L: Sleep related vehicle accidents. BMJ 1995(b) Mar 4;310:565-7.
- Hublin C et al.: Daytime sleepiness in an adult, Finnish population. J Intern Med 1996;239:417-23.
- Huntley M, Centybear T: Alcohol, sleep deprivation and driving speed effects upon control use during driving. Hum Factors 1974;16:19-28.
- Johns MW: A new method for measuring daytime sleepiness: the Epworth Sleepiness Scale. Sleep 1991;14:540-5.
- Kerr et al.: Separate and combined effects of the social drugs on psychomotor performance. Psychopharmacology 1991;104:113-19.
- Kessler E: Shift work: family impact and employer responses. Washington, DC: Bureau of National Affairs; 1992. BNA special report no. 32. pp. 1-32.
- Knipling R, Wang J: Crashes and fatalities related to driver drowsiness/fatigue. Research Note from the Office of Crash Avoidance Research. Washington, DC: National Highway Traffic Safety Administration; 1994 Nov. pp. 1-8.
- Knipling R, Wang J: Revised estimates of the U.S. drowsy driver crash problem size based on general estimates system case reviews. Association for the Advancement of Automotive Medicine, 39th Annual Proceedings; 1995 Oct 16-18.
- Kozena L et al.: Vigilance impairment after a single dose of benzodiazepines. Psychopharmacology (Berl) 1995;119(1):39-45.
- Kribbs N, Dinges D: Vigilance decrement and sleepiness. In: Harsh J, Ogilvie R, editors. Sleep onset mechanisms. Washington, DC: American Psychological Association; 1994. pp. 113-125.
- Langlois P et al.: Temporal patterns of reported single vehicle car and truck accidents in Texas, USA during 1980-83. Chronobiol Int 1985;2:131-40.
- Lavie P et al.: Frequency of sleep related traffic accidents and hour of the day. Sleep Res 1986;15:175.
- Leveille et al.: Psychoactive medications and injurious motor vehicle collisions involving older drivers. Epidemiology 1994;5:591-8.
- Lisper H et al.: Relation between time to falling asleep behind the wheel on a closed track and changes in subsidiary reaction time during prolonged driving on a motorway. Ergonomics 1986;29(3):445-53.
- Lorist M et al.: Influence of caffeine on selective attention in well-rested and fatigued subjects. Psychophysiology 1994;31:525-34..29
- Lumley M et al.: Ethanol and caffeine effects on daytime sleepiness alertness. Sleep 1987;10:306-12.
- McCartt A et al.: The scope and nature of the drowsy driving problem in New York state. Accident Analysis and Prevention 1996;28(4):511-17.
- Marcus C, Loughlin G: Effect of sleep deprivation on driving safety in housestaff. Sleep 1996;19(10):763-6.
- Martikainen K et al.: Daytime sleepiness: a risk factor in community life. Acta Neurol Scand 1992;86(4):337-41.
- Maycock G: Sleepiness and driving: the experience of UK car drivers. J Sleep Res 1996;5(220):220-37.
- Minors D, Waterhouse J: Anchor sleep as a synchronizer of rhythms on abnormal routines. Int J Chronobiol 1981;7:165-88.
- Mitler M et al.: Catastrophes, sleep, and public policy: consensus report. Sleep 1988;11(1):100-9.
- Mitler M et al.: Maintenance of wakefulness test: a polysomnographic technique for evaluating treatment efficacy in patients with excessive somnolence. Electroencephalogr Clin Neurophysiol 1982;53:658-61.
- Mitler M, Miller J: Methods of testing for sleeplessness. Behav Med 1996;21:171-83.
- Naitoh P: Minimal sleep to maintain performance: the search for sleep quantum in sustained operations. In: Stampi C, editor. Why we nap: evolution, chronobiology, and functions of polyphasic and ultrashort sleep. Boston: Birkhauser; 1992. pp. 199-216.
- National Commission on Sleep Disorders ResearchWake up America: a national sleep alert. 1993;1.
- National Sleep Foundation. Use of continuous shoulder rumble strips: consensus report. 1997 June. National Sleep Foundation. Survey: sleepiness in America. 1997. National Sleep Foundation. Survey: sleep in America. 1995.
- National Transportation Safety Board. Factors that affect fatigue in heavy truck accidents. Washington, DC: PB95-917001, NTSB/SS-95/01; 1995.
- New York GTSC Sleep Task Force, Public Information and Education Subcommittee. Drowsy driving focus group study: final report. 1994 Aug. New York State Task Force on Drowsy Driving. Status report. Institute for Traffic Safety Management and Research. 1996 May.
- Novak R, Auvil-Novak S: Focus group evaluation of night nurse shiftwork difficulties and coping strategies. Chronobiology International 1996 13(6):457-463.
- Ohayon M, Priest R, Caulet M, et al.: Snoring and breathing pauses during sleep: telephone interview survey of a United Kingdom population sample. BMJ 1997;314(7084):860-3.
- Pack A et al.: Characteristics of crashes attributed to the driver having fallen asleep. Accid Anal Prev 1995;27(6):769-75.
- Peeke S et al.: Combined effects of alcohol and sleep deprivation in normal young adults. Psychopharmacology 1980;67:279-87.
- Philip P et al.: Objective measurement of sleepiness in summer vacation long-distance drivers. Electroencephalogr Clin Neurophysiol 1997;102(5):383-89.
- Philip P et al.: Determinants of sleepiness in automobile drivers. J Psychosom Res 1996;41(3):279-88.
- Ray et al.: Psychoactive drugs and the risk of injurious motor vehicle crashes in elderly drivers. Am J Epidemiol 1992;136:873-83.
- Redelmeier D, Tibshirani R: Association between cellular telephone calls and motor vehicle collisions. N Engl J Med 1997;336(7):453-8.
- Regina E et al.: Effects of caffeine on alertness in simulated automobile driving. J Appl Psychol 1974;59(4):483-9-30
- Richardson G et al.: Circadian variation of sleep tendency in elderly and young adult subjects. Sleep 1982;5:S82-S94.
- Roehrs T et al.: Sleepiness and ethanol effects on simulated driving. Alcohol Clin Exp Res 1994;18(1):154-8.
- Rosa R: Editorial: factors for promoting adjustment to night and shift work. Work & Stress 1990;4:201-2.
- Rosekind M et al.: Alertness management: strategic naps in operational settings. J Sleep Res 1995;4(2): 62-66.
- Rosenthal L et al.: Level of sleepiness and total sleep time following various time in bed conditions. Sleep 1993(a);16:226-32.
- Rosenthal L et al.: The Sleep-Wake Activity Inventory: a self-report measure of daytime sleepiness. Biol Psychiatry 1993(b);34:810-20.
- Samel A et al.: Jet lag and sleepiness in aircrew. J Sleep Res 1995;4(2):30-6.
- Sharpley A: Impact of daytime sleepiness underrated. Lancet 1996;338:71.
- Stampi C: Sleep and circadian rhythms in space. J Clin Pharmacol 1994;34:518-34.
- Stradling J et al.: Self reported snoring and daytime sleepiness in men aged 35-65 years. Thorax 1991;46(11):807-10.
- Strohl KP, Redline S: State-of-the-art: recognition of obstructive sleep apnea. Am J Respir Crit Care Med 1996;154:279-89.
- Torsvali L, Åkerstedt T: Extreme sleepiness: quantification of EOG and spectral EEG parameters. Int J Neurosci 1988;38(3-4):435-41.
- Treat J et al.: Tri-level study of the causes of traffic accidents: final report. Volume I: Causal factor tabulations and assessments. Institute for Research in Public Safety, Indiana University; 1979. DOT Publication No.: DOT HS-805085.
- Van Laar M et al.: Acute and subchronic effects of nefazodone and imipramine on highway driving, cognitive functions, and daytime sleepiness in healthy adult and elderly subjects. J Clin Psychopharmacol 1995;15(1):30-40.
- Waller P: A graduated licensing system for beginning drivers. In: National Highway Traffic Safety Administration: provisional licensing programs for young drivers. Washington, DC; 1989. pp. 35-51.
- Wang J, Knipling R, Goodman M: The role of driver inattention in crashes: new statistics from the 1995 crashworthiness data system. Fortieth Annual Proceedings of the Association for the Advancement of Automotive Medicine; 1996 Oct 7-9. pp. 377-92.
- Weirwille et al.: Research on vehicle-based driver status/performance monitoring: development, validation, and refinement of algorithms for the detection of driver drowsiness. Final Report. Washington, DC: U.S. Department of Transportation, National Highway Traffic Safety Administration; 1994 Dec.
- Wewers M, Low N: A critical review of visual analogue scales in the measurement of clinical phenomena. Res Nurs Health 1990;13:227-36.
- Wilkins J et al.: Sleep- and fatigue-related motor vehicle crashes, with and without alcohol involvement. Presented at the 11th annual meeting of the Association of Professional Sleep Societies; 1997 June.
- Wilkinson R: Interaction of alcohol with incentive and sleep deprivation. J Exp Psychol 1968;76:632-9.
- Williams H et al.: Impaired performance with acute sleep loss. Psychol Monogr 1959;73:1-26.
- Wylie C et al.: Commercial motor vehicle driver fatigue and alertness study, technical summary. Montreal: Transportation Development Centre; Public Health Service National Institutes of Health National Heart, Lung, and Blood Institute U.S. Department of Transportation National Highway Traffic Safety Administration DOT HS 808 707 April 1998
| Source: |
U.S. Department of Health and Human Services
Public Health Service
National Institutes of Health National Heart Lung, and Blood Institute
September 1997. |



