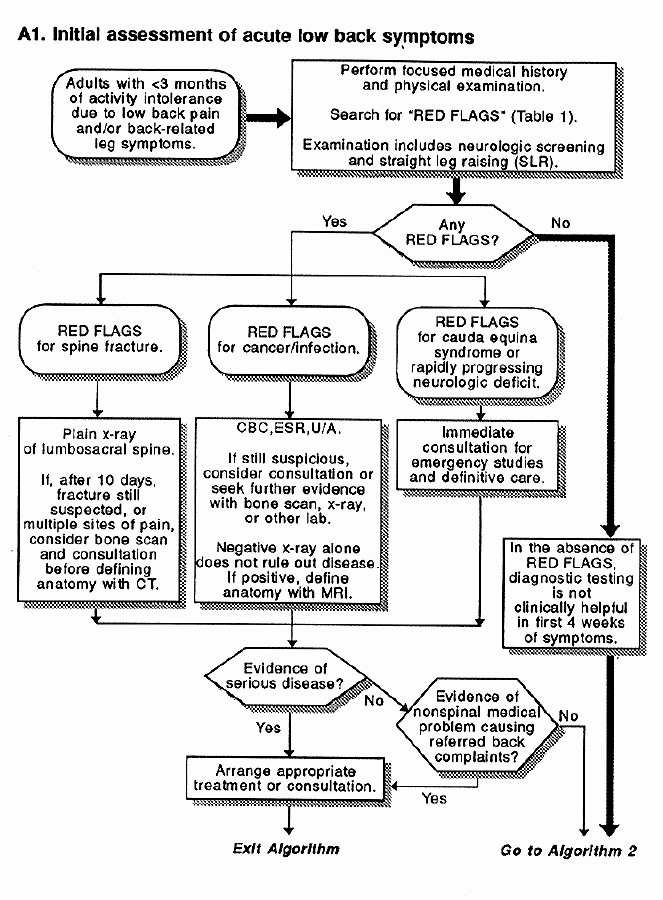
A1. Initial assessment of low back symptoms
| Contents | Previous | Next |
Acute low back problems, the subject of this Clinical Practice Guideline, are experienced by almost everyone at some time in their adult lives. Back problems rank high among the reasons for physician office visits and are costly in terms of medical treatment, time lost from work, and nonmonetary costs such as diminished ability to perform or enjoy usual activities. For persons under age 45, low back problems are the most frequent cause of disability.
The Agency for Health Care Policy and Research (AHCPR) convened a 23-member, multidisciplinary, private-sector panel to develop a guideline for the evaluation and treatment of acute low back problems in adults. The panel included physicians, nurses, chiropractors, experts in spine research, physical therapists, a psychologist, an occupational therapist, and a consumer representative. The panel defined back problems as activity intolerance due to back-related symptoms and acute as limitations of less than 3 months' duration. Back symptoms include pain, primarily in the back, as well as back-related leg pain (sciatica). The panel agreed that the guideline should provide primary care clinicians with information on the detection of serious spinal pathology (such as tumor or infection, spinal fracture or cauda equina syndrome) as well as nonspinal pathology that could be causing limitations due to low back symptoms, but that treatment of these conditions is outside the scope of the guideline.
Furthermore, the panel agreed that the assessment and treatment of patients younger than 18 years or those with chronic low back problems (back-related limitations lasting longer than 3 months) may be quite different than for adults with acute problems. For this reason, the panel decided that back problems in children as well as chronic low back problems are also outside the scope of the guideline.
The panel's overall intent was to change the paradigm of focusing care exclusively on the pain of low back problems to one of helping patients improve their activity tolerance. Findings and recommendation statements are based on an exhaustive and systematic review and analysis of the scientific literature as well as information gathered from the clinical experience of the expert panel, public testimony, peer review, and presetting in outpatient settings. This guideline is divided into an introduction and three chapters to correlate with the clinical approach:(1) Initial Assessment Methods(2) Clinical Care Methods(3) Special Studies and Diagnostic Considerations.
The initial assessment of a patient with activity intolerance due to low back symptoms consists of a focused medical history and physical examination. The primary purpose is to seek medical history responses or physical examination findings that suggest a serious underlying spinal condition such as fracture, tumor, infection, or cauda equina syndrome. These responses or findings are referred to as "red flags." The history and physical examination should also assess for nonspinal conditions (vascular, abdominal, urinary, or pelvic pathology) causing referred low back symptoms.
Once the clinician has ruled out red flags and nonspinal pathology, the symptoms can be categorized as either sciatica or nonspecific back pain. In the absence of red flags, neither routine nor special testing is required in the first month of symptoms for either category. Most of these patients will recover spontaneously from their activity limitations within 1 month.
In the absence of the red flags described above, most patients with activity intolerance due to an acute episode of low back symptoms can be treated similarly during the first month. The goals are to provide patients with accurate information about low back problems, assist with symptom relief, and make appropriate activity recommendations.
Once the history and physical examination are complete, the patient can be assured that there is no hint of a dangerous medical condition causing the back problem and that a rapid recovery is expected. Symptom control methods focus initially on providing the patient with a comfort level adequate to keep the patient as active as possible while awaiting spontaneous recovery. Later in treatment, symptom control is considered an adjunct in helping the patient overcome a specific activity intolerance. The primary methods of symptom control are oral pharmaceuticals and physical methods.
Among the oral medications available to control the discomfort of acute low back problems, the panel recommends acetaminophen as reasonably safe and acceptable. Nonsteroidal anti-inflammatory drugs (NSAIDs), including aspirin, are also acceptable despite the potential for side effects, most frequently gastrointestinal irritation. Muscle relaxants, including benzodiazepines, have been found no more effective than NSAIDs in treating patients with acute low back problems, and potential side effects of these drugs include drowsiness in up to 30 percent of patients. The panel recommended that opioids be avoided if possible because of significant risks of debilitation, drowsiness, decreased reaction time, clouded judgment, and potential misuse. If chosen, they should be used only for a short time. The panel also recommended against the use of oral steroids, colchicine, or antidepressant medications for acute low back problems.
The panel found manipulation to be a recommendable method of symptom control. Manipulation seems helpful for patients with acute low back problems without radiculopathy when used within the first month of symptoms. If no symptomatic and functional improvement has been noted after 1 month of manipulative therapy, this treatment should be stopped and the patient reevaluated. The panel found no evidence of benefit from the application of physical agents and modalities such as ice, heat, massage, traction, ultrasound, cutaneous laser treatment, transcutaneous electrical nerve stimulation (TENS), and biofeedback techniques. Self-application of heat or cold may be taught to patients who choose such options to provide temporary relief of symptoms. Evidence does not support the use of trigger point, ligamentous and facet joint injections, needle acupuncture, or dry needling as treatment for acute low back problems.
The panel found that prolonged bed rest (for more than 4 days) may lead to debilitation and is not appropriate in the treatment of acute low back problems. A gradual return to normal activities is advisable, although bed rest for 2 to 4 days may be an option for patients with severe initial symptoms of sciatica. The patient whose symptoms are aggravated by lifting or prolonged sitting may require specific advice and exploration of alternatives. For most patients, aerobic activities that minimally stress the back (such as walking, biking, or swimming) can be started during the first 2 weeks of acute low back problems. After this, conditioning exercises for trunk muscles (in particular back extensors) may be helpful, especially if the patient's acute low back problems persist, although such exercises may initially aggravate symptoms.
The panel recommended that clinicians consider a diagnostic reevaluation that may include special studies if the patient continues to be limited by back symptoms for more than 1 month without improvement. This reevaluation begins with a review and update of the history and physical exam to look again for red flags or evidence of nonspinal conditions causing back symptoms. If none of these is found, an appropriate evaluation can be initiated for either patients with sciatica or those with nonspecific low back symptoms.
For patients limited by sciatica for more than 4 weeks without clear evidence on physical examination of nerve root compromise, electromyography (EMG) and H-reflex tests of the lower limb may provide evidence of suspected neurologic dysfunction. Sensory evoked potentials (SEPs) may be a useful adjunct for assessment of suspected spinal stenosis or spinal cord myelopathy. For patients limited by sciatica for more than 4 weeks with physiologic evidence of neurologic dysfunction, MRI or CT is an appropriate consideration to provide anatomic definition of suspected herniated disc before surgery. Anatomic abnormalities of the lumbar spine (such as degenerative changes or abnormal discs) can be confusing since they increase in frequency as patients age and are often noted on imaging tests in subjects with no symptoms of low back problems. Abnormalities on imaging should corroborate evidence from physical examination or physiologic testing. A referral for surgical consultation is reasonable for patients with sciatic symptoms who have (1) activity limitations for more than 1 month without improvement, (2) clear clinical or electrophysiological evidence of nerve root compromise, and (3) corroborative findings on imaging studies. Earlier emergency consultation is reserved for patients with findings of bowel and/or bladder dysfunction or progressive and/or severe neurologic impairment. Most patients with symptoms persisting beyond 4 weeks will not be surgical candidates since the majority will have nonspecific acute low back symptoms without evidence of a serious underlying condition.
Following diagnostic or surgical procedures, treatment for those patients who have not recovered focuses on graduated physical conditioning to gain tolerance for activities required at home and/or the workplace. To help patients who have extreme difficulty overcoming their personal activity intolerance, clinicians are encouraged to address any nonphysical factors (such as unrealistic expectations by patient or employer or other psychosocial problems) that can potentially be influenced in a positive manner. The goal is to help the patient recover normal activity tolerance and avoid the development of a chronic low back disability.
There are four principal reasons acute low back problems were selected as a subject for guideline development. One reason is their prevalence. Most people report low back problems at some time in their lives, and national statistics indicate a general yearly prevalence in the U.S. population of 15-20 [1] percent. Among working-age people surveyed, 50 percent admit to back symptoms each year[2], [3] . Back symptoms, in fact, are the most common cause of disability for persons under age 45[4] . At any given time, about 1 percent of the U.S. population is chronically disabled because of back problems, and another 1 percent temporarily disabled. [1]
A second reason for a guideline on assessment and treatment of acute low back problems is cost. Low back problems are expensive. Their total costs to society are difficult to calculate, but evidence indicates that both the economic and psychosocial costs are substantial. Low back problems are the second most common symptomatic reason expressed by patients for office visits to primary care physicians [5]. They are the most common reason for office visits to orthopedic surgeons, neurosurgeons, and occupational medicine physicians. They rank third among the reasons for surgical procedures.
Moreover, although medical costs are high, loss of time from work as well as the disability payments for work-related low back problems can together cost up to three times as much as medical treatment. [6] About 2 percent of the U.S. work force has compensable back problems each year [7]. Various estimates of the total annual societal cost of back pain in the United States range from $20 to $50 billion. [8] No monetary costs of low back problems can also be substantial. The inability to function normally at work and in other daily activities has an impact on both patients and their families.
A third important reason for this guideline is the increasing evidence that many patients with activity intolerance due to low back symptoms may be receiving care that is inappropriate or at least less than optimal. Rates for hospitalization and surgery for low back problems vary substantially among regions of the United States as well as among small areas within states. [9]-[11] Marked regional variations also occur in the use of diagnostic tests for assessing low back problems. These variations imply a lack of consensus about appropriate assessment and treatment of low back problems, suggesting that some patients may be receiving inappropriate or suboptimal care.
In addition, some patients appear to be more disabled after treatment than before, another potential indicator of suboptimal care. Perhaps the most obvious examples involve surgery. Despite an extensive medical literature on failed back surgery and evidence that repeat surgical procedures for low back problems rarely lead to improved outcome, there are documented examples of patients who have had as many as 20 spine operations [9]. However, surgery is not the only treatment that can lead to increased disability. Common treatment methods such as extended bed rest or extended use of high-dose opioids can prolong symptoms and further debilitate patients.
A fourth reason for the guideline is a growing body of research on low back problems, allowing a systematic evaluation of commonly used assessment and treatment methods. Although the existing literature has shortcomings, there is sufficient scientific evidence for a number of conclusions about the efficacy and safety of current assessment and treatment methods.
Scope
This Clinical Practice Guideline is intended to provide primary care clinicians with information and recommended strategies for the assessment and treatment of acute low back problems in adults. To develop this guideline, AHCPR convened a private-sector, multidisciplinary panel of clinicians, researchers, and a consumer representative to evaluate the scientific evidence in the medical literature, draw conclusions, and make recommendations.
In determining the scope of the guideline, the panel focused on information needed for primary care assessment and treatment of adults with acute low back problems. "Back problems" were defined as activity intolerance due to back-related symptoms and acute as limitations of less than 3 months' duration. Back symptoms include pain in the back as well as back-related leg pain (sciatica). The panel agreed that the guideline should provide information on initial detection of underlying serious conditions (such as fracture, tumor, infection, or cauda equina syndrome) that could be causing low back problems, but that treatment of these conditions is outside the scope of the guideline.
The panel agreed further that the assessment and treatment of patients who have chronic low back problems (with symptoms lasting over 3 months) may be quite different than for patients with acute problems. Patients who become disabled due to chronic low back problems represent less than 5 percent of those with low back problems, but they account for up to 60 percent of the societal costs for this disorder. [6] To a much greater extent than acute problems, chronic low back problems are influenced by complex psychological, behavioral, socioeconomic, demographic, legal, and occupational factors, many of which are not easily controlled. [8] For these reasons, the panel decided that chronic low back problems are beyond the scope of a guideline on acute problems. The recommendations included in the guideline may not apply to persons younger than 18 years since diagnostic and treatment considerations for this group are often different than for adults.
Evaluation of Evidence
The panel agreed that this guideline on acute low back problems should be anchored to published scientific evidence, and that such evidence should take priority over panel opinion in making guideline recommendations. In looking at a proposed assessment or treatment method, the panel considered: (1) efficacy, (2) potential harms, and (3) costs.
The panel considered randomized controlled trials (RCTs) that focused on patient-oriented clinical outcome measures such as symptom relief or improved level of functioning to be the acceptable method for establishing the efficacy of treatment methods. Evidence about efficacy of assessment methods was considered adequate if results of the diagnostic test studied were compared to an independent reference standard in a way that allowed calculation of standard test parameters, such as the test's true-positive rate (sensitivity) and true-negative rate (specificity).
The panel agreed to give the greatest weight to scientific research evidence that met the above criteria. When such strong scientific evidence was not available, the panel labeled the evidence as weak and indirect and used the combined expert opinion and clinical judgment of panel members for interpretation. In all cases, the guideline explicitly states the type of evidence used by the panel as the basis for recommendations. The scale used for labeling the evidence is at the end of this chapter.
Prevention Studies
The panel found that, to date, studies of interventions aimed at preventing low back problems or their risk factors present conflicting findings and explain only a small portion of back complaints. Few of these prevention studies have been well designed, and most have been conducted in workplace settings focusing on injury claims or have used interventions that could not easily be carried out by primary care providers. When information from these studies was applicable to primary care, however, it was included under specific areas of assessment or treatment in the guidelines.
The panel agreed that a methodological problem commonly associated with studies of the prevention of back problems is lack of precision in specifying the goal (s) of the preventive intervention. Researchers often fail to establish whether the goal is to prevent the first episode of low back symptoms, activity limitations, recurrent episodes, injury claims, time lost from work, chronic disability, and/or medical care utilization and costs. In addition, some authors have suggested that efforts to prevent first or recurrent episodes of low back symptoms at work may be futile, and that research should focus instead on preventing long-term disability that results in high-cost disability claims. [6], [12], [13]
Organization and Clinical Categories
Chapter 2 of this guideline focuses on the initial assessment of the patient with activity limitations due to acute low back symptoms, and Chapter 3 addresses initial treatment methods for these patients. The assessment and treatment methods considered in these chapters can typically be managed by the primary care clinician. Up to 90 percent of patients with acute low back problems recover within 1 month from activity limitations due to symptoms. [6], [14], [15] Chapter 4 Addresses diagnostic and treatment considerations for the small percentage of patients who still have substantial symptoms or limitations after 1 month. Many of these diagnostic and therapeutic methods can be managed by the primary care clinician; others will require consultation with a specialist.
The panel recognized that different clinical disciplines use a variety of diagnostic labels that implicitly suggest a cause for low back symptoms. However, these labels are often unreliable for categorizing causes of acute low back problems. Even after an extensive workup, only about 15 percent of patients can be given a definitive diagnosis. [16]
Since the many diagnostic labels currently used to describe low back problems may confuse patients and clinicians, the panel considered it more useful to classify a patient's acute low back problem into one of three descriptive clinical categories based on medical history and physical examination findings:
In the panel's opinion, clinicians would have enough information to make appropriate decisions about initial assessment and treatment, as well as some hints about prognosis, after correctly classifying patients with low back problems into one of the above three categories. The panel used this classification scheme in making guideline recommendations about assessment and treatment methods.
The general theory and principles underlying development of clinical practice guidelines are presented in an Institute of Medicine report; [17] other reports published by AHCPR provide specific information on the clinical guideline development process. [18] These materials provided a starting point for developing the Clinical Practice Guideline on low back problems. AHCPR provided the general parameters for guideline development. The panel, aided by the methodologists and consultants, then independently determined the specific methodology for the project, directed the literature review, and developed the guideline findings and recommendations.
Formation of the Panel and Staff
AHCPR initiated formation of the panel and appointed its chairperson and members. Important considerations in the choice of panel members were: (1) demonstrated knowledge about low back problems, (2) representation of major clinical disciplines involved in back care, and (3) geographic diversity. Nominations were solicited through a Federal Register announcement and from professional and consumer organizations and persons interested in the care of patients with low back problems.
More than 200 individuals were nominated. AHCPR selected 23 representing the fields of biomechanical and spine research, chiropractic care, emergency medicine, family medicine, internal medicine, neurology, neurosurgery, occupational health nursing, occupational medicine, occupational therapy, orthopedics, osteopathic medicine, physical and rehabilitation medicine, physical therapy, psychology, rheumatology, and radiology.
The panel also included a consumer representative who had experienced low back problems, but did not work in the health care field. Several consultants with expertise in spine research, clinical care of low back problems, clinical epidemiology, and health economics were appointed to the panel. Two methodologists with experience in developing clinical practice guidelines were assigned to the panel by AHCPR. Both methodologists were physicians with MPH degrees, one an emergency medicine physician and one an internist. The methodologists aided the panel in determining the scope of the literature search and the criteria to be used for selecting articles for panel review.
The panel chair formed a research and support staff that included two physicians: a spine-fellowship-trained orthopedic surgeon and an occupational-medicine-trained physician with an MPH degree. National Library of Medicine representatives aided the staff in retrieving literature. The staff screened articles and constructed evidence tables for articles according to panel review criteria. These evidence tables and the original articles were presented to the panel for review and interpretation. The panel used this information as the basis for its guideline findings and recommendations.
Public Comment and Peer Review
An open forum was held early in the guideline development process to give interested individuals, organizations, and agencies the opportunity to present written or verbal testimony. Later in the process, drafts of the guideline were sent out for peer and pilot review. AHCPR selected peer and pilot reviewers from those who had expressed interest in the guideline, participated in the open forum, or were nominated by professional organizations or panel members.
Over 100 peer reviewers were selected based on their expertise in the care of low back problems. They were asked to evaluate the comprehensiveness of the literature review as well as the panel's findings and recommendations. The pilot reviewers who were selected represented a cross-section of primary care settings including private and group practices, health maintenance organizations, and occupational medicine clinics. They were asked to evaluate the practical applicability of the guideline in their own practice settings by using examples published in the Quick Reference Guide for Clinicians and by soliciting feedback from patients given the Consumer Version. The panel used comments from peer and pilot reviewers to guide final revisions of the guideline.
Literature Search
The panel initiated a comprehensive literature search of topics deemed applicable to low back problems. The Quebec Task Force on Spinal Disorders had previously published an evidence-based guideline on low back problems, based upon an exhaustive literature search through 1984. The bibliography from their report was the starting point in the literature search for this AHCPR guideline.
The literature search of articles published after 1984 was performed through the National Library of Medicine. Abstracts of 10,317 articles which met the search criteria were each independently evaluated by the orthopaedic surgeon and occupational medicine physician on the research staff. If either reviewer thought an article might be useful, the entire article was retrieved. A total of 3,918 articles (38 percent of all abstracts evaluated) was obtained for further evaluation.
Additional articles came from panel members, from the open forum process, and from unsolicited sources. All articles were entered in a comprehensive bibliography, classified by topic, and screened methodologically to determine if they contained information that might be useful to the panel.
Evaluation of Efficacy
In evaluating efficacy of assessment and treatment methods, the panel decided to focus on how each method affected clinical outcomes important to patients and society. Examples of such outcomes are symptoms, level of physical functioning, patient satisfaction, and morbidity and mortality (as complications of the assessment or treatment method). The panel dealt with costs, another outcome of interest to patients and society, as a separate issue. Cost was not considered when evaluating efficacy.
The panel used a standard methodology to identify and evaluate the best scientific evidence available on the efficacy of each assessment and treatment method, while focusing on clinical outcomes. This process included a systematic evaluation of each study's quality and its clinical applicability to patients with acute low back problems. The panel used this information to screen all articles, using minimum article selection criteria for efficacy. Articles meeting these minimum criteria were prioritized (giving priority to articles of higher quality and clinical applicability), and data from the higher priority articles were abstracted onto evidence tables.
The panel then reviewed the available data from both evidence tables and original articles to decide how much weight to give each study in developing the findings and recommendations statements for this guideline. The greatest weight was given to studies of high quality that evaluated adults with acute low back problems, although few such studies were found.
For most topics, the quality and clinical applicability of studies reviewed were limited. Inclusion and exclusion criteria for subjects were often either incompletely described or so broad that they allowed for wide variations in age, symptoms, symptom duration, examination findings, prior treatments, and other potentially confounding factors. Studies often inadequately described the baseline demographic and clinical characteristics of subjects. Many studies did not distinguish acute from chronic patients; others failed to either describe or control for factors known to cause significant variation in outcome (such as prior back surgery). Certain studies lacked appropriate statistical analysis or included too few subjects to attain adequate statistical power.
Evaluation of Potential Harms and Costs
Evaluating Harms
Since back problems are rarely life-threatening, the panel paid special attention to potential harms (side effects or complications) of assessment and treatment methods. Controlled trials evaluating treatment and assessment methods, however, seldom included enough subjects to detect rare but potentially serious complications. This information was found only in large case series or case reports. On the other hand, controlled trials of oral medications often included extensive information on side effects. Thus, accurate comparison of the relative risks of side effects and complications of different assessment and treatment methods was not possible.
A lack of published evidence about harms related to specific treatment or assessment methods does not mean that potential harms do not exist. In many instances, the side effects and complications of assessment and treatment methods have never been extensively studied or comprehensively reported. In addition, articles evaluating newer treatment and assessment methods are often written by advocates of these methods, who may tend to deemphasize the harms.
The panel felt it was important for both clinicians and patients to have a sense of potential harms relative to the potential benefits of these methods. Therefore, the panel considered information about potential harms from a variety of sources, including case series, case reports, cross-sectional surveys, clinical trials, and in some instances studies of patients who did not have low back problems. Finally, if no specific information was available from any of these sources, the panel generally considered whether the method was invasive or carried the potential for an allergic reaction.
Evaluating Costs
Both clinicians and patients need to consider relative costs of assessment and treatment methods before making informed decisions about care. Costs vary greatly, however, and the cost data on assessment and treatment methods for low back problems are limited. The unit cost of a service may vary within and between geographical regions. The aggregate cost of services also varies depending on the frequency and duration of services for the individual patient. Although costs of various medical services have generally increased in recent years, they have done so at inconsistent rates. Given these variations, the panel decided to make broad statements about whether methods appeared to be of low, moderate, or high cost, graded according to the following system (based on 1993 dollars):
This grading system provides no more than a rough comparison of costs, and the panel recognized that the divisions between cost categories are somewhat arbitrary. For example, some Americans may not consider a $199 expense that comes directly out of pocket to be "low cost."
Developing the Guideline Recommendations
To develop recommendations for each assessment and treatment method, the panel considered: (1) the quality and amount of evidence for efficacy, (2) the strength of the effect found for the method, (3) the consistency of findings between studies, (4) the clinical applicability of the evidence to adult patients with acute low back problems, and (5) any evidence on harms or costs. For each assessment and treatment method the panel then sought to answer the following questions:
- Benefit the patient?
- Harm the patient?
The development of findings and recommendations statements required the collective judgment of the panel in interpreting the available evidence. The panel rated the amount and quality of evidence supporting each guideline statement using the scale in the Figure below.
Panel ratings of available evidence supporting guideline statements
|
*Met minimal formal criteria for scientific methodology and relevance to population and specific method addressed in guideline statement.
This rating system (A, B, C, or D) is the basis for:
|
|
|
A1. Initial assessment of low back symptoms |
The initial assessment (Attachment A1) of a patient with activity intolerance due to acute low back symptoms consists of a focused medical history, a physical examination, and related decisions. A careful medical history and physical examination are critical. The primary purpose is to seek medical history responses or physical examination findings suggesting a serious underlying condition such as fracture, tumor, infection, or cauda equina syndrome. These responses or findings are referred to as red flags. They alert clinicians to the possibility that low back symptoms may be related to a dangerous condition. However, serious conditions presenting as low back problems are relatively rare.
The initial assessment categorizes back symptoms without red flags as either primarily back (nonneurologic) or sciatic (neurologic) and defines the duration of these symptoms to guide both what type of special studies may be considered and when they should be considered. In the absence of red flags, special tests are not usually required in the first month of low back symptoms because most patients recover from their activity limitations within 1 month.
The initial assessment also provides an opportunity for the clinician to establish rapport with the patient, to find out patient expectations, and to become aware of potential psychological and socioeconomic factors that can alter response to care.
Of the 214 articles screened for this topic, 34 met the article selection criteria for efficacy. [20]-[53]
The important points in these articles are well summarized in review articles by Deyo, Rainville, and Kent [54] and Waddell, Main, Morris, et al. [55] Both reviews elaborate on the reproducibility and accuracy of specific medical history findings (Table 1) and physical examination findings (Table 2) for assessing low back problems. Other articles not meeting selection criteria are cited where appropriate since they contain information used in formulating recommendations. [56-65]
| References | Disease to be detected | Medical history red flags | True-positive rate (sensitivity) | True-negative rate (specificity) |
| Deyo and Diehl[26] | Cancer | Age >= 50 | 0.77 | 0.71 |
| Previous cancer history | 0.31 | 0.98 | ||
| Unexplained weight loss | 0.15 | 0.94 | ||
| Failure to improve with 1 month of therapy | 0.31 | 0.90 | ||
| Bed rest no relief | > 0.90 | 0.46 | ||
| Duration of pain > 1 month | 0.5. | 0.81 | ||
| Age > 50 or history of cancer or unexplained weight loss or failure of conservative therapy | 1.0 | 0.60 | ||
| Waldvogel and Vasey[64] | Spinal osteomyelitis | Intravenous drug abuse, UTI, or skin infection | 0.40 | NA |
| Unpublished data[a] | Compression fracture | Age >= 50 | 0.84 | 0.61 |
| Age >= 70 | 0.22 | 0.96 | ||
| Trauma | 0.30 | 0.85 | ||
| Corticosteroid use | 0.06 | 0.995 | ||
| Deyo and Tsui-wu[59], Spangfort[63] | Herniated disc | Sciatica | 0.95 | 0.88 |
| Turner, Ersek, Herron, et al.[66] | Spinal stenosis | Pseudoclaudication | 0.60 | NA |
| Age >= 50 | 0.90 [b] | 0.70 | ||
| Gran[60] | Ankylosing spondylitis | Positive responses 4 out of 5 | 0.23 | 0.82 |
| Age at onset <= 40 | 1.00 | 0.07 | ||
| Pain not relieved in supine position | 0.80 | 0.49 | ||
| Morning back stiffness | 0.64 | 0.59 | ||
| Duration of pain >3 months | 0.17 | 0.54 | ||
|
||||
| References | Test | True-positive rate (sensitivity) | True-negative rate (specificity) | Comments |
| Hakelius and Hindmarsh[61]; Kosteljanetz, Espersen, Halaburt, et al.[37] | Ipsilateral SLR | 0.80 | 0.40 | Positive result: leg pain at < 60 degrees |
| Hakelius and Hindmarsh[61]; Spangfort[63] | Crossed SLR | 0.25 | 0.90 | Positive result: reproduction of contralateral pain |
| Hakelius and Hindmarsh[61]; Spangfort[63] | Ankle dorsiflexion weakness | 0.35 | 0.70 | HNP usually at L4-L5 (80 degrees) |
| Hakelius and Hindmarsh[61]; Kortelainen, Puranen, Koivisto, et al.[35] | Great toe extensor weakness | 0.50 | 0.70 | HNP usually at L5-S1 (60 degrees) or L4-L5 (30 degrees) |
| Hakelius and Hindmarsh[61]; Spangfort[63] | Impaired ankle reflex | 0.50 | 0.60 | HNP usually at L5-S1; absent reflex increases specificity |
| Kortelainen, Puranen, Koivisto, et al.[35]; Espersen, Halaburt, et al.[37] | Sensory loss | 0.50 | 0.50 | Area of loss poor predictor of HNP level |
| Aronson and Dunsmore[56] | Patellar reflex | 0.50 | NA | For upper lumbar HNP only |
| Hakelius and Hindmarsh[61] | Ankle plantar flexion weakness | 0.06 | 0.95 | |
| Hakelius and Hindmarsh[61] | Quadriceps weakness | < 0.01 | 0.99 | |
| Note: Sensitivity and specificity were calculated by Deyo, Rainville, and Kent.[54] Values represent rounded averages where multiple references were available. All results are from surgical case series. HNP = herniated nucleus pulposous. SLR = straight leg raising. | ||||
Medical History
A few key questions on the medical history can help ensure that a serious underlying condition, such as cancer or spinal infection, will not be missed. These questions include: age, history of cancer, unexplained weight loss, immunosuppression, duration of symptoms, responsiveness to previous therapy, pain that is worse at rest, history of intravenous drug use, and urinary or other infection.
Symptoms of sciatica (leg pain) or neurogenic claudication (walking limitations due to leg pain) suggest possible neurologic involvement. Pain radiating below the knee is more likely to indicate a true radiculopathy than pain radiating only to the posterior thigh. A history of persistent numbness or weakness in the leg (s) further increases the likelihood of neurologic involvement. The articles indicate that cauda equina syndrome can be ruled out with a medical history that ascertains the absence of bladder dysfunction (usually urinary retention or overflow incontinence), saddle anesthesia, and unilateral or bilateral leg pain and weakness.
Patients' reports of symptoms and treatment outcomes may be influenced by psychological or socioeconomic factors. Several studies have reported a variety of such factors for patients with low back problems. These factors include work status, typical job tasks, educational level, pending litigation, worker's compensation or disability issues, failed previous treatments, substance abuse, and depression. [23], [38], [39], [41], [43], [50], [58]
Clinicians are urged by some authors to augment the medical history with pain drawings and visual analog pain rating scales to document the distribution of pain and intensity of symptoms (Attachment B). [40], [45], [46], [52], [53]
|
|
|
B1. Visual analog scale |
|
|
|
B2. Pain drawing |
Physical Examination
The physical examination supplements the information obtained in the medical history in seeking an underlying serious condition or possible neurologic compromise. The basic elements of a physical examination are inspection, palpation, observation including range of motion testing, and a specialized neuromuscular evaluation. This evaluation emphasizes ankle and knee reflexes, ankle and great toe dorsiflexion strength, and distribution of sensory complaints. For patients presenting with acute low back problems and no limb complaints, a more elaborate neurologic evaluation is usually not necessary.
The physical examination is less useful than the history in searching for underlying serious conditions such as cancer, but may be helpful in detecting spinal infections. Fever, vertebral tenderness, and very limited spinal range of motion suggest the possibility of spinal infections, but these are also common findings in patients without infection. Otherwise, evaluation of spinal range of motion has been found to be of limited diagnostic value, [62] although some clinicians consider it helpful in planning and monitoring treatment.
Findings from both the history and physical examination provide useful information in the search for possible neurologic compromise. For example, sciatica has such a high true-positive rate for lumbar nerve root compression that its absence makes a clinically important lumbar disc herniation related to neural compression unlikely. In addition, leg pain usually overshadows back pain when such a clinically significant radiculopathy is present. Finally, crossed straight leg raising is such a highly specific test that a positive finding makes neurologic compromise due to herniated lumbar disc very likely, but this is not a sensitive test since discomfort upon crossed straight leg raising may be absent in many patients with neurologic compression. [31], [34], [61], [63]
Deyo, Rainville, and Kent's summary of available data suggests that in the primary care setting for patients with leg symptoms, the neurologic examination can safely be limited to a few tests. These are: (1) testing of dorsiflexion strength of the ankle and the great toe, with weakness suggesting L5 and some L4 root dysfunction; (2) testing of ankle reflexes to evaluate S1 root dysfunction; (3) testing of light touch sensation in the medial (L4), dorsal (L5), and lateral (S1) aspects of the foot; and (4) the straight leg raising (SLR) test.
This abbreviated neurologic examination of the lower extremities will allow detection of most clinically significant nerve root compromise due to L4-L5 or L5-S1 disc herniations, which together make up over 90 percent of all clinically significant radiculopathy due to lumbar disc herniations. [35], [37], [56], [61], [63] Although this limited examination might miss the much less common L2-L3 or L3-L4 disc herniations, these conditions are more difficult to diagnose on physical examination. Moreover, if such patients have not improved by 1 month, this guideline suggests a further diagnostic workup or consultation (Chapter 4), which may clarify the diagnosis. For over 95 percent of patients with acute low back problems, no special interventions or diagnostic tests would be required within the first month of symptoms.
Potential harms and costs are considered low for both the medical history and the physical examination.
Summary of Findings
Positive answers to key medical history questions, in addition to positive findings on physical examination and/or simple lab tests, are red flags that suggest the possibility of a serious underlying condition as the cause of acute low back problems.
For cancer or infection, red flags are: history of cancer, unexplained weight loss, immunosuppression, urinary infection, intravenous drug use, prolonged use of corticosteroids, back pain not improved with rest, and age of patient over 50.
For spinal fracture, red flags are: history of significant trauma (for example, a fall from a height, motor vehicle accident, or direct blow to the back for a young adult, or a minor fall or heavy lift in a potentially osteoporotic or elderly individual), prolonged use of steroids, and age over 70.
For cauda equina syndrome or severe neurologic compromise, red flags are: medical history or physical examination findings of acute onset of urinary retention or overflow incontinence, loss of anal sphincter tone or fecal incontinence, saddle anesthesia (about the anus, perineum, and genitals), and global or progressive motor weakness in the lower limbs.
There are indications in the literature that psychological or socioeconomic factors may affect a patient's report of symptoms and response to treatment.
Simple laboratory tests, including complete blood count (CBC) and erythrocyte sedimentation rate (ESR), are sufficiently inexpensive and efficacious for use as initial tests when there is suspicion of back-related tumor or infection.
In the absence of red flags, treatment is similar for most patients with activity intolerance due to an acute episode of low back symptoms (Attachment A2). After assuring the patient that there is no hint of a dangerous problem and that a rapid recovery is expected, the goals are to provide accurate patient information about low back problems, to help provide comfort by means of symptom control methods, and to recommend activity modifications.
|
|
|
A2. Treatment of acute low back problems on initial and follow-up visits |
Patient Education About Low Back Symptoms
Panel findings and recommendations:
Patients with acute low back problems should be given accurate information about the following (Strength of Evidence = B): Expectations for both rapid recovery and recurrence of symptoms based on natural history of low back symptoms. Safe and effective methods of symptom control. Safe and reasonable activity modifications. Best means of limiting recurrent low back problems. The lack of need for special investigations unless red flags are present. Effectiveness and risks of commonly available diagnostic and further treatment measures to be considered should symptoms persist.
Patient education as defined here includes all forms of patient-oriented education about low back problems except for "back schools" (formally structured, classroom-style back education programs). Under this definition, patient education includes printed and audiovisual materials, information given by health care providers, and educational programs that are less formal than back schools.
Literature Reviewed
Of 14 articles screened for this topic, 2 met the criteria for review. [67], [68] Other articles contained information used by the panel, but did not meet article selection criteria. [69]- [71]
Neither of the studies meeting the criteria focused solely on patients with acute low back problems. Both evaluated patients with low back problems of unspecified duration. Interventions evaluated included giving patients booklets on back pain and holding a brief individual educational session during an emergency room visit or by phone after the visit.
Evidence on Efficacy.
Jones, Jones, and Katz [67] evaluated educational intervention for patients with low back problems who came to a hospital emergency department and were referred for follow-up care. Patients receiving an educational intervention in the emergency department and/or a follow-up phone call were more likely than control patients to schedule and keep their follow-up appointment.
Roland and Dixon [68] conducted a randomized controlled trial (RCT) in which patients presenting with low back problems were assigned either to a group receiving an educational booklet on back problems or to a control group receiving no educational materials. In the first 2 weeks after the intervention, no differences were found between the education and control groups in number of consultations for back pain. However, in the period from 2 weeks to 1 year after the intervention, significantly fewer patients in the group receiving the booklet consulted physicians for back pain.
The importance of providing information to the patient is indicated in a study by Deyo and Diehl. [70] Failure to receive an explanation of the problem was the most frequently cited source of patient dissatisfaction among 140 patients with low back problems. Patients who felt they did not receive an adequate explanation wanted more diagnostic tests, were less satisfied with their visit, and were less likely to want the same doctor again, compared with patients who reported an adequate explanation.
Thomas [71] randomly assigned patients with symptoms (including low back pain), but no definite diagnosis, to one of four consultations: either one of two positive consultations, with and without treatment, or one of two negative consultations, with and without treatment. In the positive consultations, patients were given a firm diagnosis and told confidently that they would be better in a few days. The negative consultations were devised so that no firm assurance was given. Two weeks later the difference in recovery was significant between the positive and negative groups, but not between the treated and untreated groups.
A study of patients visiting family physicians for common symptoms, including back or neck pain, found that gaining patient agreement about the nature of the problem led to earlier resolution.
Potential Harms and Costs
The potential risks, harms, and costs of educating patients are considered to below.
Summary of Findings
Evidence indicates that educating patients about back problems may reduce use of medical resources, decrease patient apprehension, and speed recovery.
Structured Patient Education: Back School
Panel findings and recommendations:
Back school is defined here as a structured program of education about low back problems, usually in a group setting. The therapeutic objectives are to give the patient information on the anatomy and natural history of disorders of the back; to teach the principles underlying posture, daily activities, and sports; and thereby to increase functional work capacity.
Literature Reviewed
Of 35 articles screened for this topic, 15 reporting on 12 RCTs met criteria for review. [72]- [86]
Two meta-analyses regarding back schools were also examined. [87,88] The panel used information from one other study that did not meet selection criteria. [89]
Evidence on Efficacy
One of the few studies demonstrating the efficacy of back school [72] was conducted in the medical department of a Swedish automotive assembly plant. The 217 subjects all had nonspecific low back pain for less than 3 months and were randomly assigned to one of three interventions: back school, combined physiotherapy exercise, or placebo shortwave diathermy. The back school intervention consisted of four 45-minute sessions in 2 weeks and included the following topics: anatomy and causes of low back problems, muscle function and posture, ergonomics, and advice on physical activity. Patients attending back school had a shorter duration of sick leave during the initial episode than the other two treatment groups, but at the 1-year follow-up neither the number nor the length of absences from work owing to recurrences differed among the three treatment groups.
A meta-analysis by Keijsers, Bouter, and Meertens [87] evaluated eight studies of back schools done in group settings. [72,73,76,79,81,85,86,89] These studies of back schools were compared in terms of program duration and content, patient selection criteria, number of patients, interventions, and outcome measures used. All eight studies were found to have major methodological problems. The authors found that although there was insufficient evidence to form a strong and valid judgment on the efficacy of back schools, the available evidence suggested that back schools are at most marginally effective.
Another meta-analysis by Linton and Kamwendo [88] reviewed the scientific literature on back schools and reported some positive effects in studies of patients with acute back pain. However, the authors found that most studies of back schools lacked adequate control groups and that the evidence on efficacy is inconclusive.
Potential Harms and Costs
The potential risks and harms of back schools are considered low. Costs are variable, depending on the number of sessions and the setting, and range from moderately inexpensive to expensive.
Summary of Findings
Available data on formal patient education programs, or back schools, vary in terms of program quality, length, content, costs, and outcomes. Only one study of a structured low back education program, performed in industry, was found to have a positive short-term impact on acute low back problems although no effect was seen at 1-year follow-up. [72] In summary, the published evidence on back school as a treatment for acute low back problems is limited in quantity and the results are contradictory.
Symptom control methods focus initially on providing comfort to keep the patient as active as possible while awaiting spontaneous recovery and, later in treatment, on aiding the activation needed to overcome a specific activity intolerance. The methods traditionally include oral medications, such as acetaminophen and nonsteroidal anti-inflammatory drugs (NSAIDs), as well as physical treatments. They also include therapeutic injections. Proving the efficacy of these methods to relieve acute low back symptoms is difficult due to the rapid rate of spontaneous recovery. The use of symptom control methods known to have less risk of harm than methods with proven efficacy may thus be warranted if such methods are inexpensive and allow an individual to remain active or build activity tolerance through exercise.
Symptom Control: Medications
Acetaminophen and NSAIDs
Panel findings and recommendations:
Acetaminophen, a nonnarcotic analgesic, has commonly been regarded as having an analgesic effect, but little or no known anti-inflammatory mechanism. The therapeutic objective for its use in acute low back problems is pain relief.
NSAIDs are a class of medications, including aspirin, ibuprofen, indomethacin, phenylbutazone, and a variety of other drugs. They have anti-inflammatory and analgesic properties as well as being prostaglandin inhibitors. The therapeutic objective of NSAIDs in treating acute low back problems is to decrease pain, presumably by reducing inflammation and promoting healing.
Literature Reviewed
Of 50 articles screened for this topic, 4 RCTs met the review criteria for adequate evidence about efficacy. [85], [90] - [92] Other articles did not meet the criteria, but contained information used by the panel. [93]- [103]
Evidence on Efficacy
The four RCTs that met review criteria for this topic were all double-blind studies comparing NSAIDs with a placebo in treating patients with low back problems. No studies were found that compared acetaminophen to placebo in treatment of patients with low back pain.
Two studies compared a single NSAID to a placebo: Amlie, Weber, and Holme [90] evaluated piroxicam. Postacchini, Facchini, and Palieri [85] evaluated diclofenac. The study by Berry, Bloom, Hamilton, et al. [92] had three treatment groups evaluating either one of two NSAIDs (diflunisal or naproxen sodium) or a placebo. The study by Basmajian [91] compared four treatment groups receiving an NSAID alone (diflunisal), a muscle relaxant alone (cyclobenzaprine), the two in combination, or a placebo.
Three of the studies evaluated patients with acute low back symptoms of less than 3 months' duration. Berry, Bloom, Hamilton, et al. [92] evaluated patients with chronic low back pain.
Three studies found NSAIDs superior to a placebo for pain relief in the short term: from 1 week to 2 months of symptom duration. [85,90,92] The remaining study found no significant difference between NSAID and placebo in terms of pain improvement scores. [91]
Although there were no RCTs comparing acetaminophen to placebo for patients with low back pain, one nonplacebo-controlled RCT found an NSAID (diflunisal) superior to paracetamol (which is similar to acetaminophen) in producing pain relief for patients with chronic low back pain. [97] In addition, the literature on acetaminophen does show it to be more effective than placebo in studies of patients with nonback-related pain. [98], [102]
Several RCTs comparing efficacy of different NSAIDs in the same study have found no NSAID to be consistently more effective than the others. [96,101,102] However, these studies also suggest that individual patients report better pain relief from some NSAIDs compared with others. For this reason, Brooks and Day [93] suggest that patients change to a different NSAID if no relief is reported after a 2-week trial.
Potential Harms and Costs
The risks from the use of acetaminophen at usual doses are low. [95] However, high doses of acetaminophen can lead to liver damage, and massive single doses sometimes lead to fatal hepatic necrosis. Compared with NSAIDs, acetaminophen has a minimal effect on platelets and few gastrointestinal side effects since it is not a mucosal irritant. Acetaminophen is inexpensive. The expense of treatment with NSAIDs varies greatly, depending on the medication used and the length of treatment.
Potential complications of NSAIDs have been extensively studied. [93], [95] These include gastritis and other gastrointestinal complaints, including bleeding in 20 to 30 percent of those patients with active peptic ulcer problems. The degree of gastrointestinal side effects from NSAIDs appears to be dose related, but side effects can occur with one tablet. Ingestion of NSAIDs with meals or in combination with antacids has not been proven effective in reducing these gastrointestinal side effects. However, one medication (misoprostol), when taken with NSAIDs, has been shown to reduce NSAID-induced gastric erosion and the risk for gastroduodenal ulcers. [99], [100]
NSAIDs interfere with platelet adhesion and renal sodium metabolism. Their use in patients with a bleeding diathesis is considered contraindicated. They can be used in the presence of hypertension, renal disease, and edematous states, but only if great caution is exercised. [93] For these reasons, some experts caution that routine blood tests (such as CBC and serum chemistry screen) be done before treatment for older patients or those with vascular disease. These tests are also recommended if there is any suspicion of complications for those patients on prolonged NSAID therapy. [95]
Phenylbutazone has been associated with bone marrow suppression (aplastic anemia and agranulocytosis). Indomethacin has a higher reported incidence of gastrointestinal side effects than other NSAIDs. Otherwise, there is no significant demonstrated difference between remaining NSAID preparations in terms of the prevalence or severity of complications. [95]
Summary of Findings
There is fair to good evidence that NSAIDs are effective for reducing pain in patients with acute low back problems. Although no studies were found comparing acetaminophen to placebo in patients with back pain, there is evidence that acetaminophen is comparable in efficacy to NSAIDs for treating back problems and with fewer side effects. In studies of patients with nonback pain, no consistent difference in symptom relief has been demonstrated between acetaminophen and any available NSAID (including aspirin). Both NSAIDs and acetaminophen have been found to be generally adequate to achieve pain relief.
Muscle Relaxants
Panel findings and recommendations:
Muscle relaxants are commonly used for the treatment of low back problems. Pharmacologically, these are usually benzodiazepines, other sedative medications, or antihistamine derivatives. The therapeutic objective of muscle relaxants is to reduce low back pain by relieving muscle spasm. However, the concept of skeletal muscle spasm is not universally accepted as a cause of symptoms, and the most commonly used muscle relaxants have no peripheral effect on muscle spasm.
Literature Reviewed
Of 42 articles screened for this topic, 12 RCTs met review criteria for adequate evidence about efficacy. [91,[104- 114]
Evidence on Efficacy
Three studies evaluating patients with low back problems either did not specify duration of symptoms or included a mix of patients with acute and chronic problems. [104,113,114] The remaining nine studies evaluated only patients with acute low back problems.
Of the articles that met review criteria, 9 evaluated a muscle relaxant compared with a placebo. [91,104,105,108-113] Two studies compared two different muscle relaxants. [107], [114] Some of the studies also compared a muscle relaxant to another medication, including a barbiturate; [110], [111] an NSAID; [91], [106] and acetaminophen. [91]
Of the nine studies comparing muscle relaxants with placebos, seven had results favoring the muscle relaxant. [104], [105], [108] - [111], [113] Two showed no difference in outcomes between muscle relaxant and placebo. [91], [112] In most studies, the positive effect for muscle relaxants was short-lived, lasting no more than 4 to 7 days, with no significant difference from placebo seen after this time.
Panel methodologists did a meta-analysis of the 12 studies that met panel review criteria. The studies were assessed for quality without knowledge of the results. There was one excellent study, [107] three good studies, [105], [109], [114] and eight fair studies. [91], [104], [106], [108], [110] - [113]
Each study was examined for outcome measures such as pain, functional capacity, or a global measure of improvement. When meta-analytically combined, the studies showed a trend toward greater improvement in the patients treated with muscle relaxants, but did not reach statistical significance. Even if the findings had reached significance, statistical combinations of such study results should be interpreted with caution. The conclusion of the meta-analysis was that muscle relaxants are probably, but not certainly, more effective than placebos in decreasing symptoms of acute low back problems. However, there was not enough evidence to determine whether muscle relaxants are more or less effective than NSAIDs for reducing symptoms or whether the addition of a muscle relaxant adds to the efficacy of an NSAID.
Potential Harms and Costs
Potential complications of muscle relaxants include drowsiness and dizziness, reported to be up to 30 percent higher in patients taking muscle relaxants compared with patients taking placebos. [91], [104], [105], [108] - [113] The cost of muscle relaxants is considered low to moderate.
Summary of Findings
There is moderate research evidence that muscle relaxants are more effective than placebo, but no evidence that they are better than NSAIDs, in relieving symptoms of acute low back problems. These medications have substantial potential side effects, especially a high incidence of drowsiness.
Opioid Analgesics
Panel findings and recommendations:
Oral opioid analgesics commonly given to patients with acute low back problems include morphine derivatives (opioids) and synthetic opioids. The therapeutic objective in treating low back problems is temporary pain relief.
Literature Reviewed
No RCTs were found that compared opioid analgesics (either alone or in combination with other drugs) to a placebo. Therefore, three studies were evaluated that compared opioid analgesics to other medications, [115] - [117] recognizing that results of the evaluation would not entirely answer the question of whether opioids are any better than placebo for back symptoms. Another article [118] contained information used by the panel.
Evidence on Efficacy
All three studies evaluated patients with acute low back problems, but with a mixed group of medications. Two reports compared acetaminophen with codeine to diflunisal (an NSAID) with patients treated for 1 and 2 weeks, respectively. [115], [116] The third study compared three groups, one group receiving codeine, one oxycodone plus aspirin, and one acetaminophen. [117]
At the conclusion of treatment, Muncie, King, and DeForge [116] and Brown, Bodison, Dixon, et al. [115] found no significant differences between groups in terms of pain relief or functional improvement.
Wiesel, Cuckler, Deluca, et al., [117] who evaluated a population of military recruits with acute low back pain, found no difference between the three medication groups in amount of time before patients returned to full activities. Pain relief was claimed to be superior in groups receiving opioid analgesics compared with acetaminophen, with the greatest effect seen in the first 3 days of treatment. No statistics were reported to support the claim.
Potential Harms and Costs
Side effects reported by subjects receiving acetaminophen with codeine included dizziness, fatigue, inability to concentrate, impaired vision, drowsiness, nausea, and constipation. [115], [116] In one study, 35 percent of subjects receiving acetaminophen with codeine had to discontinue the medication because of intolerable side effects. [116] Prolonged use of opioid analgesics is associated with the development of tolerance and physical dependence. A risk of developing physical dependence with short-term use of opioids has also been reported. [118]
The expense of treatment with these medications varies greatly, depending on the medication used and the length of treatment.
Summary of Findings
There are no well-designed controlled studies that evaluate the use of opioid analgesics compared with no treatment in patients with acute low back problems. The studies reviewed found that patients taking opioid analgesics did not return to full activity sooner than patients taking NSAIDs or acetaminophen. In addition, two studies found no difference in pain relief between NSAIDs and opioids. Finally, side effects of opioid analgesics were found to be substantial, including the risk for physical dependence. These side effects are an important concern in conditions that can become chronic, such as low back problems.
Oral Steroids
Panel findings and recommendations:
Oral steroids (corticosteroids) are used by some clinicians in the treatment of patients with acute low back problems. The therapeutic objective is to reduce inflammation in an attempt to promote healing and reduce pain.
Literature Reviewed
Of six articles screened for this topic, the only one meeting criteria for review was Haimovic and Beresford. [119] Two other articles also contained information used by the panel.
Evidence on Efficacy
Haimovic and Beresford, [119] in a double-blind RCT, evaluated patients with low back pain who had findings of a single nerve root irritation (symptom duration of patients not specified). Patients were randomly assigned to receive a 1-week course of either an oral dexamethasone or a placebo. On follow-up at the end of treatment and at 1 year, no significant differences were found between the two groups in terms of pain relief.
Potential Harms and Costs
The incidence of side effects associated with steroids correlates with the potency of the drug, dosage, and duration of administration. Well-recognized complications from the prolonged use of oral steroids include suppression of pituitary-adrenal function, fluid and electrolyte disturbance, hyperglycemia, demineralization of bone, and immunosuppression (with increased susceptibility to infection). While many of these effects can be reduced or eliminated with alternate-day therapy, even short-term daily use of high-dose steroids can contribute to posterior subcapsular cataract formation, myopathy, central nervous system disturbance, and avascular necrosis of bone, especially of the femoral head.
The expense of treatment varies greatly, depending on the medication used and the length of treatment.
Summary of Findings
The limited available research evidence indicates that oral steroids do not appear to be an effective treatment for patients with acute low back problems. Serious potential complications are associated with long-term use, but potential complications appear minimal with short-term use.
Colchicine
Panel findings and recommendations:
Colchicine has been used primarily to treat acute attacks of gouty arthritis and can be administered intravenously or orally. The therapeutic objective of using the drug in patients with acute low back problems is to reduce inflammation and thereby reduce pain.
Literature Reviewed
Of 13 articles screened, 3 RCTs met criteria for review. Schnebel and Simmons evaluated only patients with acute low back problems of less than 3 months' duration. Meek, Giudice, McFadden, et al. Evaluated patients with symptoms of more than 2 months. Simmons, Harris, Koulisis, et al. [124] evaluated those with symptoms lasting up to 6 months.
Evidence on Efficacy
Schnebel and Simmons [123] found no statistically significant difference between oral colchicine and a placebo, although the oral colchicine group did have significantly more diarrhea and vomiting than the placebo group. Simmons, Harris, Koulisis, et al., [124] who compared groups receiving either intravenous colchicine or intravenous saline, found significantly improved pain ratings for the colchicine group, but pain relief was short-lived (lasting from 1 hour to 2 days). Also, two patients in the colchicine group developed complications (diarrhea and a local inflammatory response). Meek, Giudice, McFadden, et al., [122] who evaluated for 1 month a group receiving one dose of intravenous colchicine followed by oral colchicine, compared with a group receiving placebo, found significantly greater pain relief in the colchicine group.
Potential Harms and Costs
Potential complications from the use of colchicine are gastrointestinal irritation, skin problems, severe chemical cellulitis from intravenous infiltration, and bone marrow suppression with agranulocytosis. [124] The expense of treatment with colchicine varies greatly, depending on whether oral or intravenous administration is used and on length of treatment.
Summary of Findings.
Research evidence is limited and conflicting on whether colchicine, given either orally or intravenously, is an effective treatment for patients with acute low back problems. Serious potential side effects have been reported with use of this medication.
Antidepressant Medications
Panel findings and recommendations:
Antidepressant medications have been widely used for both depressed and nondepressed patients with chronic low back problems. The extent to which these medications are used in treating patients with acute low back problems is unknown. Some researchers have hypothesized that the medications may possibly have a pain-relieving effect in addition to antidepressant properties. If so, the medications could help some patients who have chronic pain whether or not the patients are also depressed. The therapeutic objective of using antidepressant medications for low back problems is to reduce pain.
Literature Reviewed
Of 18 articles screened, 3 RCTs met review criteria. [125]- [127] Other articles also contained information used by the panel. [128], [129]
Evidence on Efficacy.
No studies were found evaluating the efficacy of antidepressant medications for treatment of acute low back problems. The three studies reviewed all compared an antidepressant medication to a placebo in a double-blind fashion in patients with chronic, not acute, low back pain. These studies all randomized patients to receive either a pharmacologically inert placebo or an antidepressant medication. Alcoff, Jones, Rust, et al. [125] used imipramine, as did Jenkins, Ebbutt, and Evans. [127] Goodkin, Gullion, and Agras [126] used trazodone. The studies found no significant differences between groups receiving antidepressant and placebo in terms of pain reduction, functional limitations, depression, or the use of opioids. All three studies had methodological flaws, including small sample sizes, lack of power calculations, and incomplete description of follow-up.
Potential Harms and Costs
Antidepressant medications can produce a variety of side effects including dry mouth, drowsiness, constipation, urinary retention, orthostatic hypotension, and mania. [128], [129]
The cost of treatment with antidepressant medications can vary from low to high depending on the medication used, dose, and length of treatment.
Summary of Findings.
No studies were found that evaluated the efficacy of antidepressant medications for treatment of acute low back problems. The studies reviewed all evaluated patients with chronic low back problems. They found no significant differences between antidepressants and placebo on any outcome measured. Numerous reported side effects are associated with antidepressant medications, but the potential for serious side effects is small in otherwise healthy adults.
Symptom Control: Physical Treatments
Spinal Manipulation
Panel findings and recommendations:
Spinal manipulation includes many different techniques. For this guideline, manipulation is defined as manual therapy in which loads are applied to the spine using short or long lever methods. The selected joint is moved to its end range of voluntary motion, followed by application of an impulse loading. The therapeutic objectives of manipulation include symptomatic relief and functional improvement.
Literature Reviewed
Of the 112 articles screened for this topic, 13 reporting on 12 RCTs met criteria for review. [72], [85], [130] - [140]
The panel also considered recent meta-analyses and cost analyses. [141]- [144] In addition, the panel used information from articles that did not meet selection criteria. [145]- [149]
Evidence on Efficacy
The meta-analysis by Shekelle, Adams, Chassin, et al. [144] was based on 29 controlled trials of manipulation for low back problems. Nine of the studies used in the meta-analysis focused on patients with acute low back problems and tested the effect of manipulation against sham manipulation [136] or various other conservative treatments. [72], [132], [135], [137], [138], [140], [145], [149]
Of those RCTs that evaluated manipulation in patients with acute low back pain, the two highest quality studies used similar research designs. [136], [137] Both these studies randomly assigned patients to either a group receiving manipulation or a nontreatment control group, with patients stratified by whether symptoms had lasted less than 14 days, 14 to 28 days, or over 28 days in one study. [137] For patients with 14 to 28 days of symptoms, both studies found the manipulation groups had statistically significant improvement in pain relief and functioning compared with the control groups. However, this effect was only seen within the first 2 weeks after starting treatment. For patients with symptoms of less than 14 days or over 28 days, no differences in improvement were found between the manipulation and control groups for any follow-up times.
A meta-analysis of the remaining seven studies also showed statistically significant short-term effects of manipulation in hastening recovery from low back problems. [144] Another meta-analysis, based on 23 randomized controlled trials of manipulation or mobilization, came to a similar conclusion.[sup141 This analysis indicated that, in patients with acute low back problems without radiculopathy, manipulation reduces pain and has positive short-term impact on daily functioning. Most studies have concentrated upon outcomes assessed within the first month of care.
The meta-analysis by Shekelle, Adams, Chassin, et al. [144] analyzed, in addition, studies of spinal manipulation in patient groups who had predominantly chronic low back problems, a mix of acute and chronic low back problems, or pain of undetermined duration. Studies of manipulation in these groups had conflicting results concerning the efficacy of manipulation.
Shekelle, Adams, Chassin, et al. [144] also analyzed three studies on the use of spinal manipulation for patients with low back problems who had radiculopathy, but concluded that the evidence was insufficient to demonstrate efficacy. [131], [146], [148]
Potential Harms and Costs.
Shekelle, Adams, Chassin, et al. [144] described published case reports of patients presenting with sciatica who had increasing neurologic deterioration following manipulation, but estimated that the risk of serious complications from lumbar spinal manipulation is small and may vary with the clinical condition with which the patient presents. No systematic report of frequency of complications from spinal manipulative therapy has been published. Mandell, Lipton, Bernstein, et al. [147] listed autonomic disturbances such as faintness, perspiration, and hyperventilation as common short- term reactions to manipulation. The total cost of manipulative therapy is determined by the frequency and duration of care.
Summary of Findings
The evidence for effectiveness of manipulation varies depending on the duration and nature of the patient's presenting symptoms. For patients with acute low back symptoms without radiculopathy, the scientific evidence suggests spinal manipulation is effective in reducing pain and perhaps speeding recovery within the first month of symptoms. For patients whose low back problems persist beyond 1 month, the scientific evidence on effectiveness of manipulation was found to be inconclusive. For patients with radiculopathy, the scientific evidence was also inconclusive about either the effectiveness or the potential harms of manipulation. Finally, the panel offered the opinion that, for patients with acute low back problems and findings of possible progressive or severe neurologic deficits, assessment to rule out serious neurologic conditions is indicated before initiating manipulation therapy.
Physical Agents and Modalities
Panel findings and recommendations:
Physical agents and modalities include ice, heat (including diathermy), massage, ultrasound, cutaneous laser treatment, and electrical stimulation (not transcutaneous electrical nerve stimulation or TENS). The therapeutic objective of physical agents and modalities is to provide symptomatic relief and, for some modalities, to reduce inflammation, "muscular symptoms," or joint stiffness.
Literature Reviewed
Of 25 articles screened for this topic, 10 reporting on 8 RCTs met criteria for review.
Evidence on Efficacy
Many studies compared different combinations of physical agents and modalities, making it difficult to evaluate effectiveness of specific modalities. Only two studies evaluated physical agents and modalities in patients with acute low back pain. [85], [140] Neither found significant differences in self-rated pain relief or other outcome measures between patient groups receiving physical agents and modalities (including diathermy, ultrasound, flexion/extension exercises, massage, and electrotherapy) and groups receiving a placebo.
The other studies reported on groups of either chronic or a mix of acute and chronic low back pain patients. Three studies found no significant differences in patient-reported outcome measures between treatments (including cutaneous laser, diathermy, electrotherapy, exercise, heat, massage, and ultrasound) and a placebo. Manniche, Hesselsoe, Bentzen, et al. [155] found intensive back-strengthening exercises superior to physical agents and modalities on patient-rated outcome measures, but the group receiving physical agents/modality treatment was not compared with a control group receiving no intervention. Melzack, Vetere, and Finch [156] found that a group receiving TENS therapy had greater pain relief than a group receiving massage therapy. Again, treatments were not compared with a no-intervention control. Linton, Bradley, Jensen, et al. [154] found that a group given a combination of physical agents and modalities, ergonomic education, and behavioral therapy had significantly better outcomes than a control group receiving no intervention, but the effect of physical agents and modalities could not be determined.
Potential Harms and Costs
Risks from potential complications of physical agents and modalities are believed to be small. A possible exception is in pregnant patients, for whom ultrasound and diathermy are not recommended because of theoretical risks to the fetus.
The costs of individual treatment sessions using physical agents and modalities are variable, determined by the number of modalities used, the length of treatment, and the number of treatment visits.
Summary of Findings
No well-designed controlled trials support the use of physical agents and modalities as treatments for acute low back problems. However, some patients with acute low back problems appear to have temporary symptomatic relief with physical agents and modalities. Therefore, self-administered home programs for modalities involving heat or cold are considered a treatment option.
Transcutaneous Electrical Nerve Stimulation
Panel findings and recommendations:
A TENS unit is a small battery-operated device worn by the patient. It provides continuous pulses of electricity by way of surface electrodes. Presumably, TENS produces a counter-stimulation of the nervous system, which can modify pain perception. The therapeutic objective of TENS in patients with low back problems is to provide symptomatic pain relief.
Literature Reviewed
Of 34 articles screened for this topic, 9 articles reporting on 8 RCTs met criteria for review. [156]- [164] Only one study evaluated patients with acute low back pain. [160]
Evidence on Efficacy
Hackett, Seddon, and Kaminski [160] evaluated a treatment called "electroacupuncture," which consisted of low-amplitude pulsed electrical current administered by way of surface electrodes rather than by needles. The panel considered this a variation of TENS rather than a type of acupuncture since no needling was involved. For the study, 37 patients with low back pain of less than 3 days' duration were randomly assigned to groups receiving either two 15-minute treatments of electroacupuncture and placebo tablets or paracetamol tablets and placebo electroacupuncture with no current applied. There was no difference in results at 1 and 2 weeks. By the sixth week after the initial treatment, patients who had electroacupuncture reported significantly less pain, measured on a visual analog pain-rating scale, compared with those who took paracetamol.
The other studies reviewed focused on patients with chronic low back pain or other types of chronic pain or on a mixture of acute and chronic low back pain patients. The largest randomized study of TENS was carefully blinded and found no benefit for TENS over sham TENS in patients with chronic low back problems. [157] The remaining studies were of variable quality and were inconclusive regarding efficacy of TENS for relieving chronic pain.
Potential Harms and Costs
The risks of TENS are considered low. The cost of this treatment is considered low to moderate (depending upon whether the equipment is rented or owned by the patient).
Summary of Findings
There is inconclusive evidence of the efficacy of TENS in patients with acute low back problems. Only one published study addresses this issue, and its findings are considered weak.
Shoe Insoles and Shoe Lifts
Panel findings and recommendations:
Shoe insoles (or inserts) are devices placed inside shoes that may vary from over-the-counter foam or rubber inserts to custom-made orthotics. The therapeutic objective of shoe inserts is the reduction of back pain.
Shoe lifts (or raises) are additions made to the heel or sole of a shoe to increase its height. The therapeutic objective of shoe lifts is to compensate for lower limb length inequality and thereby reduce back pain.
Literature Reviewed
Of seven articles reviewed for this topic, only one was an RCT that met criteria for review. [165] Other articles contained information used by the panel, but did not meet article selection criteria. [166]- [168]
Evidence on Efficacy
Basford and Smith [165] used a randomized crossover design to evaluate the use of shoe insoles compared with no insoles in adults with mild back pain who spent at least 75 percent of each workday standing. Of 39 subjects studied, 44 percent reported reduced back pain when using the insoles, 3 percent reported increased back pain, and 51 percent reported no difference. Of the subjects who reported no improvement, many stated that their shoes were too tight to allow insoles to be added comfortably.
There were no controlled trials that evaluated shoe lifts in patients with either acute or chronic low back problems. The extent to which leg length inequality might be associated with low back problems has not been established. Lower limb length differences of up to 2 cm are frequently seen in subjects with no history of low back problems. [167], [168] One study evaluated aircraft industry workers and found no correlation between a 2-cm limb length inequality and either previous back problems or later reports of back complaints. [166]
Potential Harms and Costs.
Shoe insoles and shoe lifts are low-risk treatments; their cost varies from low (for ready-made items) to moderate (for custom-made orthotics).
Summary of Findings
Limited evidence (one crossover study) indicates that shoe insoles may reduce back pain in some individuals with mild back complaints. There is no evidence they provide any long-term benefit. The extent to which leg length inequality might be associated with acute low back problems has not been established, although differences of less than 2 cm are unlikely to be problematic.
Lumbar Corsets and Back Belts
Panel findings and recommendations:
Lumbar support devices for low back problems include lumbar corsets and support belts, back braces and molded jackets, and back rests for chairs and car seats. The panel decided to evaluate only lumbar corsets and support belts for this guideline. Among theories on why lumbar corsets and support belts might help treat or prevent low back problems are that they compress the abdomen (causing increased intra-abdominal pressure, which unloads the vertebral column) and/or that they act as a mechanical reminder to decrease bending. Therapeutic objectives of lumbar supports are to control pain and/or protect against injury.
Literature Reviewed
Of 31 articles screened, 3 RCTs about lumbar corsets and support belts met review criteria for adequate evidence about efficacy. [131], [169], [170] Another article contained information used by the panel, but did not meet selection criteria. [171] None of these studies evaluated only patients with acute low back problems. One evaluated only chronic low back pain patients. [171] One evaluated a mixed group of acute and chronic low back pain patients. [131] The other two studies evaluated the prevention of low back problems in workers doing frequent lifting tasks. [169], [170]
Evidence on Efficacy
Coxhead, Meade, Inskip, et al. [131] compared lumbar corset use to traction, exercise, and manipulation but included other interventions, making the direct effect of corset use difficult to determine.
Million, Haavik Nilsen, Jayson, et al. [171] compared the use of two types of lumbar corsets, one with and one without a lumbar support, in patients with chronic low back problems (all with symptoms longer than 6 months). This study was an RCT, but had too few subjects to meet review criteria. Although this study found a considerable and significant improvement in symptoms in the group wearing corsets with a lumbar support, no control group was used in the study to ascertain the effect of corset use as compared with no corset use.
Walsh and Schwartz, [170] in an RCT, evaluated 90 grocery warehouse workers not currently receiving treatment for low back problems. Subjects were randomly assigned to three groups. One group received a custom-molded lumbar corset plus a 1-hour training program on proper lifting, one the training program alone, and one no intervention. During the 6-month study period, no significant differences were reported between groups in back injury rates or in time lost from work due to back problems. However, the group assigned to lumbar corsets plus training showed significantly less time loss from work due to back symptoms during the 6 months of the study when compared with the prior 6-month period. No similar significant effect was found for the other two groups.
Reddell, Congleton, Huchingson, et al., [169] in an RCT, evaluated 642 airline baggage handlers randomly assigned to use of a lumbar weightlifting belt, with and without a supplemental training class, or to the training class alone, or to no intervention. The 1-hour training course included instruction on proper lifting techniques, and employees were given stretching exercises to be done before each flight. Over an 8-month period, no significant differences were found between groups studied in back injury claims or in days lost from work. However, the validity of these results is questionable since 58 percent of workers assigned to wear weightlifting belts stopped using them before the end of the study period.
Potential Harms and Costs
Some authors suggest that the prolonged use of lumbar corsets and support belts may lead to a decrease in strength of abdominal and back muscles, but no clear evidence of this was found in patients with low back problems. Walsh and Schwartz [170] found that no such weakness occurred in workers who wore lumbar corsets for 6 months as a preventive measure. In the study by Reddell, Congleton, Huchingson, et al., [169] the majority of workers who stopped wearing weightlifting belts complained that the belts were too hot and/or too uncomfortable.
The cost of lumbar corsets and support belts varies from low to moderately expensive.
Summary of Findings
There is no evidence that lumbar corsets or support belts are effective for treating acute low back problems and conflicting evidence on whether lumbar corsets and support belts are effective for preventing or reducing the impact of low back problems in subjects who do frequent lifting at work.
Traction
Panel findings and recommendations:
Traction, when used for low back problems, involves the application of intermittent or continuous force along the axis of the spine in an attempt to elongate the spine by either mechanical or manual means. The most common type used for low back pain is pelvic traction, in which a snug girdle around the pelvis is attached to weights hung at the foot of the bed. The therapeutic objective of traction for patients with low back problems is to reduce pain.
Literature Reviewed
Of 31 articles screened for this topic, 7 articles reporting on 6 RCTs met criteria for review. Another article contained information used by the panel, but did not meet selection criteria.
Evidence on Efficacy
A meta-analysis of the studies on traction was done by the panel methodologists. Quality rating was done for the six RCTs reviewed without knowledge of study results. There were no excellent studies, one good study, three fair studies, a fair study reported on by Mathews, Mills, Jenkins, and one poor study.
All the studies involved patients with acute low back pain of less than 3 months' duration, but studies varied on whether patients with a history of previous low back problems were excluded. Groups receiving traction were compared with groups receiving sham traction. [173], [174] Traction combined with bed rest and corset use was compared with bed rest and corset use alone. [172] Traction was compared with heat [138] and with isometric exercise. [175] In addition, Coxhead, Meade, Inskip, et al. [131] studied groups receiving various combinations of traction, manipulation, exercise, and corset use in a multifactorial design with 16 cells. The six studies varied with respect to types of traction, control groups, outcome measures, and assessment periods. For this reason, no attempt was made to quantitatively combine these data.
Five of the six studies showed no difference between traction and the comparison group. In one study, the group treated with bed rest and corset use combined with traction had less pain at 1 week than those receiving bed rest and corset use without traction, but this difference was gone by 3 weeks. [172] Moreover, some criticize this study because of attention bias against those in the control group. In general, the studies did not indicate that traction in any form is beneficial in terms of pain relief, physiological status, length of hospital stay, functional outcome, or perception of overall improvement for patients with acute low back problems. The studies were too small to determine if traction actually harms patients with acute low back problems.
Potential Harms and Costs
The potential harms from traction relate to debilitation due to prolonged bed rest, including loss of muscle tone, bone demineralization, and the risk of thrombophlebitis. There is added risk of increased intraocular pressure and blood pressure with inverted hanging traction. [176] The cost of traction is considered low to moderate if it is done on an outpatient basis, or high if the patient is hospitalized for traction.
Summary of Findings
Evidence does not demonstrate traction to be effective in the treatment of patients with acute low back problems.
Biofeedback
Panel findings and recommendations:
Biofeedback involves translating the physiologic activity of a patient's muscular response into a visual or auditory signal that allows the patient to try to facilitate or inhibit the muscular activity. The therapeutic objective is to reduce muscle tension and thereby reduce pain. Biofeedback has been advocated primarily for patients with chronic low back problems.
Literature Reviewed
Of 13 articles screened for this topic, 4 reporting on 5 RCTs met criteria for review. [177]- [180] Other studies did not meet panel review criteria because they had fewer than 10 subjects per treatment group, but were used in a meta-analysis. [181], [182] All of the studies involved patients with chronic low back pain. In most subjects, pain had persisted for several years.
Evidence on Efficacy
Because these trials presented conflicting results, a meta-analysis was begun by the panel methodologists. Studies were assessed for quality without knowledge of the results. There were no excellent studies, one good study, [178] three fair studies, [177], [180], [182] and a fair study reported by Flor, Haag, Turk, et al. [179] and by Flor, Haag, and Turk. [181] There were no poor studies.
The studies involved comparisons of biofeedback with sham biofeedback; [178], [179], [181] biofeedback combined with another treatment in comparison with the other treatment alone; [177] and biofeedback alone compared with some other treatment. [179], [181], [182]
The study with a good quality rating showed no benefit for biofeedback over sham biofeedback. [178] Two studies reported patients in the biofeedback groups developed significantly better control of paraspinous muscle electromyographic activity. [178], [180] In neither study did this reduce pain. Thus, of the five studies, two showed no benefit for biofeedback. [178], [180] Two showed a benefit for biofeedback: Asfour, Khalil, Waly, et al. [177] and the study reported by Flor, Haag, Turk, et al., [179] and by Flor, Haag, and Turk. [181] One study showed a slight benefit for biofeedback compared with a placebo condition, but reported an even better benefit for relaxation training. [182] Statistical combination of results from these studies was not done because it would require requesting the original data from the authors.
Conclusions from the attempted meta-analysis were that biofeedback as a treatment for low back problems has been studied only for chronic problems, and that most of the studies are of mediocre quality and arrive at conflicting results.
Potential Harms and Costs
The risks for biofeedback are considered low. The costs of biofeedback treatment are determined by the number of treatment visits.
Summary of Findings
There is conflicting evidence on the effectiveness of biofeedback for treating patients with chronic low back problems. However, this technique has not been studied in patients with acute low back problems.
Symptom Control: Injection Therapy
Trigger Point and Ligamentous Injections
Panel findings and recommendations:
Trigger point injections involve the injection of local anesthetic into soft tissues (muscles) near localized tender points in the paravertebral area. [189] The theory that such trigger points are responsible for causing or perpetuating low back pain is controversial and disputed by many experts. Other articles reviewed for this topic involve the injection of various substances (especially sclerosing agents) into interspinal ligaments and ligamentous muscle attachments in the low back. The theory behind such treatment is that this stimulates formation of scar tissue in ligaments. The therapeutic objective of both trigger point injections and ligamentous injections is to reduce low back pain.
Literature Reviewed
Of 14 articles screened for the topics of trigger point and ligamentous injections, 6 RCTs met criteria for review. Three of these evaluated trigger point injections into muscle. [183]- [185] Three evaluated injections into ligamentous structures in the back. [186]- [188] Other articles contained information used by the panel, but did not meet article selection criteria. [189]- [190]
Evidence on Efficacy
Of the articles evaluating trigger point injections, only Frost, Jessen, and Siggaard-Andersen [184] evaluated patients with acute low back problems. The study population, however, included patients with acute neck or shoulder pain, and data were not given separately for the patients with low back problems. For the other two RCTs on trigger point injections, either the patients evaluated had chronic low back problems [183] or the duration of symptoms was not reported. [185]
Various medications were used for trigger point injections. Frost, Jessen, and Siggaard-Andersen [184] had two groups receiving either local anesthetic or saline. Bourne [183] had three groups receiving methylprednisolone and lignocaine, or triamcinolone and lignocaine, or lignocaine alone. Garvey, Marks, and Wiesel [185] had four groups receiving lidocaine alone, or lidocaine combined with a steroid, or needle acupuncture (with no injection of material), or vapocoolant spray to the skin followed by acupressure (using a plastic needle guard). Two studies included control groups who had no medication injected into muscles, [184], [185] but none of the three studies included a group with no intervention.
Frost, Jessen, and Siggaard-Andersen [184] and Garvey, Marks, and Wiesel [185] found no differences between groups in pain relief or other outcome measures on follow-up at 1 and 2 weeks posttreatment, respectively. Bourne[183] found significantly greater pain relief at 3 months follow-up for the two groups receiving steroid injections than for the group receiving injections of local anesthetic alone.
Of the three articles evaluating injections into ligamentous structures, two studies evaluated patient groups including some patients with acute low back problems. [186], [188] One study evaluated a subgroup of patients with acute low back problems, all with pain over the medial iliac crest. [186] In the other study, patients were only described as having low back problems for greater than 1 month's duration without specifying how many patients had either acute or chronic symptoms. [188] The third article evaluating ligamentous injections evaluated only patients with chronic low back problems. [187]
Various substances were injected into different ligamentous structures of the low back. Collée, Dijkmans, Vandenbroucke, et al. [186] studied groups receiving injections of either local anesthetic or saline into an area of tenderness over the medial iliac crest (not specified if into muscle or ligamentous attachments). Ongley, Klein, Dorman, et al. [187] evaluated groups receiving injections of either a dilute phenol solution (sclerosing agent) or saline into the lumbar interspinal ligament. Sonne, Christensen, Hansen, et al. [188] evaluated groups receiving injections of either a combination of local anesthetic and steroid or saline alone into the iliolumbar ligament.
Collée, Dijkmans, Vandenbroucke, et al. [186] found that for patients with acute low back pain, there was no significant difference in pain relief between the saline or anesthetic groups, either immediately postinjection or at 1 or 2 weeks follow-up. Ongley, Klein, Dorman, et al. [187] found greater improvement in pain and disability scores for the patients receiving phenol injections (intended to induce scar) as compared with saline. Sonne, Christensen, Hansen, et al. [188] found that the group receiving injections with a combination of steroid and local anesthetic had significantly greater improvement in symptoms at 2 weeks follow-up than did the group receiving injections with saline.
Potential Harms and Costs
The potential risks of trigger point injections include damage to nerves or other tissues, infection, and hemorrhage. [190] The cost for this treatment is considered low to moderate.
Summary of Findings
Based on limited research evidence in studies that included patients with chronic problems, the efficacy of trigger point or ligamentous injections for treating acute low back problems appears equivocal. The injections can expose patients to serious potential complications.
Facet Joint Injections
Panel findings and recommendations:
In treatment of low back problems, facet joint injections involve the injection of local anesthetics and/or corticosteroids into or around facet joints of the lumbar spine, with needle placement aided by fluoroscopy. The theoretical basis is that some patients with low back problems have a "facet syndrome" with pain arising from facet joints. The facet syndrome reportedly involves patients with primarily low back pain (unilateral or bilateral) and no root tension signs or neurologic deficits, the pain usually being aggravated by extension of the spine. [191] The therapeutic objective of facet joint injections is temporary relief from motion-limiting pain so the patient may proceed into an appropriate exercise program. [198]
Literature Reviewed
Of 17 articles screened for this topic, 5 RCTs met review criteria. [191]- [195] Other articles contained information used by the panel, but did not meet criteria. [196], [197]
Evidence on Efficacy
No articles were found evaluating patient groups who had only acute low back problems of less than 3 months' duration. One study evaluated a mixed group of acute and chronic patients with pretreatment symptom durations ranging from 1 to 12 months. [191] Three articles evaluated patients with low back pain of over 3 months' duration. [192] - [194] One study did not specify symptom duration before treatment. [195]
Injections were made either into facet joints or into pericapsular areas around facet joints. The latter type of injection was also referred to as a "facet nerve block" when a local anesthetic was used. Medications injected included steroids, local anesthetics, and saline (either alone or in combination).
Three studies evaluated a combination of steroid and local anesthetic injected into either facet joints or pericapsular areas. [193]- [195] Three studies evaluated groups receiving facet joint injections in which steroid was compared with saline, [192] or local anesthetic was compared with saline, [191] or a combination of steroid and local anesthetic was compared with saline. [193]
None of the five studies that met review criteria found any significant differences between groups for patient-rated pain relief or global improvement scores during follow-up periods of up to 3 months after treatment. The only study with follow-up beyond 3 months found significantly greater improvement in pain and functional disability ratings at 6 months follow-up for the group receiving steroid facet injections compared with saline facet injections, but no significant differences between groups in number of patients who had sustained improvement over the entire 6-month follow-up period. [192]
Potential Harms and Costs
Some of the articles reviewed noted transient local pain at the injection sites. The risks of facet joint injections include potential infection, hemorrhage, neurologic damage, and chemical meningitis, [196], [197] as well as x-ray exposure from fluoroscopy. Facet injections are considered a moderate- to high-cost treatment.
Summary of Findings
No studies have adequately investigated the efficacy of facet injections for patients with acute low back problems. However, there were an adequate number of studies evaluating facet injections for chronic low back problems. [192]- [195] One study evaluated a mix of acute and chronic problems. [191] Neither the type of agent injected (steroid, local anesthetic, saline, or a combination of these) nor the location of the injection (intrafacet or pericapsular) made a significant difference in patient outcomes during the first 3 months after treatment or in the percentage of patients with sustained improvement over 6 months.
Based on limited research evidence, facet joint injections appear to be associated with rare potential serious complications and do not appear to be effective for treating acute low back problems.
Epidural Injections (Steroids, Lidocaine, Opioids)
Panel findings and recommendations:
Epidural injections for treating low back problems, done primarily in patients with suspected radiculopathy, involve the injection of medication (corticosteroids, local anesthetics, or narcotics) into the epidural space, near the site where the nerve roots pass before entering the intervertebral foramen. In theory, injecting medication into the epidural space allows a concentrated amount of medication to be deposited and retained in a specific area, exposing the nerves to the medication for a prolonged period of time. The therapeutic objective of epidural injections is to reduce swelling, inflammation, and pain.
There are various techniques for performing the epidural injection, some of which are more precise than others. [198] According to White, [199] placement of epidural needles is incorrect in 25 percent of the cases.
Literature Reviewed
Of 74 articles screened for this topic, 9 RCTs met criteria for review. [138], [200] - [207] Other articles contained information used by the panel, but did not meet article selection criteria. [147], [198], [199], [208], [209]
Evidence on Efficacy
Two studies evaluated patients with acute low back pain of less than 3 months' duration and also with radicular symptoms and findings suggesting nerve root dysfunction. [138], [202] Both studies compared groups receiving epidural injections of steroids combined with local anesthetic to groups receiving injections of local anesthetic alone, either into the epidural space [202] or into a tender spot over the sacrum. [138]
Cuckler, Bernini, Wiesel, et al. [202] found no significant differences in pain relief between groups immediately posttreatment or at long-term follow-up (mean of 20 months). Mathews, Mills, Jenkins, et al. [138] found no significant differences in pain relief between groups at 1, 6, or 12 months follow-up, but the epidural steroid group did have significantly better results at 3 months follow-up.
The remaining seven studies evaluated groups with either chronic low back problems or a mix of acute and chronic problems. [200], [201], [203] - [207] Medications used and locations injected varied. Four studies evaluated groups receiving epidural injections with various combinations of steroids, local anesthetics, and/or saline. [200], [201], [205], [207] Two studies evaluated groups receiving either epidural steroid injections or injections of saline into the interspinous ligament. [204], [206] One study evaluated groups receiving epidural injections with various combinations of steroids and morphine. [203]
The five studies that reported on short-term pain relief at 2 to 4 weeks follow-up showed conflicting results. For this time period, three studies reported significantly greater pain relief for the epidural steroid groups. [201], [204], [206] The other two studies found no differences in pain relief between groups. [205], [207]
Five studies reported on follow-up beyond 1 month. [200], [201], [204], [205], [207] Only one found significantly greater pain relief for the epidural steroid group. [200] The other studies found no significant differences in pain relief between groups. One study did find that a significantly higher percentage of the group receiving epidural steroid injections had returned to work at 3 months. [204] Three studies showed significantly better results within the first month for epidural steroids versus local anesthetic or saline injections, but not on longer follow-up. [201], [204], [206] No significant differences were reported between groups at 3 months [204] or at 1 year. [201] Ridley, Kingsley, Gibson, et al. [206] did not report follow-up beyond 2 weeks. Two other studies found no significant differences in pain relief between groups for any follow-up period. [205], [207] One study that evaluated epidural injections of morphine compared with (and/or in combination with) steroids found no significant differences in pain relief between groups on either short-term (within 1 month) or longer term follow-up. [203]
Potential Harms and Costs
Reported complications of epidural injections are described by Kepes and Duncalf. [208] The primary major complication reported was rare epidural abscess. Minor transient complications included headache, fever, and inadvertent spinal tap. Rocco, Frank, Kaul, et al. [209] reported several cases of life-threatening ventilatory depression in patients who received epidural injections of morphine and steroids combined. In 5 of the 19 times such injections were given, the patients experienced respiratory depression to the point of somnolence and had to receive naloxone for reversal of narcosis. Also posttreatment, the respiratory rates of patients receiving epidural morphine were lower than for patients receiving epidural steroids alone. The lowest respiratory rates were seen in those receiving injections of morphine combined with steroids. Mandell, Lipton, Bernstein, et al. [147] described headache as the most common side effect of epidural steroid injections (presumably resulting from pressure changes in the epidural space or accidental puncture of the dura) and listed aseptic meningitis, infection, and neurologic problems as other possible complications. Epidural injections are considered an expensive treatment.
Summary of Findings
Limited research evidence indicates that epidural injections using any type of medication lack proven efficacy for treating patients with acute low back pain without radiculopathy. Epidural injections are invasive and pose rare but serious potential risks. There was no evidence that epidural steroids are effective in treating acute radiculopathy, but the panel's opinion was that epidural steroid injections may be useful as an attempt to avoid surgery.
Acupuncture
Panel findings and recommendations:
Acupuncture is defined here to include all types of "dry needling" procedures (where no medication is injected) into cutaneous and subcutaneous tissues, muscles, or ligaments. Traditional acupuncture, based on Chinese philosophy, requires that needles be inserted into specific areas of the body (the prescribed Chinese meridians) and that these needles be rotated to produce a noxious stimulus. Other types of dry needling involve needle insertion without regard for the Chinese meridians into tender spots or other areas and may or may not involve the rotation of the needles. Some dry needling techniques also add electrical stimulation to the needles. The therapeutic objective of acupuncture and other dry needling techniques is to reduce pain.
Literature Reviewed
Of 24 articles screened for this topic, 8 reporting on 6 RCTs met criteria for review. [161], [162], [210] - [215] The panel also examined a meta-analysis. [216] Other articles contained information used by the panel, but did not meet article selection criteria. [217]- [220]
Evidence on Efficacy
All six RCTs evaluated patients with chronic back problems (with or without leg symptoms) of greater than 6 months' duration. Four of the articles reporting on three RCTs compared groups that received needling with groups that received no needling. [161], [162], [210], [213] Needling received was either acupuncture in traditional Chinese meridians [161], [162], [210] or needle insertion into tender muscle points. [213] In these studies, the groups that received some type of needling intervention had significantly better outcomes (in pain reduction and increased activity levels) than did the groups receiving no needling.
The remaining four articles reporting on three RCTs compared groups receiving acupuncture in the traditional Chinese meridians to groups receiving various types of needle insertion in other parts of the back. [211]- [215] None of these studies found any significant differences between groups in any outcomes measured.
A meta-analysis, based on 51 clinical studies on acupuncture used for various types of chronic pain (including back pain), found that the quality of even the better studies was mediocre and their results highly contradictory. [216] Specifically noted was that most of these studies did not provide an appropriate control group or were not adequately blinded. None of the studies demonstrated an advantage of needling in the appropriate Chinese meridians over misplaced needling. In this meta-analysis, the authors concluded that the efficacy of acupuncture for treatment of chronic pain remains doubtful.
Potential Harms and Costs
Reported complications of acupuncture include hematomas, infections (hepatitis B and Staphylococcus aureus), pneumothorax, and spinal nerve and spinal cord injuries due to buried needles migrating to the spinal cord. [217]- [220] In addition, the panel offered the opinion that needle insertion treatments involve some discomfort. Costs of acupuncture and other dry needling treatments vary depending on the number of treatment visits.
Summary of Findings.
No studies were found evaluating efficacy of acupuncture in patients with acute low back problems. In three of the six RCTs evaluating efficacy for chronic low back problems, outcomes were better for the acupuncture group than for nontreatment control groups. All studies had methodologic flaws. Acupuncture was also found to have risks of significant complications.
Activity Recommendations
Panel findings and recommendations:
Patients with acute low back problems may be more comfortable if they temporarily limit or avoid specific activities known to increase mechanical stress on the spine, especially prolonged unsupported sitting, heavy lifting, and bending or twisting the back while lifting. (Strength of Evidence = D.)
Activity recommendations for the employed patient with acute low back symptoms need to consider the patient's age and general health, and the physical demands of required job tasks. (Strength of Evidence = D.)
Patients with acute low back problems frequently seek advice from clinicians about the physical activities they can "safely" perform. Employed patients, or their employers, also often ask health care providers to recommend work restrictions that will allow the patient to remain on the job during an episode of acute low back symptoms. Activity modifications are aimed at allowing the patient with an acute low back problem to achieve a tolerable comfort level while continuing adequate physical activity to avoid debilitation. The overall goal is to aid recovery while disrupting daily activities as little as possible.
Literature Reviewed
Of the articles screened dealing with work and other activity modifications for patients with acute low back problems, none met established panel review criteria for adequate evidence about efficacy. However, eight articles were considered by the panel to contain useful information on these issues. [221]- [228]
Evidence on Efficacy
A number of epidemiological studies have looked at risk factors associated with developing acute low back problems. Although there is no clear consensus on the role of these factors, several studies have identified an increased incidence of low back problems among individuals whose work involves heavy or repetitive lifting, exposure to total body vibration (from vehicles or industrial machinery), asymmetric postures, and postures sustained for long periods of time. [222], [225]
Other biomechanical research suggests that certain postures and activities increase the mechanical stress on the spine. [221], [223], [225] It is not clear whether these mechanical stresses are the cause of low back problems. However, once symptoms are present, mechanical stresses correlate with worsening of symptoms. Prolonged sitting and postures that involve bending and twisting have been shown to increase the mechanical stress on the spine according to pressure measurements in lumbar intervertebral discs. Heavy lifting also appears to increase mechanical stress on the spine, but this stress can be reduced if the lifted object is held close to the body rather than at arm's length.
A lifting equation to calculate appropriate lifting limits for various tasks was part of a guideline developed in 1981 by the National Institute of Occupational Safety and Health [227] and revised more recently. [228] Unfortunately, the ability of the guideline to reduce the incidence of low back problems has yet to be directly validated. Other ergonomic guidelines for safe lifting have been reviewed by Dul and Hildebrandt. [224]
Summary of Findings
While scientific information is limited, the panel felt that activity modifications represented an important practical issue for the clinician. The panel's recommendations are based on their interpretation of the available scientific data. Patients with acute low back problems can be advised to limit temporarily any heavy lifting, prolonged sitting, and bending or twisting the back since these activities have been shown to increase mechanical stress on the spine.
In recommending activity modifications for patients who work, the clinician may find it helpful to obtain from the employer a description of the physical demands of required job tasks. The nature and duration of limitations will depend on the clinical status of the patient and the physical requirements of the job. Activity modifications must be time-limited, clear to both patient and employer, and reviewed by the clinician on a regular basis.
Several ergonomic guidelines on lifting and materials-handling tasks are available to help the clinician provide ranges of activity alterations at work. These guidelines are based on various biomechanical assumptions and theoretical equations to build a margin of safety for individuals who have to lift at work. It should be remembered that such guidelines were developed or otherwise healthy workers and are therefore of limited use in making strict recommendations. None of these guidelines has been adequately tested to see if adherence will reduce the occurrence of low back problems.
The panel recommends that clinicians help patients establish activity goals, in consultation with their employer when applicable. Such goals are particularly important for the small percentage of patients who are still not able to overcome activity intolerance after 1 to 2 months of symptoms. Since nonphysical factors, such as emotional distress or low work satisfaction, may also affect an individual's symptoms and response to treatment, activity goals can help keep attention focused on the expected return to full functional status and emphasize physical conditioning to improve activity tolerance.
Bed Rest
Panel findings and recommendations:
Bed rest is a frequently used treatment for acute low back pain. The therapeutic objective is to relieve symptoms by reducing intradiscal pressure and/or pressure on nerve roots. Studies have shown that intradiscal pressures are lowest when subjects are lying supine in the semi-Fowler position, on the back with hips and knees moderately flexed. [8]
Literature Reviewed.
Of 12 articles screened for this topic, 5 reporting on 4 RCTs met criteria for review. [75], [85], [117], [229], [230] All these studies evaluated patients with acute low back problems. Other articles contained information used by the panel, but did not meet selection criteria. [8], [231], [232]
Evidence on Efficacy
Evidence is limited regarding efficacy of bed rest versus no treatment for patients with acute low back problems. One study involving military recruits compared forced bed rest to an alternative treatment of forced ambulation. [117] Although the bed rest group returned to full activity sooner, methodological problems with this study made interpretation difficult. Outcome assessments were not blinded, and patients in the hospitalized group were deprived of their peer-group activities, possibly confounding results. Two articles compared groups receiving either a recommendation for bed rest (of at least 4 days duration) or some other treatment (such as exercise, education, or manipulation) but no bed rest recommendation. [75], [85], [230] These two articles found no statistically significant differences between bed rest and other treatment modalities. Bed rest of more than 4 days and the resulting deactivation were worse for patients than a gradual return to normal levels of activity. Deyo, Diehl, and Rosenthal [229] compared two groups receiving recommendations for either 2 days or 7 days of bed rest. No differences were found between the groups in pain relief or in time to resumption of normal activities, except for earlier return to work in the 2-day group for those employed at baseline.
One problem with these studies is that the actual amount of bed rest reported by the subjects often differed greatly from the amount recommended. Deyo, Diehl, and Rosenthal [229] found that 74 percent of the 99 subjects assigned to the 7-day bed rest group reported fewer than 7 days of actual bed rest. The study reported by Evans, Gilbert, Taylor, et al. [75] and Gilbert, Taylor, Hildebrand, et al. [230] found that subjects who did not receive a bed rest recommendation also reported trying bed rest, but the duration was less than for the group receiving the recommendation.
Potential Harms and Costs
Potential physical side effects from prolonged bed rest are many, including muscle atrophy (1.0 to 1.5 percent of muscle mass lost per day), cardiopulmonary deconditioning (15-percent loss in aerobic capacity in 10 days), bone mineral loss with hypercalcemia and hypercalciuria, and the risk of thromboembolism. [232] There are also social side effects, such as perception of severe illness and economic loss due to increased time lost from work. [231]
Summary of Findings.
There is no evidence to support the efficacy of bed rest compared with no treatment in patients with acute low back problems. Deactivation resulting from prolonged bed rest (more than 2 to 4 days) appears to be worse for patients than a gradual return to normal levels of activity.
Exercise
Panel recommendations and findings:
Various types of exercise programs have been advocated for patients with low back problems. The most commonly studied types focus on back flexion, back extension, generalized strengthening, endurance (aerobic conditioning), stretching, or some combination of these. Authors also reported exercises for low back problems as dynamic (isotonic) and static (isometric). Most of these exercises can be either taught to the patient for home use or performed under supervision in a clinical setting. Commonly reported therapeutic objectives of exercise programs for low back problems are improvements in endurance, muscle strength, and flexibility presumably leading to reduced symptoms, improved level of functioning, and fewer or less severe future back problems.
Literature Reviewed
Of 92 articles screened, 20 RCTs met criteria for review. [74], [75], [81] , [83], [84], [86], [131], [155], [157], [233] - [243]
Other articles contained information used by the panel, but did not meet article selection criteria. [221], [226], [232], [244] - [253]
Only six of the articles reviewed involved studies of exercise as a treatment for patients with acute low back problems. [75], [83], [86], [131], [234], [243]
Two other studies evaluated the efficacy of exercises for preventing or reducing the impact of low back problems in workers whose jobs involved frequent lifting. [236], [237] The remaining articles all evaluated exercise as a treatment for groups that contained only patients with chronic pain or a mix of patients with acute and chronic problems. These were given less weight by the panel as there were enough studies using patients with acute low back problems.
Evidence on Efficacy
Of the six articles evaluating patients with acute low back problems, only one was considered well designed. [83] Swedish auto workers who had been off work for 6 weeks due to low back problems were randomized to either a control group with no recommendations for exercise or an exercise group with a program of gradually increased aerobic and back-strengthening exercises. At 1-year follow-up, patients in the exercise group had lost significantly less time from work due to back pain and had achieved a significantly higher level of fitness compared with the control group.
The other five articles dealing with acute low back problems included interventions that made the effect of exercise difficult to determine. [75], [86], [131], [234], [243]
Stankovic and Johnell [86] compared McKenzie extension exercises to a 45-minute educational session and found that the exercise group stopped medication use earlier and reported more pain relief and fewer days off work. Evans, Gilbert, Taylor, et al. [75] found that patients who received a flexion exercise program plus a 30-minute educational program stopped using medication sooner than did patients in bed rest and control groups. However, no differences were found between groups in reported degree of pain relief or activities of daily living.
The other three of these five studies showed no significant differences in outcomes between the treatment groups. [131], [234], [243]
Davies, Gibson, and Tester [234] compared groups receiving short-term diathermy and either extension or flexion exercises. Zylbergold and Piper [243] compared flexion exercises to manual therapy in combination with home back care instructions. Coxhead, Meade, Inskip, et al. [131] compared groups receiving various combinations of exercise (not otherwise specified), traction, manipulation, and lumbar corset use in a multifactorial study with 16 cells.
In summary, the six studies, which evaluated exercise for treating acute low back problems, used different forms of flexion or extension exercises, different treatment or control groups, different outcome measures, and different assessment periods. For this reason, no attempt was made to quantitatively combine these data.
As noted previously, two studies evaluated exercise for preventing acute or recurrent episodes of low back problems. Gundewall, Liljeqvist, and Hansson, [236] in a RCT, evaluated 60 nursing personnel working at a geriatric hospital. Subjects were randomized to receive either no intervention or a supervised exercise program during work six times per month for 13 months (emphasizing isometric and dynamic exercises strengthening the back extensor muscles).
At the end of the study, the exercise group had a significantly lower incidence of new low back problem episodes when compared with the control group (4 percent compared with 38 percent), fewer days lost from work, fewer days with back pain complaints, and a lower average duration of low back pain complaints. Trunk extensor strength measured with a spring gauge was not different between groups at the start of the study, but at the end of the study average trunk strength was significantly greater in the exercise group compared with the control group. The authors noted that the exercise group did receive more attention than the control group, which could account for some of the positive effect. Results were not reported separately for those with and without prior low back problems.
In the second study, Kellett, Kellett, and Nordholm, [237] in a RCT, evaluated 60 workers at a kitchen cabinet manufacturing company in Sweden. All were working at the start of the study and reported having either current or prior back pain. Subjects were randomly assigned to a control group or an exercise group. The exercise group was offered an exercise program at work once per week (30 minutes of aerobic movements of the arms, legs, and trunk followed by 10 minutes of relaxation) and were asked to do 30 minutes of aerobic exercise (such as walking, jogging, or cycling) on their own at least once per week.
Although subjects in the exercise group were encouraged to progressively increase their effort level during exercise, no direct measures of exertion (such as heart rate) were recorded. The exercise group was also given lectures about back problems and proper lifting techniques. There were no significant differences between exercise and control groups in incidence rates or days lost from work for episodes of back pain in the 1.5 years before the intervention. The incidence rate and days lost from work for episodes of back pain decreased in the exercise group during the subsequent 1.5-year intervention period. In the control group, absenteeism attributable to back pain increased during the intervention period. There were no significant differences, either before or after the study, between groups in cardiovascular fitness as measured by a suboptimal bicycle ergometer.
Deyo [232] remarked that, although there seems to be a consensus among experts that exercise plays a major role in the treatment of low back symptoms, most treatment programs prescribe a combination of exercises and there is little agreement on specific regimens. He also offered an opinion that additional benefits of aerobic exercise may include weight loss and favorable psychological effects, such as reduction of anxiety and depression. Other studies have shown that patients improve faster when given specific quotas of exercises to do rather than being told to stop exercise when it produces pain. [83], [246]
One study [251] found a back-specific exercise machine (the B- [200]) does not provide added benefit over traditional exercise in improving the objective back strength and flexibility (as measured by functional lifting capacity) of low back patients.
Potential Harms and Costs
Potential harms of exercise are usually not discussed. However, one RCT found that extension exercises caused increased symptoms in chronic low back pain patients. [238] Another study suggests that abdominal flexion (Williams flexion) exercises and stretching can increase mechanical stress on the spine as observed by intradiscal pressure measurements. [248]
Many methods have been proposed to evaluate mechanical stress on the back in different postures and activities. [221], [226], [244], [245], [247] - [250], [252] A biomechanical model by Schultz directly correlates with in vivo measurements of intradiscal pressure and myoelectric signals. [253] The measurements of relative stress on the spine during postures and activities generally relate to increased and decreased symptoms experienced by patients with back problems. Thus, this information can be used for recommendations about safety and altering activity. The costs of exercise programs can vary depending upon the setting. Those performed at home are inexpensive, whereas those done in supervised clinical settings are more costly. Exercise programs using back-specific computerized exercise machines can be very expensive. No studies meeting review criteria were found that provided evidence of any of these exercise settings being more effective than the others.
Summary of Findings
There are only a few RCTs that have evaluated exercise as a treatment for acute low back problems, and these are limited by small numbers of patients and inadequate descriptions of specific exercise regimens. The one well-designed RCT of patients limited for less than 3 months by low back symptoms found that a program of gradually increased aerobic and back-strengthening exercises was superior to doing no exercise at all.
Exercise programs aimed at improving general endurance (aerobic fitness) and muscular strength (especially of the back and abdomen) have been shown in some published studies to benefit patients with acute low back problems. No evidence supports stretching as effective treatment for acute low back problems. The panel offered the opinion that patients with acute low back problems would benefit from exercise programs if endurance programs are started early, using exercises that cause minimal mechanical stress on the back; if patients are given set exercise quotas gradually increased with time; and if later strengthening programs are individualized based on the level of activity to which patients wish to return. The panel suggested that the early goal of exercise programs is to prevent debilitation due to inactivity and then to improve activity tolerance to return patients to their highest level of functioning as soon as possible.
After the first month of symptoms, the vast majority of patients have recovered from activity limitations due to low back problems. However, if the patient is limited by back symptoms for more than 1 month, special diagnostic and treatment procedures are often considered to find a reason for the slow recovery (Attachment A3).
|
|
|
A3. Evaluation of the slow-to-recover patient limitations >4 weeks) |
The special studies are of two kinds. First are tests to provide evidence of physiologic dysfunction such as neurologic dysfunction, infection, inflammation, malignancy, or other systemic illness. Second are tests to define a potential anatomic reason for the dysfunction such as a herniated lumbar disc, spinal stenosis, infection, tumor, or abdominal mass. As a result of diagnostic considerations, therapeutic interventions including surgery may be recommended.
Except when serious underlying pathology is suspected, special diagnostic tests are usually not needed during the first month because it is not possible to predict early on which patients will and will not improve during this period. But those who are not improving at 1 month may include some who could benefit from specific therapeutic interventions. Waiting longer to start the diagnostic workup may delay recovery for these individuals.
Tests commonly used to identify focal neurologic physiologic dysfunction include electromyography (EMG), sensory evoked potentials (SEPs), and thermography. To detect physiologic dysfunction of nonneurologic diseases, general laboratory screening tests, such as erythrocyte sedimentation rate (ESR), complete blood count (CBC), and urinalysis (UA), and bone scan have been proposed.
Electrophysiologic Tests (EMG and SEP)
Panel findings and recommendations:
Electrophysiologic tests are sometimes used in patients with sciatica to evaluate physiologic functioning of the spinal cord, nerve roots, and peripheral nerves. Overall diagnostic objectives of these tests are to assess suspected myelopathy (dysfunction of the spinal cord), radiculopathy (dysfunction of a spinal nerve root), neuropathy (dysfunction of a peripheral nerve distal to the nerve root), and myopathy (muscle abnormalities). The tests and their specific diagnostic objectives for low back problems are as follows:
Literature Reviewed
Of 52 articles screened for this topic, 8 met review criteria for adequate evidence about efficacy. Also reviewed was one study that evaluated findings in asymptomatic subjects who had no history of low back problems. [261] Other studies contained information used by the panel.
Four studies evaluated needle EMG. Three studies evaluated H-reflex or F-wave tests. Two studies evaluated surface EMG. [258], [261] One study evaluated SEPs. [259] No studies were found evaluating nerve conduction for assessing low back problems. All articles meeting review criteria involved groups of patients either with chronic problems or with unreported symptom duration.
Evidence on Efficacy
Reference tests used to determine diagnostic accuracy (true positive and true negative rates) of needle EMG included surgical findings. [21], [254], [260] They also included clinical follow-up (pain rating and work status), with posttest at 1 year. The amount and quality of data that could be used to calculate diagnostic accuracy of these tests varied significantly between studies. Many studies had major methodological flaws such as biased test interpretations, faulty cohort assembly, and poor clinical descriptions. Determining the accuracy of EMG is difficult as well because anatomic defects seen at surgery, which are used in many of these studies as the reference standard for EMG, may or may not be the cause of symptoms. This makes true positive and true negative rate determinations of questionable value.
For needle EMG, four articles evaluated the test's accuracy in diagnosing nerve root problems. Aiello, Serra, Migliore, et al. evaluated 25 patients who had clinical evidence of L3 and/or L4 nerve root impairment. Needle EMG was abnormal in all 24 patients who had positive findings at surgery, but predicted the exact levels of nerve root pathology in only 9 percent of these 24 patients. One patient had a false-positive EMG with no disc herniation found at surgery.
Aiello, Serra, Tugnoli, et al. [254] evaluated the accuracy of EMG for detecting and localizing nerve root compromise in patients who had surgical findings of a single lumbar disc prolapse at the L3-L4 level (100-percent true positive rate, 88-percent true negative rate), with disc herniation at L4-L5 (96-percent true positive rate, 38-percent true negative rate) and with disc herniation L5-S1 (71-percent true positive rate, 79-percent true negative rate).
Khatri, Baruah, and McQuillen evaluated outcomes at 1 year in patients with radicular leg pain who had needle EMGs and computerized tomography (CT) scans and then went on to have disc surgery or nonsurgical treatment (including conservative care and/or epidural steroids). There were 35 patients who had abnormal EMGs and CT scan findings of a herniated lumbar disc. Of the 16 patients treated with surgery, 81 percent were better at 1 year, while of the 19 who had nonsurgical treatments only 47 percent reported improvement at one year. There were 24 patients whose EMGs and CT scans were both normal; none of these patients had surgery, and at 1-year follow-up 67 percent were improved.
Young, Getty, Jackson, et al. [260] evaluated 100 patients with clinical evidence of L5 or S1 radiculopathy and found that needle EMG correctly predicted the level of nerve root pathology in 84 percent of the 95 patients with positive surgical findings. The wrong level was predicted in seven patients, and in nine patients only one abnormal root was detected when two were involved. EMGs were negative in all five patients who had no root pathology noted at surgery.
In cases of radiculopathy or neuropathy, EMG results may be unreliable in limb muscles until a patient has had significant leg symptoms for over 3 weeks. Also, abnormal EMGs tend to normalize over time. There is some evidence that greater accuracy can be obtained in diagnosing lumbar nerve root compromise when information from needle EMG is combined in a systematic fashion with information from imaging tests and clinical findings, rather than relying on the results of each test alone. [49], [50]
For H-reflex and F-wave tests, three articles reported on accuracy in diagnosing nerve root problems. Aiello, Serra, Migliore, et al. [21] evaluated 25 patients with clinical evidence of L3 and/or L4 nerve root impairment. H-reflex tests were abnormal on the affected side in 96 percent of the 24 patients with L3 and/or L4 nerve root compromise confirmed at surgery, but the test was also positive in the 1 patient with no nerve root pathology noted at surgery (96-percent true positive rate, 0-percent true negative rate).
Aiello, Serra, Tugnoli, et al. [254] evaluated H-reflex tests and EMGs for 50 patients in whom a single disc prolapse was found at surgery. H-reflex tests were positive in 71 percent of 7 patients with L3-L4 disc herniations, 58 percent of 26 patients with L4-L5 disc herniations, and 100 percent of 17 patients with L5-S1 disc herniations. In addition, by combining information from H-reflex tests and needle EMG, 30 percent of single disc prolapses could be determined accurately.
Braddom and Johnson [256] evaluated H-reflex tests in 25 patients with clinically suspected S1 radiculopathy. A normal range was established in 100 asymptomatic subjects. All 25 patients had H-reflex-test latencies greater than 2 standard deviations above the mean for the control group. Only three patients were reported as having surgery, and long-term follow-up results were not given.
For surface EMG, two articles evaluated efficacy in assessing patients with low back symptoms. Arena, Sherman, Bruno, et al. [255] evaluated surface EMG of lumbar paraspinal muscles as a function of pain state. Surface EMG results were not significantly able to differentiate back pain patients with high pain states from those in low pain states. Sihvonen, Partanen, Hanninen, et al. [258] evaluated both needle and surface EMG of lumbar paraspinal muscles in 87 patients with back pain (not radiculopathy) longer than 6 months, but who had not had surgery, and in 25 controls with no history of back problems. When compared to the asymptomatic controls, the patients with back pain had significantly increased surface EMG activity while standing and immediately after lumbar flexion.
For SEPs, the only article reviewed [259] evaluated accuracy in 18 patients with clinical findings of suspected spinal stenosis who went on to have surgery. At operation, all patients were found to have spinal stenosis. In all but 1 of the 18, SEPs had been positive (94-percent rate).
Potential Harms and Costs
Inserting small needle electrodes into muscle tissue is invasive, causes some patients discomfort, and may cause bruising. Patients who have severe pain, low pain thresholds, excessive anxiety, or conflicting emotional symptoms may not be able to participate fully in the examination. [147] EMG and other electrophysiologic tests are moderately expensive.
Summary of Findings
The evidence suggests that in patients with low back problems who have a confusing clinical picture of severe leg symptoms of more than 3 to 4 weeks' duration, EMG and H-reflex tests appear to be useful (1) to document presence or absence of radiculopathy or neuropathy as the cause of symptoms in the lower extremities, (2) to provide more information on specific nerve roots that may be compromised, and (3) to help differentiate between acute and chronic nerve root dysfunction. Optimal time for needle-EMG testing is after the patient has had lower limb symptoms at least 3 to 4 weeks. Test results are not reliable before this time.
SEPs appear to be useful in diagnosing spinal stenosis and spinal cord myelopathy. However, F-wave tests and surface EMGs are not considered effective methods of assessing acute low back problems.
Accuracy of electrophysiologic testing is highly dependent on the skill with which the examination is performed. Clinicians are urged to assess the qualifications of the diagnostician before referring a patient with suspected neurologic compromise.
Bone Scan
Panel findings and recommendations:
Bone scanning, a type of radionuclide imaging, involves intravenous injection of radioactive compounds known to adhere to metabolically active bone. Gamma detectors localize regions of uptake. Most of the bone-seeking compounds used contain the radionuclide technetium- [99]m. The diagnostic objective is to detect occult fractures, infections, and bony metastases of the spine and to differentiate them from common benign pathology such as degenerative changes.
Literature Reviewed
Of 26 articles screened for this topic, 5 met criteria for review. [262]- [266]
Evidence on Efficacy
In the studies reviewed, bone scan was used to detect several different clinical conditions: stress fracture injuries of the pars interarticularis; [263] inflammatory sacroiliitis; [262], [264] spine infections; [266] metastatic cancer and other systemic disease; [265] and symptomatic spondylolysis. [263] All of these studies either evaluated mixed patient groups with both acute and chronic problems or did not report symptom duration. [264], [265] There were no studies focusing specifically on patients with acute low back pain.
The reference standard used depended on the clinical condition to be assessed. Included were: clinical diagnoses; [262]- [264] clinical follow-up or autopsy; [265] and biopsy with microbial cultures. [266]
Schütte and Park [265] evaluated bone scans for two groups. One group comprised 138 patients with a history of malignancy. In the other group, 38 patients with no previously recognized systemic disease had nonspecific low back pain and normal x-rays, but with strong clinical suspicion of an underlying serious condition causing the back pain. Of these 38 patients with "nonspecific" low back pain, 14 (37 percent) were later found to have a systemic disease. Of the 14 patients, 13 had elevated ESRs, but only 7 had positive bone scans (all 7 also with high ESRs). Of patients with a history of malignancy, 40 percent had positive bone scans determined on follow-up to be metastases and 14 percent had osteoporotic rib or vertebral fractures.
The authors concluded that bone scan has a high yield in patients with known malignancy. In patients where clinical suspicion of an underlying serious problem was high, but who had no known malignancy and normal x-rays, ESR detected 93 percent of those with systemic disease. Bone scan detected only 50 percent of these cases. The authors concluded that bone scan has a low yield in patients with longstanding low back problems and normal x-rays and lab tests.
Whalen, Brown, McLeod, et al. [266] evaluated patients with low back pain who had extensive diagnostic workups because of suspected spinal infections, and who then had open biopsy or percutaneous needle aspiration for culture and microbiologic diagnosis. Duration of symptoms before workup ranged from 2 weeks to 4 years (37 percent with symptoms for less than 3 months). One subgroup of 19 patients had all of these tests before spinal biopsy: technetium- [99]m (Tc- [99] m) bone scan, indium- [111] (In- [111] ) white blood cell (WBC) bone scan, plain lumbar x-rays, and ESR. Of the 19 patients, 16 had spinal infections confirmed on culture of biopsy material.
For the 16 patients, true positive rates were: 81 percent for Tc- [99]m bone scan, 19 percent for In- [111] WBC bone scan, 44 percent for plain x-rays, 82 percent for ESR > 20, and 56 percent for ESR > 50. False-negative rates for diagnosing spinal infection were: 3 of 3 (100 percent) for Tc- [99]m bone scan, 14 of 17 (82 percent) for In- [111] WBC bone scan, 8 of 11 (73 percent) for plain x-rays, 2 of 2 (100 percent) for ESR > 20, and 6 of 8 (75 percent) for ESR > 50. Half the infections were attributed to prior spinal surgery or instrumentation, with the rest attributed to hematogenous spread.
Miron, Khan, Wiesen, et al. [264] evaluated the accuracy of a quantitative bone scan technique, scintigraphy, for diagnosing sacroiliitis in various groups of patients. First, 90 subjects with no history of low back symptoms were evaluated with the test to establish age- and sex-specific normal values for a sacroiliac index. A positive test was defined as a sacroiliac index greater than two standard deviations above the mean for normals. In evaluating patients with low back pain, the test was positive in 50 percent of 18 patients who had signs and symptoms of active sacroiliitis. The test was positive in only 7 percent (1 patient) of 14 patients who had low back pain, but no clinical, x-ray, or CT-scan evidence of sacroiliitis. The authors concluded that this test has a low true positive rate (50 percent), but high true negative rate (93 percent) for diagnosing sacroiliitis.
Esdaile, Rosenthall, Terkeltaub, et al. [262] evaluated Tc- [99]m bone scan scintigraphy for diagnosing sacroiliitis. Normal values for sacroiliac joint-to-sacrum ratios on scintigraphy were established in 18 controls with no clinical evidence of inflammatory back pain. These ratios were found abnormally elevated in 66 percent of 12 patients considered to have "possible" ankylosing spondylitis and in 46 percent of 22 patients considered to have "definite" ankylosing spondylitis based on clinical and x-ray findings. At the time of the initial testing, all patients were taking very little or no anti-inflammatory medication. All were then treated with such medication. The S1 joint-to-sacrum ratios significantly decreased after treatment. The authors concluded that this technique is not a useful screening technique to detect early ankylosing spondylitis.
Potential Harms and Costs
The primary potential complications of bone scan involve exposure to ionizing radiation from the radionuclide injected. The total radiation dose to the patient is equivalent to a set of lumbar spine x-rays. This test is contraindicated during pregnancy. The radionuclide may be found in breast milk, and breast feeding must be discontinued for a brief interval after the test. Bone scans are moderately expensive.
Summary of Findings
The bone scan is a moderately sensitive test for detecting suspected tumor, infection, or occult fractures of the vertebrae in patients with low back pain, but not for specifying the diagnosis. A positive bone scan suggesting one of these conditions will usually need to be confirmed using other diagnostic tests or procedures. Bone scan has been shown to be moderately sensitive for detecting metastases to the spine in patients with a previously established diagnosis of cancer who present with acute low back problems. Bone scan also appears to be effective for detecting serious conditions, such as tumor, infection, or fracture, in patients where there is suspicion of these problems based on clinical findings. Bone scan appears to be more accurate than plain x-ray for detecting these conditions. No studies were found comparing the relative accuracy of bone scan versus CT scan or magnetic resonance imaging (MRI) scan for detecting the conditions.
Thermography
Panel findings and recommendations:
In patients with low back problems, thermography involves measuring small temperature differences between sides of the body and evaluating the patterns on infrared thermographic images of the back and lower extremities. Because thermography is noninvasive and involves no ionizing radiation, the test has been proposed as a physiologic test with clinical utility for documenting the presence or absence of radiculopathy (nerve root compression).
Literature Reviewed
Of 17 articles screened for this topic, only 1 met review criteria for adequate evidence about efficacy. [267] The panel also reviewed a meta-analysis on thermography. [268] Reviewed as well were four articles providing data on thermography in asymptomatic subjects without back problems. [269]- [272]
Evidence on Efficacy
The one study meeting review criteria [267] evaluated thermography in 107 patients who had sciatica of unspecified duration, 19 of whom went on to have low back surgery, and 28 asymptomatic subjects with no history of back problems and no evidence of disease affecting the lower extremities. All the asymptomatic subjects had temperature differences on thermography of less than 1.9 degreesC in the feet and less than 1.0 degreesC in other parts of the lower limbs. These values were used as the upper limits of normal for evaluating patients with sciatica. Of the 19 patients with sciatica who went on to have surgery, only 53 percent had results on preoperative thermography in agreement with surgical findings.
The most recent meta-analysis [268] reviewed 81 relevant citations and analyzed 28 studies of thermography used for diagnosing lumbar radiculopathy. Articles were graded excellent, good, fair, or poor based on the following criteria: technical quality of the reference test, uniform application of the reference test, independence of interpretations, clinical description, cohort assembly, and sample size. Only excellent and good studies were considered reliable sources of data on diagnostic accuracy. No study was graded excellent, 1 study was graded good, 3 were graded fair, and the remaining 24 were graded poor. Because of the methodological flaws in 27 studies, summary pooled statistics were not reported. The only study considered reliable [267] found no discriminant value for thermography in diagnosing lumbar radiculopathy. True positive and true negative rates were both 48 percent.
The four studies evaluating thermography in persons without back problems found abnormal thermography of the lower limbs in 7 to 81 percent of these asymptomatic subjects. Chafetz, Wexler, and Kaiser, [269] evaluating 15 asymptomatic subjects with no current back pain and no history of back surgery or disability from back pain, found that 40 percent had abnormal thermograms.
Harper, Low, Fealey, et al. [270] evaluated thermography in 37 asymptomatic subjects (carefully screened for no history of back pain, back surgery, or disease or injury affecting the lower extremities) as well as in 55 patients with clinically suspected radiculopathy. All thermograms were interpreted independently by five readers experienced in thermography who were blinded to all clinical data. The different readers interpreted thermograms as probably or definitely abnormal in 56 to 81 percent of the asymptomatic controls.
Perelman, Adler, and Humphreys [271] evaluated thermography in 16 asymptomatic subjects with no low back complaints and found 25 percent of these subjects to have abnormal thermograms. Tests were considered abnormal if the thermogram had an asymmetric visual pattern, but temperature differences were not measured. So, Aminoff, and Olney [272] evaluated thermography in 30 patients with symptoms of lumbar radiculopathy and in 27 asymptomatic controls. Thermogram readers were blinded to clinical data. Abnormal thermograms, defined as temperature differences between sides greater than three standard deviations from the mean for all asymptomatic subjects, were found in 7 percent of the asymptomatic subjects.
Potential Harms and Costs
No reports of significant risks from thermography were found. Thermography is considered moderately expensive.
Summary of Findings
The one study meeting review criteria found that thermography did not accurately predict either the presence or absence of lumbar nerve root compression found at surgery. In addition, several studies have shown thermography of the lower limbs as abnormal in a substantial proportion of asymptomatic subjects without back problems. Based on the available research evidence, thermography does not appear effective for diagnosing low back problems.
In addition to x-rays, the imaging studies most generally used to define a possible anatomic cause for evidence of physiologic abnormalities include plain myelography, MRI, CT, CT-myelography, discography, and CT-discography.
Abnormal findings on anatomic studies such as MRI, CT, myelography, and discography may be misleading, however, if they are not corroborated with evidence of physiologic abnormality from the medical history, physical examination, or physiologic tests. One problem with imaging studies is that in many patients, there is an inability to find any defects. Another problem is the lack of a "gold standard" in determining if an anatomic defect seen on imaging tests is actually the cause of symptoms. Anatomic abnormalities of the lumbar spine, such as degenerative changes and bulging or herniated discs, are found to increase with aging on x-rays and other imaging tests in subjects asymptomatic for low back problems.
Several studies stress the importance of not relying too heavily on imaging studies alone for assessment when nerve root compromise is suspected. The anatomic level of imaging study findings must correspond to the side and the level of concern physiologically detected through the history, physical examination, or other physiologic methods.
Plain X-Rays
Panel findings and recommendations:
X-ray, or radiography, is the oldest and most widely available modality for imaging the lumbar spine. The most commonly used x-ray views of the lumbar spine, the standard anteroposterior and lateral views, permit assessment of lumbar alignment, comparison of vertebral body and disc space size, assessment of bone density and architecture, and gross evaluation of soft tissue structures. Oblique views of the lumbar spine are used in the detection of unilateral or bilateral spondylolysis. Other special views include sacroiliac views to evaluate possible ankylosing spondylitis. The diagnostic objective of x-rays is to reveal the bony and structural abnormalities associated with back pain.
Literature Reviewed
Of the 128 articles screened for this topic, 20 articles reporting on 18 studies met criteria for review. [26], [276] - [294] Other articles contained information used by the panel, but did not meet article selection criteria. [295], [296]
Evidence on Efficacy
Two articles evaluated patients who had less than 3 months of symptoms. Two articles involved patients with chronic low back pain. [282], [292] Two articles had three separate groups, one asymptomatic, one with patients seen for acute low back problems, and a third comprising patients with chronic low back symptoms. The remaining 14 articles (reporting on 13 studies) involved a mix of patients with acute and chronic symptoms or did not report symptom duration.
Hansson, Bigos, Beecher, et al. [281] evaluated the degree of lumbar lordosis seen on x-rays in three groups of age-matched men engaged in heavy labor jobs. They included 200 asymptomatic subjects who had preemployment x-rays, 200 patients seen for acute low back problems, and 200 patients with low back disability longer than 6 months. Films were read by back specialists blinded to all other data. No differences were found between groups in the degree of lordosis noted on x-ray.
Deyo and Diehl [278] evaluated the use of a set of criteria based on medical history questions for selectively ordering x-rays in 621 patients presenting to a hospital emergency room with low back pain (patients with urinary tract symptoms excluded). The 11 criteria, any one of which would prompt an early x-ray, were: (1) age over 50, (2) significant trauma, (3) neuromotor deficits, (4) unexplained weight loss, (5) suspicion of ankylosing spondylitis, (6) drug or alcohol abuse, (7) history of cancer, (8) use of corticosteroids, (9) temperature greater than or equal to 100 F, (10) a return visit for the same problem within 1 month and not improved, and (11) patients seeking compensation for back pain.
X-ray findings were considered therapeutically important if they detected a malignancy or fracture. Of these patients who had x-rays, 227 met one or more of the criteria for x-ray, and 6.6 percent of these had therapeutically important findings. Another 84 patients had x-rays even though they did not meet any of the criteria. None of this group had therapeutically important x-ray findings. The highest diagnostic yield was in patients over age 50. Of the 119 patients in this group, 11 percent had therapeutically important findings (13 fractures and 2 malignancies). Strict use of the selective criteria would have resulted in x-ray studies in 390 patients.
Deyo and Diehl [26] evaluated 1,975 walk-in patients at a public hospital, their chief complaint back pain, in order to estimate the prevalence of cancer as an underlying cause of back pain. A search of an institutional tumor registry at least 6 months after the index visit identified 13 of these patients whose back pain was attributed to cancer. History findings significantly associated with the diagnosis of cancer were age over 50, prior cancer history, unexplained weight loss, pain lasting more than 1 month, and no improvement following conservative therapy. Laboratory test results significantly associated with cancer were an ESR over 20 and anemia. The authors presented an algorithm for ordering x-rays based on these history and lab test findings that would have resulted in 22 percent of the total group receiving x-rays including all patients who were found to have cancer.
Eleven articles evaluated x-ray findings in patients with low back problems, compared with asymptomatic subjects with no history of back problems. The findings of all of these studies were similar. In general, x-ray findings correlated poorly with low back problems. [276], [277], [279], [281], [284], [285], [287], [288], [291], [292], [294]
In all these studies, degenerative changes were noted in some persons with no history of low back problems whereas other persons with back problems showed no degenerative changes. When groups of subjects of similar age were compared, some studies show an increased prevalence of degenerative changes of the lumbar spine in those who have had back problems, compared to control groups with no history of back problems. Other studies found no significant difference in prevalence of degenerative changes between these groups.
These studies generally support the idea that degenerative changes of the spine, as seen on x-rays or other imaging studies, are not by themselves a cause of back pain. In fact, many authors suggest that degenerative changes of the spine are merely signs of aging of the back. Furthermore, degenerative changes were seen more commonly with increasing age for both those with and those without a history of low back problems.
A possible exception is spondylolisthesis, a forward slippage of a vertebra on the one below it. Two studies showed significantly higher prevalence of spondylolisthesis in patients with low back problems than in asymptomatic individuals. Torgerson and Dotter [294] found spondylolisthesis on x-rays in 4.9 percent of 387 symptomatic low back pain patients, but in only 1.5 percent of 217 asymptomatic subjects. Magora and Schwartz, [290] who evaluated adults currently working, found x-ray evidence of spondylolisthesis in 3.1 percent of 648 subjects with a history of low back pain patients, but in none of 376 subjects who had never had back pain.
Three other studies found no significant difference in prevalence of spondylolisthesis between groups with low back problems and asymptomatic controls. Biering-Sorensen, Hansen, Schroll, et al. [276] evaluated a group of men and women 60 years of age, including 308 with low back pain and 358 asymptomatic controls. This study found an overall prevalence of spondylolisthesis of 2.8 percent, with no significant difference between the groups of symptomatic patients and controls. Bigos, Hansson, Castillo, et al. [277] found no difference in incidence of spondylolisthesis or other abnormalities in the evaluation of age-matched males whether asymptomatic job applicants, back injury claimants, or disabled patients with greater than 6 months' duration of symptoms. Leboeuf, Kimber, and White [285] found spondylolisthesis on x-rays in 4.9 percent of patients with low back pain and in 5.5 percent of asymptomatic controls. This difference was not significant.
None of the studies reviewed on spondylolisthesis attempted to measure spinal instability, and most did not compare groups in terms of degree of spondylolisthesis. In addition, these studies did not investigate whether there was any therapeutic benefit from determining if a patient has spondylolisthesis (especially in patients with no findings that suggest nerve root compression).
Some authors maintain that adults with severe spondylolisthesis (degree of slip greater than 50 percent or a severe increase in affected joint motion) may require special treatment. [295] However, the degree to which spondylolisthesis and abnormal motion may benefit from special interventions is controversial and beyond the scope of this guideline.
Other reported findings on lumbar x-rays for adult patients with low back problems included: transitional vertebrae (lumbarization or sacralization), spina bifida occulta, increased or decreased lordosis, mild or moderate scoliosis and spondylolysis (an interarticular defect of the posterior vertebral arch), and degenerative joint disease. These findings were reported in similar frequency for 200 subjects without symptoms, for 200 subjects reporting back injury claim, and for 200 subjects disabled more than 6 months. This confirms multiple studies that have questioned both the use of lumbar radiographs for preemployment screening and the diagnostic significance of many radiologic findings.
Spondylolysis without spondylolisthesis is equally common in persons with and without low back symptoms. [277] Spondylolysis has not been documented to be a cause or precursor of low back problems in adults, and no special treatment is required.
Potential Harms and Costs
Potential harms associated with lumbar spine x-rays are primarily related to the degree of ionizing radiation exposure. Small cumulative doses of ionizing radiation are believed to present minimal or no risks. But lumbar x-rays expose the male and female reproductive organs, especially with routine use of oblique views or repeated exposures. These practices are of questionable value and a particular concern for younger females. Oblique lumbar views approximately double total radiation exposure, compared to standard views, which alone are equivalent to female gonadal radiation of daily chest x-rays for 6, 16, or 96 years, depending upon the machine. [296] Lumbar spine x-rays are seldom indicated during pregnancy.
The cost of a lumbar spine x-ray is low compared to other imaging modalities such as bone scan, CT, or MRI, and x-rays are more readily available.
Summary of Findings
Plain lumbar x-rays have been demonstrated to be useful in helping detect or define spinal fractures, but alone do not rule in or out tumors or infections suspected by other findings (such as when red flags are present). Evidence suggests plain x-rays are rarely useful in evaluating or guiding treatment of adult acute low back pain in the absence of red flags. Plain x-rays are not effective for diagnosing lumbar nerve root impingement of herniated disc or spinal stenosis, or for ruling out cancer or infection.
The use of lumbar x-rays to screen for spinal degenerative changes, congenital anomalies, spondylolysis, spondylolisthesis, or scoliosis very rarely adds useful clinical information. Only 1 of 2,500 x-rays detects something not suspected on medical history and physical examination that has an impact on patient care. Even in the rare cases where a condition may be clinically significant, the history and physical examination findings (that is, evidence of neurologic dysfunction) should dictate more extensive diagnostic evaluation whether a routine x-ray screening is positive or negative. Oblique lumbar x-rays, usually done to screen for spondylolysis, rarely add useful clinical information in adults, and they double the x-ray dose to the patient. Patients with spondylolisthesis can be safely treated in the same fashion as those with other types of acute low back problems. Thus, x-rays done specifically to screen for the presence of spondylolisthesis are unnecessary in adults during the first 3 months of symptoms.
CT, MRI, Myelography, and CT-Myelography
Panel findings and recommendations:
Introductory Discussion.
The four imaging tests commonly used in assessing the anatomy of the lumbar spinal canal and its contents are plain myelography, CT scan, MRI scan, and CT-myelography. These four tests are discussed as a group because they are used in similar clinical situations, provide similar types of information, and are often compared with each other in research studies. Evaluation is limited by lack of a gold standard for evaluating efficacy. Each test and the type of information it provides are described briefly as follows:
Significant technological advances have taken place in these imaging modalities over the past several years. Kent, Haynor, Larson, et al. [297] have suggested technical criteria for the performance of these imaging tests to assure a minimal level of quality. Studies of imaging tests were not considered by the panel if the technical protocols were inadequately described or if the protocols varied significantly among subjects within a study. The panel used the following technical criteria for including studies of individual imaging modalities:
The objective of using these imaging tests for patients with acute low back problems is to define medically or surgically remediable anatomic pathological conditions. Therefore, the tests are not done routinely, but are generally used only for patients who present with one of these three clinical situations:
This section assesses the usefulness of the four imaging tests for diagnosing nerve root compromise due to herniated discs or spinal stenosis. The use of imaging tests for evaluating other serious conditions affecting the spine is beyond the scope of this guideline and is not discussed in detail here.
Imaging Tests to Evaluate Suspected Nerve Root Compromise Due to Lumbar Disc Herniation
Literature Reviewed
Overall, 308 articles were screened for the subject of spinal imaging tests. They included 141 for CT scan, 97 for MRI, and 70 for myelography (including CT-myelography). Of the 308, there were 17 articles meeting criteria for review that evaluated lumbar disc herniation as an anatomic cause for suspected nerve root compromise. Other information used by the panel came from Sackett, Haynes, Guyatt, et al. [311] All of these studies used surgical findings as a reference test.
Evidence on Efficacy
Four articles evaluated plain myelography alone. Three of the four evaluated only patients with no history of prior back surgery. One included patients with prior back surgery.
In the four studies, lumbar disc herniations were found at surgery in 68 to 96 percent of patients. Studies evaluating the true positive rate and true negative rate of a diagnostic test are generally considered more accurate when the target condition is present in 50 percent of the population studied. [311] Only two of these four studies had prevalence rates for lumbar disc herniation below 80 percent. Aejmelaeus, Hiltunen, Härkönen, et al. [20] studied a group with a 68-percent prevalence of disc herniation at surgery and calculated the true positive rate of 75 percent and true negative rate of 55 percent for myelography in diagnosing this condition. Herron and Turner, [30] found a disc herniation at surgery 74 percent of the time, and the true positive rate and true negative rate for myelography were 88 percent and 62 percent, respectively. The remaining two articles found a lumbar disc herniation at surgery in 84 to 96 percent of patients. In these studies, myelography was calculated to have a true positive rate of 83 to 94 percent and a true negative rate of 71 to 100 percent for diagnosing lumbar disc herniation. A total of eight studies evaluated CT scan compared with myelography. [22], [298] - [300], [304], [307] - [309] Only two of the studies looked at patient groups who had no prior back surgery. [22], [307] Two studies included some patients with prior surgery. [304], [309] The remaining four studies did not report on this variable.
For diagnosing lumbar disc herniation, all eight studies reported similar ranges of true positive and true negative rates for both tests, and these results were also similar to those from studies of myelography alone. The number of subjects ranged from 37 to 195, and prevalence of lumbar disc herniation found at surgery varied from 55 to 91 percent. The calculated true positive rate of the tests for diagnosing lumbar disc herniation varied from 60 to 91 percent for CT scan and from 65 to 98 percent for myelography. The true negative rate varied from 57 to 100 percent for CT scan and from 43 to 100 percent for myelography. One study allowed estimation of the added diagnostic value of combining information from CT and myelography for the same patient. [309] This study found similar accuracies for CT and myelography when evaluated separately for diagnosing lumbar disc herniation (sensitivities 77 percent and 78 percent, specificities 83 percent and 72 percent). However, when the results of both tests were evaluated together, the true positive and true negative rates were 91 percent and 56 percent for a positive result defined as either one of the two tests being positive. True positive and true negative rates were 64 percent and 100 percent if a positive result was defined as both tests being positive. This implies that the probability that a true lumbar disc herniation will be detected on imaging is 77 percent if one test is done and 91 percent if both tests are done. This also implies that the probability of an imaging test showing a false-positive lumbar disc herniation is 17 percent or 28 percent if one test is positive, but approaches zero if both tests are positive.
The five remaining articles evaluated multiple imaging tests done in the same patients. [302], [303], [305], [306], [310] MRI scan was compared to plain myelography, [310] to CT-myelography, [305] to both plain and CT-myelography, [306] and to CT, plain myelography, and CT-myelography. [303] Another study, also by Jackson, Cain, Jacobs, et al., [302] evaluated CT, myelography, and CT-myelography and compared them as well to discography and CT-discography. The five studies all found no significant differences between CT, MRI, and CT-myelography in terms of their true positive rates and true negative rates for diagnosing lumbar disc herniation although all these tests were better than plain myelography.
Jackson, Cain, Jacobs, et al. [302] found that for diagnosing lumbar disc herniation, CT-discography had a significantly greater true positive rate (92 percent) than CT-myelography (78 percent), plain CT (72 percent), plain myelography (70 percent), or plain discography (31 percent). However, in a subsequent study, Jackson, Cain, Jacobs, et al. [303] recommended MRI over other imaging tests as it is noninvasive and exposes the patient to no ionizing radiation. No differences were found between CT-discography, CT-myelography, CT, or myelography in the true negative rates although all had a significantly higher true negative rate than plain discography.
Imaging Tests to Evaluate Suspected Spinal Stenosis
Literature Reviewed
Lumbar spinal stenosis involves impingement of the cauda equina nerves in the spinal canal, lateral spinal canal, or neural foramina. This is usually a degenerative condition resulting from ligamentous infolding and bony hypertrophy commonly seen in persons over age 60. Spinal stenosis is occasionally developmental, due to congenitally short pedicles, and can affect younger individuals.
One meta-analysis on the accuracy of CT, MRI, and myelography for diagnosing lumbar spinal stenosis in adults was reviewed [297]. Of the 116 articles the authors screened for this meta-analysis, 14 studies met their inclusion criteria for review. [273], [275], [306], [309], [312] - [321]
Evidence on Efficacy
In their meta-analysis, Kent, Haynor, Larson, et al. [297] concluded that estimates of accuracy of the imaging tests for diagnosing spinal stenosis were imprecise and that all 14 studies had methodological flaws (all judged to be of fair or poor quality). However, based on data available, the meta-analysis found CT and MRI of similar accuracy for diagnosing spinal stenosis (true positive and true negative rates approximately 90 percent and 80 percent) and plain myelography with lower accuracy. The authors cautioned that because of bias, estimates of test accuracy obtained by the meta-analysis were likely to be too high.
Spinal Imaging Findings in Asymptomatic Subjects
Literature Reviewed
Six articles were found that evaluated lumbar spinal imaging findings in asymptomatic subjects with no low back symptoms. These studies included one evaluating CT scan, four on [sup]MRI, and one for plain myelography. Other articles contained information used by the panel, but did not meet article selection criteria.
Evidence on Efficacy
Wiesel, Tsourmas, Feffer, et al. [275] evaluated readings of CT scans for 52 subjects with no history of low back problems, with all scans read independently by three neuroradiologists blinded to other data. For those under age 40, herniated discs were diagnosed in an average of 19. 5 percent of subjects (range for the three readers, 13 to 24 percent). For subjects over age 40, those who had abnormal findings averaged 50 percent (with a range of 30 to 82 percent among the readers). Included were 27 percent of subjects diagnosed with herniated discs, 10 percent with facet joint hypertrophy, and 3 percent with spinal stenosis. Technical quality of this study was considered adequate.
Boden, Davis, Dina, et al. [273] evaluated readings of MRI scans in 67 subjects with no history of back problems. Scans were read by three neuroradiologists blinded to all other data after the scans were randomly mixed with scans of symptomatic patients who had proven back pathology. Of the asymptomatic subjects, 35 were age 20 to 39, 18 were age 40 to 59, and 14 were age 60 and over. The percentages for each of the above age groups were reported respectively by neuroradiologists as: a definite or probable abnormality in 22 percent, 22 percent, and 57 percent; bulging disc in 56 percent, 50 percent, and 79 percent; disc herniation in 21 percent, 22 percent, and 36 percent; degenerative disc in 34 percent, 59 percent, and 93 percent; spinal stenosis in 1 percent, 0 percent, and 21 percent. This study was considered of good technical quality.
Paajanen, Erkintalo, Dahlström, et al. [291] evaluated MRI scans in age- [20] male military conscripts including 75 subjects with low back pain and 34 controls with no history of low back problems. Five intervertebral discs, from L1-L2 to L5-S1, were evaluated for each subject. Disc degeneration, indicated by reduced MRI signal intensity for the disc, was found in 57 percent of patients with low back problems and 35 percent of controls. The authors stated that it was unclear if the positive findings in controls represented pathological processes or merely normal aging changes that did not predispose to future low back problems. The technical quality of the MRI scans in this study was considered suboptimal because low field strength MRI (0.02 T) was used.
Powell, Wilson, Szypryt, et al. [322] evaluated the MRI scans in 302 women who had no symptoms of low back problems, but who had the scans done for nonback obstetrical problems. Using reduced MRI signal intensity of the disc as an indication of disc degeneration, the authors found one or more degenerative discs in 34 percent of women age 21 to 30, in 60 percent of women age 31 to 40, and in 95 percent of women by age 70. Bulging discs were found on MRI in 11 percent of 82 pregnant women and 13 percent of 56 women who had never been pregnant (these data not presented by age group).
Weinreb, Wolbarsht, Cohen, et al. [323] evaluated MRI findings in 45 pregnant women age 20 to 39 and in 41 nonpregnant women age 19 to 40 with no current low back symptoms. Three intervertebral disc levels, L3-L4, L4-L5, and L5-S1, were evaluated for all subjects. No significant differences were found between pregnant and nonpregnant women in terms of the percentage with lumbar disc herniation (9 percent compared with 10 percent) or disc bulging without herniation (44 percent in each group). The technical quality of this study was considered suboptimal because testing protocols varied between subjects and low field strength MRI (0.35 T) was used.
Hitselberger and Witten [274] reviewed lumbar myelograms done in 300 patients with no prior history of radiculopathy. The technical quality of this study was considered poor because oil-based contrast media were used, which are less sensitive than more modern techniques. Still, 24 percent had myelographic evidence of lumbar disc herniation, 9.3 percent had spinal stenosis without a history of radicular symptoms (1 of 300 with a complete block of the dye). This study was of limited value because findings were not given by specific age groups, and the age range of subjects was 18 to 76 with a mean age of 51.
Degenerative discs, bulging discs, and even herniated discs are part of the aging process for the spine and may be irrelevant findings; they are seen on imaging tests of the lumbar spine in a significant percentage of subjects with no history of low back problems. Therefore, abnormal imaging findings seen in a patient with acute low back problems may or may not be related to that individual's symptoms. A herniated disc noted on an imaging test is more likely to be associated with a clinically significant nerve root compromise in patients when there are other findings (such as leg pain, positive straight leg raising, neurologic deficits, or a positive electrodiagnostic test) that suggest physiologic nerve root compromise. [30], [40], [49], [50]
Potential Harms and Costs
Factors that may influence the decision on which imaging test to use in diagnosing low back problems include the following: (1) tissue of greatest interest for imaging (CT better for bone, MRI better for imaging neural tissues and bone marrow and for diagnosing tumor or infection); (2) claustrophobia (more of a problem for MRI); (3) obesity (both CT and MRI scanners have a maximum table weight, so that extremely heavy patients may need to have myelography); (4) presence of internal metallic objects such as implanted medical devices, metallic surgical clips, or metallic objects or fragments in the eye, which can be a major problem for MRI (and sometimes for CT); (5) preference of the consultant and of the patient; (6) availability, cost, and potential side effects of the test.
CT-myelography and myelography have a higher risk of complications than CT or MRI (for example, post-spinal-tap headaches and adverse reactions to contrast media). For CT scan, potential harms include minimal x-ray exposure (including gonadal radiation exposure in females). Amount of exposure (less than two rads) is similar to that from two standard x-ray views of the lumbar spine. For MRI scan, there have been no clearly documented adverse health effects. Long-term effects of magnetic field exposure from MRI are unknown, but this test is generally believed to involve minimal risk. CT scan, MRI scan, CT-myelography, and plain myelography are all considered moderate to expensive in cost.
Summary of Findings
Given the benign natural history of acute low back problems, with 80 to 90 percent of patients expected to improve at 1 month even without treatment, routine spinal imaging tests are not generally necessary during the first month of symptoms except when a red flag (suggesting a medically emergent condition) is noted on medical history and physical examination. After 1 month of symptoms, the use of imaging tests may be appropriate when surgery is being considered for a specific detectable loss of neurologic function or to further evaluate possibly serious spinal pathology in the presence of red flags.
Discography
Panel findings and recommendations:
Discography involves the injection of a water-soluble imaging material directly into the nucleus pulposus of the disc. Information is then recorded about the amount of dye accepted, the pressure necessary to inject the material, the configuration of the opaque material, and the reproduction of the patient's pain. There are two diagnostic objectives: (1) to evaluate radiographically the extent of disc damage on discogram (sometimes with the addition of CT) and (2) to characterize the pain response (if any) on disc injection to see if it compares with the typical pain of the patient. A symptomatic degenerative disc is considered one that disperses injected contrast in an abnormal pattern, extending to the outer margins of the annulus and possibly into epidural space as well. For many investigators, a painful reaction provoked in the patient that reproduces the patient's usual pain is required to classify the disc as abnormal.
Literature Reviewed
Of the 42 articles evaluated for this topic, only 1 met review criteria for adequate evidence about efficacy. [324] Another article contained information used by the panel, although it did not meet article selection criteria. [325] There were also two articles reviewed that evaluated results of discography in asymptomatic subjects. [326], [327]
Evidence on Efficacy
No studies were found that evaluated discography for patients with acute low back problems. One of the major problems in evaluating the literature on discography is that few studies evaluate discography using an independent reference standard. Instead, many studies either compare discography results with other diagnostic test findings or evaluate discography using pain provocation on disc injection as evidence of discogenic pain, which essentially means using part of a test to validate itself.
In the only study to meet panel review criteria, Colhoun, McCall, Williams, et al. [324] evaluated the results of discography using surgical findings and long-term clinical outcomes as independent reference standards. This study evaluated discography in 195 patients with persistent low back pain (symptom duration not otherwise specified), but with no history of prior back surgery. All patients went on to have back surgery (spinal fusion for 82 percent of patients, laminectomy and/or discectomy for the remaining patients). All patients were followed for 2 to 10 years postoperatively (results not presented separately by type of operation). Patients who had spinal fusion were excluded from the study if the surgery was deemed to be technically unsuccessful (that is, if there was x-ray evidence of pseudoarthrosis at the site of attempted fusion). Treatment success on follow-up was noted in 89 percent of 137 patients who had positive pain response on discography and abnormal discograms, compared to 52 percent of 25 patients who had negative pain response but abnormal discograms and 50 percent of 12 patients who had a negative pain response and normal discography.
Holt [326] evaluated discograms done in 30 male prison inmate volunteers who had no prior history of low back problems, normal lumbar x-rays, and normal back examinations. Their age range was 21 to 49, average age 26. Discography was attempted at the L3-L4, L4-L5, and L5-S1 disc levels for each subject. Of the 71 successfully performed discograms, a positive pain response was noted in 37 percent of the discs injected. All of these also had abnormal discograms (showing either degenerative changes or disc rupture). The remaining 63 percent of discs injected had negative pain responses and normal discograms. Holt interpreted these results as showing a 37-percent false-positive rate for discograms. However, in a reevaluation of this study, Walsh, Weinstein, Spratt, et al. [327] noted inconsistencies in Holt's data and recalculated the false-positive rate as either 26 percent or 4 percent depending upon assumptions made.
Walsh, Weinstein, Spratt, et al. [327] evaluated CT-discography done in 7 patients with low back pain and in 10 "asymptomatic" subjects with no history of low back problems. Discography was attempted at three lumbar disc levels for each subject, with a water-soluble nonionic contrast media. Disc injection was videotaped, and the subjects' pain reactions and discograms were later read independently by two orthopedic surgeons and three radiologists blind to all other data. Discography in the patients was considered positive if the discogram was abnormal, if there were two or more videotaped pain behaviors, and if disc injection provoked the patient's typical pain. In asymptomatic subjects, discography was considered positive if the discogram was abnormal and there was significant pain noted on disc injection. Discography was positive in all 7 patients with low back problems (65 percent of the 13 discs successfully injected being abnormal). In the asymptomatic subjects, 50 percent had an abnormal discogram (17 percent of the 30 successful discograms for this group), but none had positive pain response on disc injection. Therefore, none of the asymptomatic subjects was considered to have positive discography (that is, no false- positive tests).
Potential Harms and Costs
Discography is an invasive procedure with risk of complications. Potential complications include disc and disc space infections, disc herniation following disc injection, and significant amounts of ionizing radiation exposure with CT-discography (estimated at 1.5 to 4.0 rads when studying 2-3 discs). [325] Discography is expensive.
Summary of Findings
Although discography seeks to identify internal changes in the disc based on evaluation of a discogram and pain response on disc injection, the disease process is not clear (the internal disc disruption), and how to use the information for acute low back problems is not clear. The main reason put forward for using discography appears to be to determine the levels at which spinal fusion will be successful in patients with persistent low back problems (due to discogenic disease). This assumes the controversial premise of a "painful disc syndrome" which has not yet been adequately documented.
There is no good evidence that discography is useful to promote better treatment outcomes in patients with acute low back problems. Colhoun, McCall, Williams, et al. [324] noted more successful outcomes after back surgery for those with a positive discography, but these were presumably patients with chronic problems (as they had persistent pain). The rationale for using discography is to select patients who would most benefit from spinal fusion. Yet, in the Colhoun article, the predictive value of positive discography in establishing which patients do well after spinal fusion cannot be determined accurately because 18 percent of patients did not have fusions and outcomes were not reported separately for fusions and discectomies. Moreover, the two articles on discography in asymptomatic subjects report a substantial percentage of subjects who had positive discograms although they had never had low back problems.
In summary, there is limited evidence that discography can help select patients who would benefit from spinal fusion and no evidence that it is helpful in patients with acute low back problems. Potential serious risks from discography, including disc infection, have been identified. The use of discography or CT-discography to diagnose herniated discs appears to offer no significant advantage over other imaging methods with less potential risk of harm.
Surgery is commonly discussed for back symptoms that are unresolved after special studies (Attachment A4). Patients may benefit from general information about the risks and potential outcomes of surgical treatment for different diagnoses.
|
|
|
A4. Surgical considerations for patients with persistent sciatica |
Surgery for Herniated Disc
Panel findings and recommendations:
Surgery for herniated discs is invasive and comprises all types of surgical and injection techniques to remove or reduce the size of herniated intervertebral discs that compress nerve roots. Included are standard discectomy, microscopic discectomy, percutaneous discectomy, and chemonucleolysis (chymopapain injection). The therapeutic objective is to relieve pressure on nerve roots and reduce pain and possibly weakness and/or numbness in the lower extremities.
Literature Reviewed
Of 345 articles screened for this topic, 13 reporting on 10 studies met criteria for review. [322], [328] - [339] In addition, a meta-analysis article was reviewed by the panel. [340] Other articles contained information used by the panel, but did not meet article selection criteria. [30], [40], [49], [50], [341] - [345]
Evidence on Efficacy
Three of the studies reviewed were randomized controlled trials (RCTs) that evaluated chymopapain as compared with standard discectomy for patients with symptoms and findings of lumbosacral radiculopathy. Crawshaw, Frazer, Merriam, et al. [328] found that at 1-year follow-up, 85 percent of those undergoing discectomy had good or excellent results, compared to 44 percent of those receiving chymopapain injections. Both groups had improved leg symptoms, but only the discectomy group had significant improvements in back pain.
Ejeskär, Nachemson, Herberts, et al. [329] found that at 6 months, 56 percent of patients initially receiving chymopapain injections had undergone surgery due to unrelieved symptoms (all of these patients with disc herniation confirmed at surgery). When patients were followed up during the first 6 months before any treatment crossovers occurred, those receiving discectomy reported significantly greater improvement in symptoms than those receiving chymopapain injections.
Van Alphen, Braakman, Bezemer, et al. [336] found that at 1-year follow-up, physicians rated significantly more of the patients in the discectomy group as having good results from their initial treatment compared with the chymopapain group (85 percent compared with 63 percent). Also, 25 percent of the chymopapain group required subsequent discectomy while only 3 percent of the discectomy group needed a second operation. Open discectomy following prior failed chymopapain injection was successful in 44 percent of the cases.
Another RCT (reported in Fraser; [330] Fraser; [331] and Gogan and Fraser [332]) evaluated chymopapain injections compared with intradiscal saline injections in patients who had sciatica and evidence of a herniated lumbar disc, but who had not improved after 6 months of conservative therapy. Treatment success rates were significantly better for the chymopapain group than for the saline group at 6-month follow-up (80 percent compared with 57 percent), at 5-year follow-up (73 percent compared with 47 percent), and at 10-year follow-up (80 percent compared with 34 percent). Also, significantly fewer patients required a laminectomy for unrelieved symptoms in the chymopapain group compared with the saline group when followed up at 2 years (20 percent compared with 40 percent) and at 10 years (20 percent compared with 47 percent).
A double-blind RCT by Javid, Nordby, Ford, et al. [333] evaluated chymopapain injection compared with intradiscal saline injection in 108 patients with sciatica who had not improved after at least 6 weeks of conservative treatment including 2 weeks of bed rest. All patients had positive straight leg raising, a neurologic defect on physical examination, and myelogram evidence of a single lumbar disc herniation. At 6 months postinjection, the treatment success rate was significantly better for the chymopapain group compared with the saline injection group (83 percent compared with 42 percent).
Revel, Payan, Vallee, et al. [334] evaluated chymopapain injections compared with percutaneous discectomy in 141 patients with sciatica who did not improve after 1 month of conservative treatment. Overall success rates were significantly better for the chymopapain group than for the percutaneous discectomy group at both 6-month follow-up (61 percent compared with 44 percent) and 1-year follow-up (66 percent compared with 37 percent). Also, fewer patients in the chymopapain group required open laminectomy within 1 year due to unrelieved symptoms as compared with the percutaneous discectomy group (7 percent compared with 33 percent).
Only one RCT (reported by Weber [338], [339] ) compared standard discectomy with conservative (nonsurgical) care. This study looked at 280 patients who consecutively presented to a hospital neurology department with severe sciatica and clinical findings of possible or definite L4-L5 or L5-S1 disc herniation. All patients were initially hospitalized for 2 weeks of conservative treatment including 1 week of strict bed rest. After 2 weeks, 87 patients with possible but indefinite disk hernia who had shown continuous improvement were assigned to continued conservative care, and discectomy was performed for 67 patients who were deemed by their surgeon to have emergent indications for immediate surgery (intolerable pain, suddenly occurring or progressive muscle weakness, or impending bladder or anal sphincter paresis). This left a group of 126 subjects who had continued sciatic symptoms provoked by mild exercise, sitting, or Vasalva maneuver and with myelograms that showed definite disc herniations consistent with their clinical findings of neurologic dysfunction. Patients in this latter group were randomly assigned to receive either standard discectomy or continued conservative treatment.
Of these 126 subjects with definite disc hernia who were randomized, Weber [338], [339] found good or fair results in 61 percent of the nonsurgery group and in 90 percent of the discectomy group at 1-year follow-up. This difference was no longer significant on follow-up at 4 years (86 percent compared with 89 percent) or 10 years (93 percent compared with 92 percent). At 4-year follow-up, considerable sciatic pain was still reported by 9 to 10 percent of each group and considerable low back pain by 11 to 12 percent of each group. At 10-year follow-up, no patients in either group reported these symptoms. During the first year, 26 percent of the nonsurgery group demanded discectomy because of unrelieved sciatic pain. On follow-up, good or fair results were reported for 82 percent of this group at 4 years and for 100 percent of the group at 10 years.
Tullberg, Isacson, and Weidenhielm [335] evaluated microdiscectomy compared with standard discectomy in a RCT of patients with sciatica who had not improved after 2 months of conservative treatment and had evidence on CT scan of a single-level disc herniation. At 1-year follow-up, no significant difference was noted between microdiscectomy and standard discectomy groups in terms of patients reporting excellent or good results (86 percent compared with 90 percent), mean postoperative time off work (10.4 weeks compared with 10.1 weeks), or mean improvement in visual analog pain scale ratings over the prior year.
A meta-analysis for herniated lumbar disc surgery by Hoffman, Wheeler, and Deyo [340] found only two RCTs. [336], [338], [339] This meta-analysis concluded that patients with severe leg symptoms and confirmed lumbar disc herniation experienced faster symptom relief and improved functioning if they underwent standard discectomy rather than conservative treatment. The meta-analysis stated that there was inadequate evidence available to determine the efficacy of microdiscectomy or percutaneous discectomy for treating low back problems. However, percutaneous discectomy was noted to have a higher reoperation rate than standard discectomy. Discectomies were noted to be relatively safe procedures, but reoperations were also reported to be fairly common.
Several studies have emphasized the role psychosocial factors play in influencing the outcome of surgery for herniated disc. [30], [40], [49], [50] In fact, Spengler, Ouellette, Battié, et al. [50] found that psychological factors, especially elevated hysteria or hypochondriasis scales on a Minnesota Multiphasic Personality Inventory (MMPI), were better predictors of surgical outcome than were findings on imaging studies.
Potential Harms and Costs
Reported complications of herniated disc surgery include operative mortality, wound infection, discitis, dural tears, nerve root injuries, thrombophlebitis and pulmonary emboli, meningitis, cauda equina syndrome, psoas hematoma, vascular injuries, and risks associated with transfusions. Hoffman, Wheeler, and Deyo [340] stated that, overall, complications appeared to occur infrequently, but that information on complications was often hard to interpret in the studies reviewed, making determination of rates difficult.
A community-based study in Michigan, which reviewed the hospital discharge records of over 28,000 patients who had a lumbar disc surgery in 1980, reported incidence rates of 0.06 percent for mortality, 0.3 percent for infections treated with intravenous antibiotics, and 0.3 percent for major neurologic complications. A similar study of hospital discharge records in Washington State found an overall mortality incidence of 0.07 percent for spinal surgery. [345]
The reported complications for chymopapain therapy include allergic reactions (some resulting in death), discitis, thrombophlebitis, pulmonary embolus, neurologic injury, vascular injury, and transverse myelitis. [341]- [344] Skin tests for sensitization before chymopapain injection are reported to significantly reduce the risk of allergic reaction. Transverse myelitis is uncommon, and the risk factors for this are unclear.
Complication rates for discectomy are generally low. Complication rates for chymopapain are also low, but the use of chymopapain has decreased drastically in the United States because of concerns about transverse myelitis and anaphylactic reactions. The use of tests for allergic sensitization to chymopapain before this treatment may reduce the risk of allergic reaction.
Surgery for herniated discs is considered an expensive treatment.
Summary of Findings
Lumbar discectomy may relieve symptoms faster than continued nonsurgical therapy in patients who have severe and disabling leg symptoms (associated with clinical examination findings of definite lumbar nerve root compromise) and who have not improved after 4 to 8 weeks of adequate nonsurgical treatment. However, the evidence also showed that in such nonemergent patients, there appears to be little difference in long-term outcomes at 4 and 10 years between discectomy and conservative care.
There are direct methods of nerve root decompression and indirect methods. The best results from herniated disc surgery were with direct methods of standard discectomy and microscopic discectomy with no significant difference in results noted between these procedures. Studies indicate that the direct method of standard discectomy produces better results than the indirect method of chymopapain. Chymopapain is better than placebo injections of saline or the indirect method of percutaneous discectomy. Rates of initial treatment failure requiring a subsequent surgery are higher for chymopapain than for discectomy.
No studies to date have shown that any of the newer indirect methods of disc surgery, such as indirect automated percutaneous and percutaneous laser discectomy, produce better results than standard discectomy or chymopapain in appropriate patients.
Patient preference does and should play a large role in the surgical decision, but only if adequate information is available about efficacy, risks, and expectations.
Surgery for Spinal Stenosis
Panel findings and recommendations:
Spinal stenosis includes any constriction or narrowing of the central spinal canal, the lateral recesses, or foramina resulting in compression of nerve roots and/or the cauda equina. Surgery for spinal stenosis may include various types of surgical techniques, usually including decompressive laminectomy (sometimes combined with discectomy and/or spinal fusion) done to alleviate the symptoms of neural compression.
Spinal stenosis is generally a degenerative condition affecting patients over age 60 and is usually related to a variety of age-related changes in spinal anatomy that combine to cause compression of the cauda equina in the lumbar spinal canal and neuroforamina. These age-related changes may include disc bulges and herniations, thickening of the infolded ligamentum flavum, degeneration of the facet joints and joint capsules, osteophytes, and occasionally degenerative spondylolisthesis. There are also some younger individuals with severe congenital narrowing of the spinal canal who have spinal stenosis symptoms, but this is uncommon.
The primary symptoms of severe spinal stenosis are neurogenic claudication (leg pain with walking or standing, relieved by sitting or spinal flexion) and occasionally weakness of the legs.
Literature Reviewed.
Of the 40 articles screened for this topic, only one met criteria for review. [346] In addition, the panel reviewed an attempted meta-analysis on the topic. [66] Other articles contained information used by the panel, but did not meet article selection criteria. [347], [348]
Evidence on Efficacy.
No RCTs were found evaluating surgery compared with nonsurgical treatment for spinal stenosis. However, a controlled trial by Herkowitz and Kurz [346] compared decompressive laminectomy done with and without spinal fusion in patients with chronic low back problems (mean symptom duration 3.0 years). None of the patients had improved after adequate conservative treatment, and all had findings consistent with degenerative spondylolisthesis and spinal stenosis on CT, MRI, or myelogram. Internal fixation using metal devices was not done as part of the fusion procedure. Immediately following surgery, the fusion group reported significantly more pain relief in the back and legs than did the nonfusion group. At long-term follow-up (mean follow-up time of 3.0 years), the percentage of patients reporting excellent or good outcomes was significantly greater for the fusion group than for the nonfusion group (96 percent compared with 44 percent).
An attempted meta-analysis reviewed 74 studies involving patients who had decompressive laminectomy for lumbar spinal stenosis. [66] The authors of the attempted meta-analysis found three prospective studies, but no randomized controlled trials comparing surgery with conservative treatment. Therefore, no conclusions could be drawn as to the relative benefits and risks of surgery compared with conservative treatment. One study reported that of 27 unoperated patients with spinal stenosis, 19 remained unchanged, 4 improved, and 4 deteriorated during a follow-up period of 10 to 103 months with a mean of 49 months. [347] A comparison of these outcomes by Turner, Ersek, Herron, et al. [66] suggested that patients may show more improvement with surgery, but conservative management may be a reasonable alternative.
Of the 74 studies reviewed by Turner, Ersek, Herron, et al., [66] 31 provided sufficient information to calculate the proportion of patients with good-to-excellent as compared with poor-to-fair outcomes. Criteria for classifying outcomes into categories of excellent, good, fair, and poor varied across studies, making it difficult to combine and compare studies. When results were classified using a standard method for each article, the percentage of patients whose outcomes were classified as good to excellent varied from 26 to 100 percent (mean of 64 percent) for the 31 articles.
Most patients who have surgery for lumbar spinal stenosis have had their symptoms for over a year. It is not a common surgical consideration within the first 3 months of symptoms. [66]
Reoperation rates after spinal stenosis surgery (which were reported in 25 of the articles) ranged from 0 to 21 percent (with a mean of 8 percent). However, the authors speculated that these rates probably underestimated the true reoperation rates because of some follow-up periods that were very short.
The attempted meta-analysis by Turner, Ersek, Herron, et al. [66] concluded that in patients with severe symptoms from lumbar spinal stenosis, decompressive laminectomy appears to be beneficial for many patients by reducing pain and increasing the ability to function and is probably associated with an acceptably low complication rate.
There are also some data showing that although short-term results from spinal stenosis surgery may be good for most patients, for many patients there may be a progressive deterioration over time. A case series by Katz, Lipson, Larson, et al., [348] which followed 88 patients over age 55 who had decompressive laminectomy for symptoms of degenerative spinal stenosis, found that 89 percent of patients reported good outcomes (defined as absence of severe pain and no repeat operations) at 1-year follow-up, but only 57 percent of patients reported good outcomes at 3- to 6-year follow-ups.
Potential Harms and Costs.
Complications were also reviewed in the Turner, Ersek, Herron, et al. [66] meta-analysis. Death as a direct result of the surgery was rare, with a mean in-hospital mortality of 0.32 percent. Other reported complications of spinal stenosis surgery included dural tears (mean 0.32 percent), deep infection (mean 5.91 percent), superficial infection (mean 2.3 percent), and deep vein thrombosis (mean 2.78 percent).
The complication rate for spinal stenosis surgery is 10-15 percent, with half the complications being serious or life-threatening problems. These complications can result from the general anesthetic, the spinal problem itself, or coexisting medical problems. The high rate of complications may be because of the older age of this group.
Surgery for spinal stenosis is considered expensive.
Summary of Findings.
No RCTs were found comparing surgery with nonsurgical treatment for spinal stenosis. Symptoms of severe and persistent spinal stenosis may either remain the same, gradually worsen, or improve with time. The duration of symptoms for most patients who have surgery for lumbar spinal stenosis exceeds 1 year. This surgery is not commonly considered within the first 3 months of symptoms.
For patients with a history of severe and persistent symptoms of neurogenic claudication who undergo spinal stenosis decompressive laminectomy, the most likely outcomes are less leg pain and improved walking tolerance. However, there is some indication that these results tend to deteriorate over time.
The potential for serious complications from this procedure is considered to be acceptably low, although the rate is higher than for other procedures primarily because this operation is usually done in older individuals.
Spinal Fusion
Panel findings and recommendations:
Lumbar spinal fusion surgeries use bone grafts, and are sometimes combined with metal devices, to produce a rigid connection between two or more adjacent vertebrae. The therapeutic objective of spinal fusion surgery for patients with low back problems is to prevent any movement in the intervertebral spaces between the fused vertebrae, thereby reducing pain and any neurologic deficits. Various theoretical rationales are given for the use of fusion in patients with low back problems. One theory postulates that in cases of significant spinal instability (abnormally increased motion at an intervertebral level), fusion prevents painful compression of the neural structures. Another controversial theory holds that, in some cases, back symptoms arise from the disc itself and fusion relieves symptoms by greatly reducing forces compressing the disc.
Literature Reviewed
Of the 129 articles screened for this topic, 3 met criteria for review. [346], [349], [350] In addition, a meta-analysis article was reviewed. [351] Other articles contained information used by the panel, but did not meet article selection criteria. [352]- [356]
Evidence on Efficacy
One RCT evaluated the rate of fusion with and without Knodt rods in patients with a diagnosis of multiple level foraminal stenosis. [349] All patients were treated by wide decompressive laminectomy, foramenotomy and bilateral-lateral fusion from L3 to the sacrum. The rates of fusion, patient-reported functional status, and the lengths of postoperative hospital stays were not significantly different between the two groups.
A controlled trial by Herkowitz and Kurz [346] compared laminectomy with and without fusion in patients with chronic symptoms (mean symptom duration 3.0 years) who did not improve after nonoperative treatment and who had a positive imaging finding (myelogram and either CT or MRI) consistent with degenerative spondylolisthesis and spinal stenosis. Internal fixation using metal devices was not done as part of the fusion procedure. Following surgery, the fusion group reported significantly greater pain relief in the back and legs than did the nonfusion group. At mean follow-up of 3.0 years, excellent or good outcome rates were significantly greater for the fusion group than for the nonfusion group (96 percent compared with 44 percent).
The third study meeting review criteria was a nonrandomized trial comparing laminectomy with and without Knodt rod fusion in patients with chronic symptoms, leg pain or neurologic deficit, who did not improve after 3 months of conservative care and who had a positive imaging finding (EMG and myelogram or CT) for a herniated disc. [350] At long-term follow-up (mean follow-up time of 4.9 years for the fusion group and 3.7 years for the nonfusion group), the percentages of patients reporting satisfactory results (excellent or good) were not significantly different between the two groups. There are serious design problems with this study, such as the fusion group having a significantly longer mean duration of preoperative symptoms: 5.7 years compared with 1.3 years.
An attempted meta-analysis on this topic [351] found only four nonrandomized studies comparing surgery with and without fusion for herniated disc [350], [353], [354], [356] Three of the four trials reported no significant difference in results between the two groups. One trial did report significantly better results with fusion, but the treatment groups were not comparable. The fusion group had significantly more abnormal findings on x-ray, fewer positive straight leg raising tests, longer duration of pain, and fewer workers' compensation patients. [356]
Potential Harms and Costs
Turner, Ersek, Herron, et al. [351] indicated that complications are frequent with lumbar spinal fusions. Based on a review of a large case series, the mean rates for the most common reported complications were 7.3 percent for instrumentation failure and 10.8 percent for bone graft donor site pain. The mean rates for other complications were 0.2 percent for in-hospital mortality, 1.5 percent for deep infection, 1.6 percent for superficial infection, 3.7 percent for deep vein thrombosis/ thrombophlebitis, 2.2 percent for pulmonary embolus, 2.8 percent for neural injury, 2.0 percent for graft extrusion, and 8.7 percent for other complications. Spinal fusion is also considered an expensive procedure.
Summary of Findings
There appears to be no good evidence from controlled trials that spinal fusion alone is effective for treatment of any type of acute low back problems in the absence of spinal fractures or dislocation. In the opinion of the panel, there may be two conditions where spinal fusion could be effective. The first is in cases of combined degenerative spondylolisthesis, stenosis, and radiculopathy where patients have decompressive laminectomy for spinal stenosis symptoms. The second situation is in some young patients (generally under age 30) with significant spondylolisthesis and severe leg pain who may receive some benefit from stabilization procedures, although this has not been proven in controlled trials.
Although the usual reasons stated for doing spinal fusion for degenerative problems are instability of the spine and disc disease, there is lack of scientific agreement on how to define spinal instability. Spondylolisthesis is often implicated as a cause of instability, but it may or may not have any detectable abnormal motion and the extent to which this contributes to low back symptoms is controversial. Moreover, there is no good evidence that patients who undergo fusion will return to their prior functional level. It appears that fusion is not commonly considered for adults within the first 3 months of symptoms except for fracture or dislocation. [346], [350]
Panel findings and recommendations:
Social, economic, and psychological factors have been reported to be more important than physical factors in affecting the symptoms, response to treatment, and long-term outcomes of patients with chronic low back problems. [357] There are indications that such nonphysical factors may affect clinical outcomes for patients with acute low back symptoms (Attachment A5). A heightened awareness among clinicians to the way such factors may affect a patient's response to symptoms and treatment is therefore warranted.
|
|
|
A5. Further care of acute low back problems |
Literature Reviewed
None of the articles screened about psychosocial factors in the assessment and treatment of low back problems were controlled trials and therefore do not meet panel review criteria for adequate evidence about efficacy. Five articles, however, that included prospective cohort studies contained information considered useful to the panel. [23], [50], [358] - [360]
Evidence of Efficacy
One large prospective study [358] of asymptomatic individuals at a worksite found premorbid nonphysical factors (i.e., measures of low work satisfaction and poor work performance reports) to be the best predictors of individuals reporting back problems at work. In a second study, [23] psychological variables measured early in the course of an acute low back episode did not predict outcome, although other nonphysical factors, such as educational level and perception of both job characteristics and "fault" concerning the back problem, were strong predictors of outcome. A population-based study [359] also suggested that psychosocial issues affect how individuals with low back symptoms make decisions about working.
Several studies have detected a strong correlation between the outcome of lumbar spine surgery and the preoperative psychological status of the patient. [50], [360]
Summary of Findings
The panel found evidence that psychological, social, and economic (nonphysical) factors can alter the response to symptoms and to treatment (including surgery) among patients with acute low back problems. While such nonphysical factors have been shown to affect outcomes, specific and effective interventions to address these factors and alter patient outcomes have yet to be defined. No studies that directly evaluated interventions aimed at psychosocial factors among patients with acute low back problems were found.
Given such limited information, the panel was55555 unable to recommend specific assessment tools or interventions focusing on psychosocial factors potentially important for patients with acute low back problems. Recognizing the impact such nonphysical issues can have on outcomes, however, the panel recommended that clinicians be aware of these factors, especially in patients whose recovery of activity tolerance following an acute low back problem seems delayed. Further research is needed to define specific methods of detecting nonphysical factors as well as interventions that might improve outcomes for those patients slow to recover from acute low back problems.
Acute low back problem
Activity limitation(s) due to low back symptoms (back pain or back-related leg pain) present less than 3 months.
Back school
A structured educational program, usually in a group setting, designed to inform patients about low back problems.
Biofeedback
The use of auditory and visual signals reflecting a patient's muscular activity to allow the patient to facilitate or extinguish this muscle action. In patients with low back pain, the objective is to reduce pain by reducing muscle tension.
Cauda equina syndrome
Compression (usually due to the extrinsic pressure of a massive, centrally herniated disc) on a sheaf of nerve roots from the lower cord segments, often resulting in bilateral motor weakness of the lower extremities, saddle anesthesia, and urine retention or incontinence from loss of sphincter function.
Chemonucleolysis
The injection of a proteolytic enzyme (e.g., chymopapain) into the herniated nucleus pulposus of a disc.
CT-myelography
Computerized tomography done after contrast media has been injected into the dural sac.
Diathermy
Therapeutic elevation of the temperature of deep tissues by means of high frequency shortwave or microwaves.
Discography
The injection of a water-soluble imaging material directly into the nucleus pulposus of a disc to assess the extent of disc damage and characterize the pain response.
Discectomy
The surgical removal of all or part of a herniated intervertebral disc compressing a nerve root. When microscopic or visually aided surgical techniques are used, this procedure is referred to as microdiscectomy. The procedure can also be done through a small incision using indirect visualization (percutaneous discectomy).
Electromyography (EMG)
An examination of the electrical activity of a motor unit, useful in determining the site of injury in a peripheral nerve and in detecting spinal nerve root lesions as well as primary muscle diseases. Needle EMG involves the insertion of needle electrodes into muscle; surface EMG uses surface electrodes instead of needle insertion.
Ergonomics
The study of the proper and efficient use of the body in work and recreation, including the design and operations of machines and the physical environment.
F-wave tests
The use of electrodiagnostic equipment to measure motor conduction through nerve roots, most frequently to assess proximal neuropathies.
Facet joints
Synovial joints formed by the facets on the articular processes of contiguous vertebrae.
H-reflex tests
The use of electrodiagnostic equipment to measure sensory conduction of a stimulus through nerve roots that then evoke a motor reflex, commonly employed to assess S1 radiculopathy.
Herniated disc
Herniation of the central gelatinous material (nucleus pulposus) of an intervertebral disc through its fibrous outer covering (annulus fibrosis).
Nerve conduction studies
Tests of peripheral nerves performed by stimulating the nerve at one point and measuring the action potential either at another point along the nerve (sensory conduction) or of the muscle innervated by the nerve (motor conduction).
Neurogenic claudication.
Symptoms of leg pain (and occasionally weakness) on walking or standing, relieved by sitting or spinal flexion, related to neural compression, usually spinal stenosis.
Pain drawings
Drawings by patients depicting the severity, type, and location of their pain as a technique for assessing psychological involvement in the pain complaints.
Radiculopathy
Dysfunction of a nerve root often caused by compression of the root. Pain, sensory impairment, weakness or depression of deep tendon reflexes may be noticed in the distribution of nerves derived from the involved nerve root.
Saddle anesthesia
Loss of sensation in the skin over the perineum indicative of dysfunction of sacral nerve roots.
Sciatica.
Pain radiating down the leg(s) below the knee along the distribution of the sciatic nerve, usually related to mechanical pressure and/or inflammation of lumbosacral nerve roots.
Sensory evoked potentials (SEP).
The use of electrical stimuli applied to specific nerves or dermatomes to assess the normalcy of nerve responses.
Spinal manipulation
Manual therapy for symptomatic relief and functional improvement of the back in which loads are applied to the spine using short or long lever methods. The selected spinal joint is moved to its end range of voluntary motion, followed by application of an impulse load.
Spinal stenosis
A narrowing of the spinal canal that may produce a bony constriction of the cauda equina and the emerging nerve roots.
Spondylolisthesis
Forward subluxation of the body of a lumbar vertebra on the vertebra below.
Spondylolysis
A fracture or cleft in the vertebral body, often through the posterior vertebral arch, loosening its normally firm attachment to contiguous vertebrae.
Straight leg raising (SLR)
A procedure of stretching the sciatic nerve to see if radicular symptomatology is reproduced. Each hip is alternately flexed with the knee extended; the extent to which each leg can be lifted is noted. Reproduction of the patient's sciatica when the unaffected leg is lifted is evidence of a positive "crossed" straight leg raising test.
Thermography.
A procedure that images the infrared radiation (heat) emitted from body surfaces. In patients with low back problems, thermographic image patterns of the back and lower extremities are measured.
Transcutaneous electrical nerve stimulation (TENS)
A small battery-operated device, worn by the patient, which provides continuous electrical pulses via surface electrodes with the goal of providing symptomatic relief by modifying pain perception.
Traction
When used for low back problems, intermittent or continuous force is applied along the axis of the spine in an attempt to elongate the spine. The type most commonly used for low back problems is pelvic traction in which a girdle around the patient's pelvis is attached to weights hung at the foot of the bed.
Trigger point
A well localized point of tenderness. In low back problems, these points are usually located in the paravertebral areas.
Visual analog scales.
A visual means by which a patient can quantify pain. The patient marks a point corresponding to the intensity of his pain on a line, one end of which represents no pain and the other end, severe, incapacitating pain.
Stanley J. Bigos, MD, Chair
Orthopedic Surgery
Dr. Bigos is Professor of Orthopedic Surgery and Environmental Health at the University of Washington School of Medicine and founder and director of the Spine Resource Clinic in Seattle. He is the author of numerous articles and book chapters focusing on back problems in industry and the management of back pain. He has contributed to a new method of spine evaluation included in the American Medical Association's "Guidelines to Evaluate Permanent Impairment, 4th edition, 1993" and also serves as Consultant to the Clinical Standards Advisory Group of the British Department of Health. Among his many honors, Dr. Bigos received from the American Academy of Orthopaedic Surgeons in 1991 the Kappa Delta Award for Orthopedic Excellence for his sentinel work on industrial back problems.
Rev. O. Richard Bowyer
Consumer
Rev. Bowyer has experienced low back pain for many years. He is campus minister at Fairmont State College, West Virginia, and also serves on the Board of Directors and Quality Assurance Committee of the Monongahela Valley Association of Health Centers. From 1981-1993 he was a consumer member of the West Virginia Board of Medicine and served as chairperson of the Board's Complaints Committee.
G. Richard Braen, MD
Emergency Medicine
Dr. Braen is a practicing emergency physician at Buffalo General Hospital and Professor and Chairman of the Department of Emergency Medicine at State University of New York, Buffalo. Certified by both the American Board of Emergency Medicine and the American Board of Internal Medicine, he has served on several guideline panels established by the American College of Emergency Physicians. He is currently President of the American Board of Emergency Medicine.
Kathleen Brown, PhD, RN
Occupational Health Nursing
Dr. Brown is Professor in the School of Nursing of the University of Alabama at Birmingham and director of Occupational Health Nursing for the NIOSH-funded Educational Resource Center for Occupational Health and Safety. Her research and publications have focused on the cost-effectiveness of back school interventions and the effect of back school education and exercise on back-injured municipal workers. She is principal investigator of an NIH-funded study of worksite education and exercise to prevent back injuries.
Richard Deyo, MD, MPH
Internal Medicine
Dr. Deyo, a general internist, is Professor in the Departments of Medicine and Health Services at the University of Washington School of Medicine, and staff physician at the Seattle Veterans Affairs Medical Center. He is principal investigator of the low back pain Patient Outcome Research Team (PORT) and has published widely on the diagnosis and treatment of low back problems in primary care and on the measurement of quality-of-life and outcomes of surgery for patients with back pain.
Scott Haldeman, DC, MD, PhD
Neurology/Chiropractic
Dr. Haldeman is trained in chiropractic and is board certified in neurology, neurophysiology and electrodiagnosis. He is an Associate Clinical Professor of Neurology at the University of California, Irvine, and an Adjunct Professor at Los Angeles Chiropractic College. He is past president of the North American Spine Society and the North American Academy of Manipulative Medicine and has published widely in the fields of electrodiagnosis, spinal manipulation, and back pain.
John L. Hart, DO
Rehabilitation Medicine
Dr. Hart serves as Director of Outpatient Physical Medicine and Rehabilitation at Still Regional Medical Center in Columbia, Missouri. His research interests include nonoperative treatment of herniated discs and the relationship of employee/employer interactions to the symptoms of low back pain.
Ernest W. Johnson, MD
Physical Medicine/Rehabilitation
Dr. Johnson served for 25 years as Chair of the Department of Physical Medicine and Rehabilitation at the Ohio State University College of Medicine before assuming his present position as Professor and Associate Dean for External Affairs. He is past president of the American Academy of Physical Medicine and Rehabilitation, the Association of Academic Physiatrists, and the American Association of Electrodiagnostic Medicine. The author of numerous articles on electromyography, he serves as Chair of the American Board of Electrodiagnostic Medicine.
Robert Keller, MD
Orthopedic Surgery
Dr. Keller serves as Executive Director of the Maine Medical Assessment Foundation and is a member of the Council on Health Policy and Practice of the American Academy of Orthopaedic Surgeons. He is co-investigator of the Patient Outcomes Research Team (PORT) evaluating low back pain and surgical outcomes and has published on the subject of small area analysis and physician behavior change. A past president of the Maine Medical Association, he is an Adjunct Professor of Community and Family Medicine and Surgery in the Dartmouth Medical School.
Daniel Kido, MD, FACR
Radiology
Dr. Kido is a Professor of Radiology and Director of the Neuroradiology Section of the Mallinckrodt Institute of Washington University School of Medicine in St. Louis, Missouri. His research and publications have focused on the assessment of imaging techniques to evaluate low back pain, including MRI, CT, and myelography. He has also compared invasive and noninvasive imaging procedures of the low back, documenting frequency of complications.
Matthew H. Liang, MD, MPH
Internal Medicine/Rheumatology
Dr. Liang is an Associate Professor in the Departments of Medicine and Rheumatology at Harvard Medical School. He also serves as medical director of rehabilitation services at the Brigham and Women's Hospital in Boston. His major research interests include outcome assessment of low back problems, cost-effectiveness of diagnostic procedures, and outcomes of spinal stenosis surgery.
Roger M. Nelson, PT, PhD
Physical Therapy
Dr. Nelson is Professor and Chairman of the Department of Physical Therapy at the Thomas Jefferson University College of Allied Health Sciences. His clinical interests include electromyography and measurements of outcome and satisfaction of low back pain patients. He is a contributor to the National Institute of Occupational Safety and Health (NIOSH) Low Back Atlas on the subject of tests and measures for the assessment of low back pain.
Margareta Nordin, RPT, Dr Sci
Orthopedic Research
Dr. Nordin is Research Associate Professor and Director of the Occupational and Industrial Orthopaedic Center of the Hospital for Joint Diseases in New York City. Her primary research interest is the prevention of chronicity among patients with low back pain. She has published extensively on the biomechanics, ergonomics, and early care of low back pain.
Bernice D. Owen, PhD, RN
Community Health Nursing
Dr. Owen is a Professor in the School of Nursing of the Center for Health Sciences, University of Wisconsin, Madison. Her work as a teacher and researcher has focused on back stress among health care personnel and the reduction of physical demands on the back in occupational settings. She currently serves as a consultant on back injury reduction programs to hospitals, long-term care facilities, and home care agencies.
Malcolm H. Pope, DrMedSc, PhD
Orthopedic Research/Biomedical Engineering
Dr. Pope is Professor of Biomedical Engineering at the University of Iowa and serves as Director of the Iowa Spine Research Center. Before coming to Iowa, he was Director of Orthopaedic Research at the University of Vermont. His research and numerous publications have focused on the biomechanics of low back pain, ergonomics, and the primary and secondary prevention of low back problems.
Richard K. Schwartz, MS, OTR, FSR
Occupational Therapy
Mr. Schwartz has treated work-related injuries since 1972. He is currently in private practice as an occupational therapy consultant on injury prevention, ergonomics, and early return-to-work programs. Before 1992 he was Associate Professor and Chairman of Occupational Therapy at the University of Texas Health Science Center at San Antonio.
Donald H. Stewart, Jr.,
MD Neurosurgery
Until his retirement in 1993, Dr. Stewart was in private practice as a neurosurgeon in Syracuse, New York. He also served as Clinical Assistant Professor of Neurosurgery at the State University of New York, Syracuse. He has published widely on medical economics and medical liability.
Jeff Susman, MD
Family Practice
Dr. Susman is Associate Professor, Director of Primary Care, and Vice Chairperson of the Department of Family Practice at the University of Nebraska Medical Center. A member of the American Academy of Family Physicians' Task Force on Clinical Policies, he is interested in clinical decisionmaking by physicians and the effects of guidelines on health provider behavior.
John J. Triano, MA, DC
Chiropractic
Dr. Triano is a staff chiropractic physician and a clinical research scientist at the Texas Back Institute in Plano, Texas. He coordinates the work of interdisciplinary teams in the rehabilitation of patients with spinal pain and conducts research on spine biomechanics and the outcomes of patients treated for spinal problems. He has served as a consultant to the U.S. Department of Labor and NIOSH training programs and is a Professor at the National College of Chiropractic, Lombard, Illinois.
Lucius C. Tripp, MD, MPH, FACPM
Industrial Medicine/Neurosurgery
Dr. Tripp, a neurosurgeon, is board certified in Occupational Medicine and Addiction Medicine. He serves as Medical Director of the General Motors-Henry Ford Hospital Rehabilitation Center in Warren, Michigan, and is actively involved in research on the prevention of back injury and restoration of function in patients with back pain. He is a member of the Board of Directors of the American College of Occupational and Environmental Medicine.
Dennis C. Turk, PhD
Psychology
Dr. Turk is a Professor in the Departments of Psychiatry and Anesthesiology at the University of Pittsburgh School of Medicine. He serves as Director of the University's Pain Evaluation and Treatment Institute, a large interdisciplinary facility that annually evaluates and treats over 1,500 new patients, the majority of whom have back pain. His current research is directed toward examination of the role of psychological factors in back pain and the accompanying disability.
Clark Watts, MD, JD
Neurosurgery
Dr. Watts is a Professor of Neurosurgery at the University of Texas Health Science Center at San Antonio. As editor of Neurosurgery from 1982-1987, he was responsible for evaluating and publishing research on the care of low back problems. His own research has focused on the nature of discogenic pain and the clinical management (operative and nonoperative) of low back problems.
James N. Weinstein, DO
Orthopedic Surgery
Dr. Weinstein is a Professor in the Departments of Orthopaedic Surgery and Biomedical Engineering and is Director of the Spine Diagnostic and Treatment Center at the University of Iowa Hospitals and Clinics. His research has focused on the basic mechanisms of pain and aging, the diagnosis and treatment of spinal tumors, and the evaluation of outcomes for patients with low back pain. He is currently Editor-in-Chief of the journal Spine.
Project Directors
John P. Holland, MD, MPH
University of Washington
Seattle, Washington
John S. Webster, MD
Naval Regional Medical Center
San Diego, California
Consultants
Michele C. Battie, PhD, PT
Orthopedic Research
University of Washington
Seattle, Washington
Claire Bombardier, MD, FRCP
Rheumatology/Clinical Epidemiology
University of Toronto
Toronto, Ontario, Canada
Nortin M. Hadler, MD
Rheumatology
University of North Carolina
Chapel Hill, North Carolina
Alf L. Nachemson, MD, PhD
Orthopaedic Surgery
Göteborg University
Göteborg, Sweden
Gordon Waddell, MD
Orthopaedic Surgery
Western Infirmary
Glasgow, Scotland
Methodologists
David L. Schriger, MD, MPH
UCLA Medical School
Los Angeles, California
Paul G. Shekelle, MD, MPH
Department of Veterans Affairs Medical Center
West Los Angeles, California
Panel Staff
Mary M. Webster, MA
Seattle, Washington
Laura Novell
St. Louis, Missouri
Keld Vaegter, MD
Ralix, Sweden
AHCPR Staff
David Lanier, MD, MFA
Project Officer
Randie A. Siegel
Managing Editor
Harriet V. Bennett
Karen Carp
Public Affairs Specialists
Lucien Abenhaim, MD, MSc, ScD
McGill University
Montreal, Quebec, Canada
Gad Alon, PhD, PT
University of Maryland
Department of Physical Therapy
Baltimore, Maryland
Michael Andary, MD
Michigan State University
College of Osteopathic Medicine
East Lansing, Michigan
Gunnar B.J. Andersson, MD, PhD
Rush-Presbyterian-St. Luke's Medical Center
Chicago, Illinois
Howard A. Balduc, DC
American Chiropractic Association
Arlington, Virginia
Judith C. Bautch, PhD, RN, CS
University of Wisconsin School of Nursing
Madison, Wisconsin
James R. Bean, MD
Neurosurgical Associates
Lexington, Kentucky
Alfred O. Berg, MD, MPH
University of Washington
Seattle, Washington
Stephen Blood, DO
American Academy of Osteopathy
Indianapolis, Indiana
Wilbur J. Boike, MD
Center for Comprehensive Back Care
Flint, Michigan
Richard H. Borman, MD
University of California
San Diego, California
Albert M. Brady, MD
Harris Methodist Health System
Fort Worth, Texas
Phillip O. Bridenbaugh, MD
University of Cincinnati Medical Center
Cincinnati, Ohio
Jerry M. Calkins, PhD, MD
University of Arizona Department of Anesthesiology
Phoenix, Arizona
J. David Cassidy, DC, PhD
Royal University Hospital Department of Orthopaedics
Saskatoon, Saskatchewan, Canada
C. Richard Chapman, PhD
University of Washington Department of Anesthesiology
Seattle, Washington
Steven G. Charapata, MD
Pain Management Associates
Kansas City, Missouri
Joy White Danches, MOT, OTR
Visionary Management, Inc.
Dallas, Texas
Marsha Courville Davis, MSN, RN, CRRN
Association of Rehabilitation Nurses
Jackson, Mississippi
Douglas E. DeGood, PhD
University of Virginia Health Sciences Center
Charlottesville, Virginia
Anthony Delitto, PT, PhD
University of Pittsburgh
Pittsburgh, Pennsylvania
Mark A. Doyne, MD, FACPE
Texas Back Institute
Dallas, Texas
Daniel A. Dyrek, MS, PT
Massachusetts General Hospital
Boston, Massachusetts
Frank Eismont, MD
University of Miami School of Medicine
Miami, Florida
Maury R. Ellenberg, MD, FACP
Wayne State University School of Medicine
Detroit, Michigan
Julia Faucett, RN, PhD
University of California
San Francisco, California
Morris A. Fisher, MD
Loyola University Stritch School of Medicine
Chicago, Illinois
Gary M. Franklin, MD, MPH
University of Washington Occupational Epidemiology
Seattle, Washington
Todd D. Gastaldo, DC
Private Chiropractic Research
Sunnyvale, California
Sharon J. Gates
The Graduate Hospital
Philadelphia, Pennsylvania
Michael Goertz, MD, MPH
Airport Medical Clinic
Minneapolis, Minnesota
Michael K. Greenberg, MD
Uniformed Services University of the Health Sciences
Bethesda, Maryland
J. Eric Griffiths, DC
Wheat Ridge Chiropractic Center
Denver, Colorado
Daniel T. Hansen, DC, FICC
Private Practice of Chiropractic
Olympia, Washington
Dennis L. Hart, PhD, PT
Rehability Corporation
Falls Church, Virginia
Jodie K. Haselkorn, MD, MPH
Veterans Affairs Medical Center
Seattle, Washington
Stanley A. Herring, MD
Puget Sound Sports and Spine Physicians
Seattle, Washington
Paul D. Howard, PhD, PT
Thomas Jefferson University
Philadelphia, Pennsylvania
Thomas E. Hyde, DC, CCSP
American Chiropractic Association Sports Council
North Miami Beach, Florida
Susan J. Isernhagen, PT
Isernhagen & Associates, Inc.
Duluth, Minnesota
Manucher J. Javid, MD
University of Wisconsin
Department of Neurosurgery
Madison, Wisconsin
John H. Juhl, DO
American Academy of Osteopathy
New York, New York
Neil Kahanovitz, MD
Anderson Clinic
Arlington, Virginia
Robert D. Kerns, PhD
West Haven VA Medical Center
Yale University
West Haven, Connecticut
Myron M. LaBan, MD, FACP
William Beaumont Hospital Department of Physical Medicine and Rehabilitation
Royal Oak, Michigan
Ruth A. Larkin, RN
North Colorado Medical Center
Greeley, Colorado
Casey K. Lee, MD
New Jersey Medical School Department of Orthopaedics
Newark, New Jersey
Daniel Lessard
Back Health Medical Centers
Seattle, Washington
Stephen M. Levin, MD
American Academy of Orthopaedic Medicine
Vienna, Virginia
Philipp M. Lippe, MD, FACS, FACPM
American Academy of Pain Medicine
Skokie, Illinois
Michael D. Lockshin, MD
National Institute of Arthritis and Musculoskeletal and Skin Diseases
National Institutes of Health
Bethesda, Maryland
John D. Loeser, MD
University of Washington
Seattle, Washington
Don M. Long, MD, PhD
Johns Hopkins University School of Medicine
Baltimore, Maryland
Sally L. Lusk, PhD, RN, FAAN
University of Michigan School of Nursing
Ann Arbor, Michigan
Norman J. Marcus, MD
New York Pain Treatment Program
Lenox Hill Hospital
New York, New York
Stephen C. Marini, MS, DC, PhD
Pennsylvania College of Chiropractic
Philadelphia, Pennsylvania
Tom G. Mayer, MD
Southwestern Medical School Department of Orthopedics
Dallas, Texas
George B. McClelland, DC
Foundation for Chiropractic Education and Research
Arlington, Virginia
William A. McIlwain, MD, FACS
Bristol Regional Medical Center
Bristol, Tennessee
William C. Meeker, DC, MPH
Palmer College of Chiropractic-West
San Jose, California
Christine Miaskowski, RN, PhD
University of California
San Francisco, California
Edward H. Mills, MD
U.S. Department of Labor
Michael Mittelmann, MD
Aetna Life and Casualty
Hartford, Connecticut
Vert Mooney, MD
University of California
San Diego, California
Mary T. Muffroid, PhD, PT
University of Vermont
Burlington, Vermont
Albert M. Murtland, MD
Guthrie Clinic
Sayre, Pennsylvania
David E. Nestor, MS, PT, ECS
U.S. Public Health Service
Rochester, Minnesota
E.J. Nordby, MD
University of Wisconsin Medical School
Madison, Wisconsin
Jane E. Parker-Conrad, PhD, RN
Walters State College
Morristown, Tennessee
Richard Payne, MD
University of Texas M.D. Anderson Cancer Center
Houston, Texas
Reed B. Phillips, DC, PhD
Los Angeles College of Chiropractic
Whittier, California
William R. Phillips, MD, MPH
University of Washington
Seattle, Washington
Vern Putz-Anderson, PhD
National Institute for Occupational Safety and Health
Cincinnati, Ohio
Jan K. Richardson, PT, PhD
Slippery Rock University School of Physical Therapy
Pittsburgh, Pennsylvania
Hubert L. Rosomoff, MD, DMedSc
University of Miami School of Medicine
Department of Neurological Surgery
Miami, Florida
Renee Steele Rosomoff, RN, MBA, CRC
University of Miami Comprehensive Pain and Rehabilitation Center
Miami Beach, Florida
Michel Rossignol, MD, FRCPC
McGill University
Montreal, Quebec, Canada
Donald Sheffel, MD
Memorial Hospital Division of Neurosurgery
Hollywood, Florida
Dennis Shubert, MD, PhD
Neurosurgical Associates
Bangor, Maine
Stover H. Snook, PhD
Liberty Mutual Insurance Company
Hopkinton, Massachusetts
Jody L. Snow, PT
Sacred Heart Medical Center
The Rehabilitation Center
Spokane, Washington
Dan M. Spengler, MD
Vanderbilt University Medical Center Department of Orthopaedics and Rehabilitation
Nashville, Tennessee
Richard L. Stieg, MD
University of Colorado Health Sciences Center Department of Neurology
Denver, Colorado
Rand S. Swenson, DC, MD, PhD
Dartmouth Medical School
Hanover, New Hampshire
Robert L. Swezey, MD, FACP, FACR
Arthritis & Back Pain Center
Santa Monica, California
Peter J. Vicente, PhD
Good Samaritan Hospital Pain Rehabilitation Center
Cincinnati, Ohio
Nicholas E. Walsh, MD
University of Texas Health Science Center
San Antonio, Texas
Barbara S. Webster, RPT, PA-C
American Academy of Physician Assistants
Alexandria, Virginia
Debra Weiner, MD
Duke University Medical Center
Durham, North Carolina
Arthur H. White, MD
San Francisco Spine Institute
San Francisco, California
John W. Wickenden, MD
Penobscot Bay Medical Center
Rockport, Maine
Sam W. Wiesel, MD
Georgetown University Medical Center Department of Orthopaedics
Washington, DC
Arthur Winter, MD, FICS
University of Medicine and Dentistry of New Jersey
New Jersey Neurological Institute
Livingston, New Jersey
Hansen A. Yuan, MD
State University of New York
Syracuse, New York
1 Being listed in this section does not necessarily imply endorsement of the guideline products.
Douglas A. Benner, MD
Kaiser Permanente
Oakland, California
James E. Blessman, Jr., MD, MPH
Wayne State University
Detroit, Michigan
Michael Erdil, MD
Industrial Medical Care Center
Hartford, Connecticut
Don C. Fisher, MD, MS
Presbyterian Occupational Health Network
Albuquerque, New Mexico
Garry A. Goldstein, MD
General Motors Corporation
Wilmington, Delaware
Robert J. Gorman, MD, MPH
Park Nicollet Medical Center
Minneapolis, Minnesota
Rowland G. Hazard, MD
University of Vermont
Burlington, Vermont
Timothy J. Key, MD, MPH
University of Alabama School of Medicine
Birmingham, Alabama
Ron R. Loeppke, MD, MPH
Corporate Health and Medical Programs, Inc.
Greeley, Colorado
Christel Mottur-Pilson, PhD
Internal Medicine Center to Advance Research & Education (IMCARE)
Washington, DC
Julie Graves Moy, MD, MPH
Baylor College of Medicine
Houston, Texas
Dennis A. Plante, MD
University of Vermont
Burlington, Vermont
Louis Sportelli, DC
Private Practice
Palmerton, Pennsylvania
1 Being listed in this section does not necessarily imply endorsement of the guideline products.
Four discussion handouts for patients are provided. They are sufficiently specific to address a full range of patient concerns. The patient's focus tends to change during treatment. Early concerns may focus on comfort, or fear of potentially dangerous causes of low back pain. Later, questions about special studies, procedures, and diagnoses may arise. The few patients having trouble overcoming their activity limitations may have to consider the relative benefits either of conditioning more vigorously or of changing their activity goals. These handouts are not intended to stand alone for all patients. Rather, they are designed to foster the clinician's discussions with patients about important issues, as needed.
The news is good.
Your clinician has not found any dangerous causes for your back problem. Almost everyone has a low back problem at some time. In only one person out of 200 does the problem have a serious cause. A medical history and physical examination alone are very good at detecting these uncommon cases.
You should recover soon.
Nine out of 10 persons with low back problems recover within 1 month, and most recover even sooner. Therefore, an x-ray of your back or other tests at this time would only waste your time. If your recovery happens to be slower than normal, your clinician will then look further for a reason.
Even with back symptoms, you may be able to continue your usual activities. But you might have to slow your pace. Strenuous activity or heavy lifting could give you trouble. If you work outside the home, much depends on the kind of work you do. Office work may require few changes. On the other hand, if your job involves heavy labor-like a furniture mover-you will probably have trouble working as usual right away.
Age also makes a difference. As we age, so do our spines. Activities that require speed and strength become harder to do. This happens to many people by age 30, to most people by age 40, and to nearly everyone by age 50. Consider your age as you plan your daily tasks when recovering from a back problem.
You can ease your discomfort safely.
Your clinician will suggest safe ways for you to be more comfortable as you recover. But staying in bed is usually not the best thing. More than a few days in bed actually weakens your back and could cause your symptoms to last longer. Neither bed rest, medications, or any other remedies should be expected to do away with all the discomfort. It is important to be up and around as much as possible even if you are uncomfortable. The sooner you return to normal daily activities, the sooner your symptoms will disappear.
You may need to make changes in your daily activities.
Sitting may not be comfortable. Sitting is not dangerous, but it puts more stress on the back than standing. While recovering, try to spend less time sitting. To make sitting easier, support the curve of your lower back with a towel or small pillow. If possible, use a chair or other seat with a slightly reclining back.
Lifting.
Keep anything you must lift close to the belly button. Lifting a carton of milk or orange juice at arm's length can stress your back more than lifting 30 pounds held close to the body. Also try not to bend forward, twist, or reach when lifting.
Exercising can help your back.
Your health care provider may suggest safe exercises such as walking, swimming, or riding a stationary bike. If done correctly, these exercises do not stress the back any more than does sitting on the side of your bed (which is not dangerous). What exercising does is keep your back muscles from becoming weakened by not enough activity. In addition, exercise is good for your general health, can speed your recovery, and may help protect you from future back problems. As your symptoms lessen, daily exercise will make it easier for you to resume your normal activities.
Special tests may be needed.
If your back problem is slow to recover, your health care provider may consider special studies (tests) to find the reason. They may include blood tests; or an imaging study may be needed to view your spine. Nerve tests may help identify certain leg problems. The chances are good that your problem will not be serious. In only one person out of 200 do low back problems have a serious cause.
Why wait to do special studies?
You may have read or heard of tests like MRI, CAT scan, or myelogram. These are special imaging studies. They use special equipment to provide different views of body structures like your spine. You may wonder why your health care provider did not order these tests in the first place. There is a good reason. Imaging studies can be confusing. By themselves, they cannot tell the difference between possible causes of a back problem and common changes in the spine because of aging.
As we grow older, the spine changes. Almost half the population has aging changes in the spine as early as age 35. Yet most people who have such changes will not have a back problem lasting longer than 1 month. Remember that nine out of 10 people who have low back problems recover within 1 month. For these persons, imaging studies are unnecessary and confusion can be avoided. The tests could show a condition that is really not a problem and has no connection to back symptoms.
Imaging studies are seldom used alone. Surgery is never based on imaging studies alone. The studies could find something that is not really the cause of your problem. Before deciding whether imaging studies are needed, your health care provider should review your physical examination carefully. He or she may also do other kinds of tests to find evidence of a problem. Ask your health care provider to explain what tests are needed for you.
Table 1 lists a number of terms that are commonly used to describe (diagnose) the cause of low back symptoms. However, scientific studies have not been able to show a connection between these diagnoses and back symptoms. In addition, there is no evidence that these conditions benefit from surgery or other specialized forms of treatment.
When is surgery a choice?
If your back symptoms affect your legs and are not getting better, a herniated lumbar disc (what many people call a slipped disc) may be the reason. The disc can press on a nerve root in your back and can either irritate the nerve or affect its function. If tests show strong evidence that this is happening, surgery to take the pressure off of the nerve may speed your recovery.
If your health care provider tells you that surgery is a possibility, ask about your choices. Ask what would happen without surgery. Before agreeing to surgery, get a second opinion from another health care provider. Also, ask about the tests that were done to suggest that surgery is the best approach for your back symptoms. Table 2 lists some conditions or diagnoses that sometimes benefit from surgery or other special treatment.
Tests cannot always tell you the cause of your symptoms.
Medical science cannot always explain the exact cause of most common low back symptoms. But medical science is very good at finding out if you have a dangerous condition causing your symptoms. If your problem is not caused by a serious condition, you can continue looking forward to recovery.
Exercise is important.
Remember to continue to exercise as you were instructed by your health care provider and as described in Handout 1. It is important not to neglect your muscles. Exercise regularly!
| Annular tear | Adult spondylolysis | Myofascitis |
| Fibromyalgia | Disc syndrome | Strain |
| Spondylolysis | Lumbar disc disease | Facet syndrome |
| Degenerative joint disease | Sprain | Osteoarthritis of the spine |
| Disc derangement/disruption | Dislocation | Subluxation |
Leg pain due to herniated lumbar disc".
|
"Leg pain due to spinal stenosis."
|
"Leg pain with spondylolisthesis."
|
"Fracture or dislocation."
|
"Spinal arthritis."
|
By now your health care provider has given you the news that you can comfortably begin to get back to your daily activities. Even if you required surgery, you can now safely begin a specific, gentle exercise program to condition your body and your back muscles. This program will increase your back's ability to help you do the things you want and need to do.
Start with a simple, safe exercise such as walking, stationary bicycling, or swimming to build your general stamina. If you have been inactive, you may need to begin slowly and gradually increase your activity each day. Your health care provider will make specific recommendations for safe exercises that do not stress your back any more than sitting on the side of your bed. Exercise helps because it:
You also will find out what you can do easily and what takes more effort.
Reality about back problems.
Although your recovery seems slow, your symptoms will continue to decrease unless you are inactive. However, your back may never feel as young as it once did. This happens to many of us by age 30, most by age 40, and just about everyone by age 50. Back problems often are the first sign of aging. You may have noticed that few professional athletes can continue competing beyond age 40. While some people may be able to resume strenuous activity after back problems as they get older, it usually needs to be at a slower pace. Most people need to shift gears and make changes in goals and activities as they grow older. Even at a slower pace, exercise will help you to be able to tolerate more of your daily activities.
Once you have had an activity-limiting back problem that lasts more than a few weeks, there is a 40 to 60 percent chance of having another back problem within the next few years. However, symptoms usually are not as severe in future episodes as in the first episode.
Success.
As you begin to recover, the goal is to try to prevent back problems from returning or, if they do return, being severe. Success will depend upon two factors. The first is the condition of your protective muscles. The second is the activities you ask your back to tolerate.
Ignoring either of these factors usually means more back problems. For example, a coal miner can expect further problems because mining is so demanding on the back. By contrast, a member of royalty who never needs to stress his or her back but does no conditioning exercises also can expect regular back problems. How well YOU do in the future will depend on what kind of condition you are in and what you ask your back to do. The more easily you and your protective muscles tire, the greater the chance that your symptoms will return. Taking action to condition the protective muscles of your back can reduce your future problems.
Safe exercises that are good for you and your back.
Although exercises such as walking, stationary bicycling, or swimming are safe, you may feel some discomfort when you first start. After muscles become better conditioned, the soreness goes away. For example, during the winter when the weather is bad and many of us might stay indoors and be less active, the muscles of the back can lose their conditioning. When the first day of spring arrives and many of us go out to garden, the back may begin to ache when the out-of-condition protective muscles easily tire. Continuing such work daily over a few days or weeks reconditions the protective muscles so that they don't tire quite so easily, and the soreness disappears.
Remember that an increase in discomfort in an already painful back is common. But safe exercises (that involve less stress on the back than sitting on the side of the bed) should not harm your back. The shorter the time since beginning the conditioning, the greater the chance of increased soreness.
Conditioning requires regular activity.
Regular activity is essential to obtain the conditioning effect to protect your back. Conditioning is achieved by building up to 30 minutes of continuous walking, stationary cycling, or swimming at a targeted heart rate (Table 1) or through jogging for 20 minutes. Conditioning works best if combined with your normal, daily activities both at home and at work. Stay as active as possible and exercise every day.
Your health care provider may have suggested ways to modify your daily chores to reduce the chance of irritating your back. Such changes at home or work are usually temporary. They are intended to give you time to improve the condition of your protective back muscles so that you can resume most normal activities. Table 2 offers guidelines to your health care provider on work recommendations to allow you reasonable time to recondition your back. Long-term activity tolerance varies greatly from person to person. Age and overall health are important factors, too. Regular, mild exercise may be enough for some. Others may be able to return to vigorous activities at a slower pace.
Both your level of physical conditioning and the stresses you put on your back will determine how often you will have problems and how severe they become.
Conditioning usually requires daily work and commitment.
Be sure your activity goal is realistic and you know what it will take to achieve it. Once you are over your back symptoms, or after a month of general conditioning training, your health care provider may suggest that you begin doing back muscle, trunk, or extremity exercises to gain further tolerance for specific tasks.
If you have great difficulty resuming your previous daily routine, you may need to consider whether your old routine is realistic for you now.
|
| Symptoms | ||||
| Severe | Moderate | Mild | None | |
| Sitting[1] | 20 min | 50 min. | ||
| Unassisted lifting[2] | ||||
| Men | 20 lbs | 20 lbs | 60 lbs | 80 lbs |
| Women | 20 lbs | 20 lbs | 35 lbs | 40 lbs |
By now, your health care provider has made every effort to seek a medical reason for your continued activity limitation. You are well into the exercise program intended to condition your back for the activities you need to do. Unfortunately, for some people success is less easy and slower to achieve. If this is the case, there are many things to consider.
Age is important.
Few middle-aged persons have a back that is as strong as it was at age 18. Medical science presently cannot reverse the aging process that limits activities requiring both speed and strength. Young people may find it hard to accept these limitations. Older people commonly find it difficult to give up or alter activities they have been doing for a long time.
Some people continue to look for a cure when progress is slow. Such efforts rarely succeed. Consider a basketball star like Larry Bird. Money was surely no object in seeking a cure for his back problem. He could afford the most expensive medical care and conditioning programs. Nevertheless, he was forced to retire at age 34. His back could no longer tolerate the physical stress of basketball.
How many athletes in strenuous sports can compete beyond age 35 or 40? Very few! Most of us must adjust our activities as we age, regardless of occupation or level of physical conditioning, many by age 30, most by age 40, and just about all of us by age 50. Some people can continue strenuous activities into their older years, especially if they are able to do it at their own pace. Others may need to consider change.
Be realistic.
Ask yourself three key questions about your daily activity requirements:
If a reasonable exercise program is not helping you, there are several options: (1) You can choose to put up with discomfort and expect some setbacks. (2) You can begin a more time-consuming conditioning program. (3) You can change the pace of doing difficult activities. This may include a job change. People may use a combination of the three approaches.
Considering a job change is difficult, especially if back problems continue to limit your ability to do your work. Again, ask yourself this important question: "Is my activity goal realistic, or do I need to look at my options?" A review now might help you avoid a similar dilemma in the near or distant future, when increased age may work against you. Being a few years older sometimes makes a big difference in the chance of changing jobs. Some creative planning could benefit you now, or in the future, especially if your job activities present a problem.
When considering a job or career change, it is important to gather information from many sources. Some possibilities include private career counselors, local or State employment offices, and veterans' or consumer groups. You may also want to talk to someone working in the field.
Information is your ally.
Whether or not you explore job opportunities alone or with professional help, remember this important point:
Only you can find a way to adjust your life, your job, or your plans in a way that is right for you.
| A = Strong research-based evidence (multiple relevant and high-quality scientific studies). B = Moderate research-based evidence (one relevant high-quality scientific study or multiple adequate scientific studies*). C = Limited research-based evidence (at least one adequate scientific study* in patients with low back pain). D = Panel interpretation of information that did not meet inclusion criteria as research-based evidence. |
| * Met minimal formal criteria for scientific methodology and relevance to population and specific method addressed in guideline statement. |